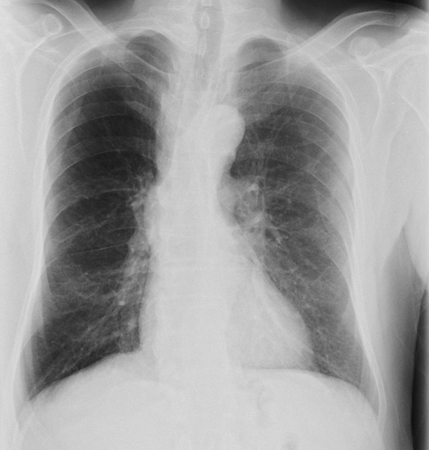
Summary
Definition
History and exam
Other diagnostic factors
- barrel chest
- hyperresonance on percussion
- distant breath sounds on auscultation
- poor air movement on auscultation
- wheezing on auscultation
- coarse crackles
- tachypnea
- asterixis
- distended neck veins
- lower-extremity swelling
- fatigue
- weight loss
- muscle loss
- headache
- pursed lip breathing
- cyanosis
- loud P2
- hepatojugular reflux
- hepatosplenomegaly
- clubbing
Risk factors
- cigarette smoking
- advanced age
- genetic factors
- lung growth and development
- white ancestry
- exposure to air pollution
- exposure to burning solid or biomass fuel
- occupational exposure to dusts, chemicals, pesticides, vapors, fumes, or gases
- male sex
- low socioeconomic status
- rheumatoid arthritis
Diagnostic tests
Tests to consider
- pulmonary function tests
- chest CT scan
- serial peak flow measurement
- sputum culture
- alpha-1 antitrypsin level
- exercise testing
- sleep study
- respiratory muscle function
- ECG
- echocardiogram
- blood eosinophil count
Treatment algorithm
Contributors
Authors
Manoochehr Abadian Sharifabad, MD

Fountain Valley Regional Medical Center
Fountain Valley
CA
Disclosures
MAS declares that he has no competing interests.
Acknowledgements
Dr Manoochehr Abadian Sharifabad would like to gratefully acknowledge Dr Jonathan P. Parsons and Dr Michael Ezzie, the previous contributors to this topic.
Disclosures
JPP has contributed at speakers' bureaus for GlaxoSmithKline, Inc., Schering-Plough, Inc., and AstraZeneca, Inc. ME declares that he has no competing interests.
Peer reviewers
Hormoz Ashtyani, MD, FCCP
Hackensack University Medical Center
Hackensack
NJ
Disclosures
HA declares that he has no competing interests.
Alejandro Comellas, MD
Clinical Professor of Internal Medicine-Pulmonary, Critical Care and Occupational Medicine
University of Iowa
Iowa City
IA
Disclosures
AC has received payments as a consultant for GSK and AstraZeneca. He also serves as a nonpaid consultant for VIDA.
William Janssen, MD
Assistant Professor of Medicine
National Jewish Medical and Research Center
University of Colorado Health Sciences Center
Denver
CO
Disclosures
WJ declares that he has no competing interests.
Francis Thien, MD, FRACP, FCCP
Associate Professor
Director of Respiratory Medicine
Eastern Health & Monash University
Victoria
Australia
Disclosures
FT declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Global Initiative for Chronic Obstructive Lung Disease (GOLD). Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: 2025 report. 2025 [internet publication].Full text
National Institute for Health and Care Excellence. Chronic obstructive pulmonary disease in over 16s: diagnosis and management. Jul 2019 [internet publication].Full text
Nici L, Mammen MJ, Charbek E, et al. Pharmacologic management of chronic obstructive pulmonary disease. An official American Thoracic Society clinical practice guideline. Am J Respir Crit Care Med. 2020 May 1;201(9):e56-69.Full text Abstract
Jacobs SS, Krishnan JA, Lederer DJ, et al. Home oxygen therapy for adults with chronic lung disease. An official American Thoracic Society clinical practice guideline. Am J Respir Crit Care Med. 2020 Nov 15;202(10):e121-41. [Erratum in: Am J Respir Crit Care Med. 2021 Apr 15;203(8):1045-6.]Full text Abstract
Reference articles
A full list of sources referenced in this topic is available here.
Use of this content is subject to our disclaimer