This page compiles our content related to skin cancer. For further information on diagnosis and treatment, follow the links below to our full BMJ Best Practice topics on the relevant conditions and symptoms.
Introduction
Relevant conditions
Merkel cell carcinoma | go to our full topic on Merkel cell carcinoma Merkel cell carcinoma is a rare, aggressive cutaneous neuroendocrine neoplasm that primarily affects white adults. Incidence increases with age and is highest among those >85 years of age.[5] Two distinct etiologies are recognized: exposure to UV radiation and oncogenic transformation by Merkel cell polyomavirus. Key risk factors are advancing age, immunosuppression, and light skin type. Diagnosis is confirmed with skin biopsy and histopathologic evaluation including immunohistochemistry. Occult metastasis is common, and sentinel lymph node biopsy and imaging are important tools for staging the disease. The tumor typically presents as an asymptomatic, rapidly growing, pink-to-violaceous or skin-colored dermal or subcutaneous nodule.[6] |
|---|---|
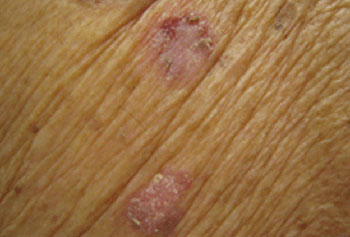
Basal cell carcinoma | go to our full topic on Basal cell carcinoma The most prevalent malignancy of the skin in fair-skinned adults in the world.[7][8] It typically presents as pearly papules and/or firm plaques; nonhealing scabs; small crusts and nonhealing wounds; plaques, nodules, and tumors with rolled borders; and/or papules with associated telangiectasias.[9][10][Figure caption and citation for the preceding image starts]: Nodular basal cell carcinoma on the cheek, on background of diffuse solar damage with marked solar elastosisFrom the collection of Dr Robert A. Schwartz [Citation ends]. |
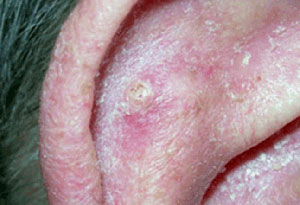
Squamous cell carcinoma (SCC) | go to our full topic on Squamous cell carcinoma (SCC) SCC is the proliferation of atypical, transformed keratinocytes in the skin with malignant behavior. Ranges from in situ tumors (Bowen disease) to invasive tumors and metastatic disease. Second most common nonmelanoma skin cancer worldwide, secondary to basal cell carcinoma.[8] Patients commonly present with a new or englarging lesion that they are concerned about, which may be tender or itchy, or a nonhealing wound originally caused by some trauma. In situ tumors are typically thin, flesh-colored to erythematous, scaly or hemorrhagic plaques, while invasive SCC may present as an exophytic tumor or ulcer.[Figure caption and citation for the preceding image starts]: Squamous cell carcinoma on the ear with surrounding actinic damageFrom the collection of Dr Jessica M. Sheehan and Dr Keyoumars Soltani [Citation ends]. |
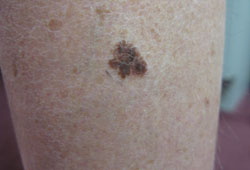
Melanoma | go to our full topic on Melanoma A malignant tumor arising from pigment-producing melanocytes found in the skin, eye, and central nervous system. Several variants exist. Clinical features of lesion asymmetry, border irregularity, color variability, diameter >6 mm, and evolution over time should raise suspicion for melanoma and prompt further assessment with dermoscopy.[13][Figure caption and citation for the preceding image starts]: Superficial spreading malignant melanomaFrom the collection of Dr Hobart W. Walling [Citation ends]. |
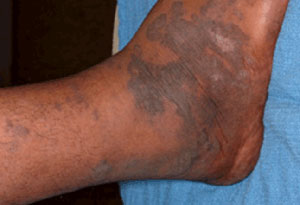
Kaposi sarcoma | go to our full topic on Kaposi sarcoma A low-grade lymphovascular neoplasm associated with human herpesvirus-8 (HHV-8, also known as Kaposi sarcoma-associated herpesvirus [KSHV]) infection.[15] Lesions frequently involve mucocutaneous sites, but may become more extensive to involve the lymph nodes and visceral organs. Skin lesions evolve from an early patch, to a plaque, and later to ulcerating tumor nodules.[Figure caption and citation for the preceding image starts]: Kaposi sarcoma cutaneous purple-brown plaque on the footFrom the collection of Dr Bruce J. Dezube [Citation ends]. |
Cutaneous T-cell lymphoma | go to our full topic on Cutaneous T-cell lymphoma Heterogeneous group of uncommon disorders characterized by clonal accumulation of T lymphocytes primarily or exclusively in the skin. The incidence of cutaneous T-cell lymphomas has been reported as <10 per 100,000 population globally.[17] While the etiology remains unclear, theories include causative genomic alterations and infectious agents. Mycosis fungoides and its leukemic variant, Sézary syndrome, are the most common subtypes.[18] Establishing a diagnosis is often difficult, as the disease can manifest in a number of different ways, including flat patches, raised plaques, large tumors, and/or marked erythroderma (intense and widespread reddening of the skin).[Figure caption and citation for the preceding image starts]: Cutaneous T-cell lymphoma: extensive patch diseaseFrom the collection of the Christie NHS Foundation Trust, Manchester, UK; used with permission [Citation ends]. |
Actinic keratosis | go to our full topic on Actinic keratosis Chronic keratotic lesions on adult skin that has been chronically exposed to UV rays. Lesions are skin-colored, yellowish, or erythematous, ill-defined, irregularly shaped, small, scaly macules or plaques localized in sun-exposed areas of the body (e.g., forehead, lower lip, dorsum of the hands and forearms, bald areas of the scalp, and ears).[Figure caption and citation for the preceding image starts]: Regular actinic keratosisFrom the collection of the Department of Dermatology and Cutaneous Surgery, University of Miami Miller School of Medicine [Citation ends]. |
Sunburn | go to our full topic on Sunburn Sunburn is an acute inflammatory reaction of the skin induced by overexposure to UV radiation. Skin findings include erythema and edema, with or without vesiculation, followed by desquamation. Key risk factors include Fitzpatrick skin type I-III, photo-sensitizing drug, intentional tanning, and lack of or improper use of sunscreen. Symptoms include pain and/or pruritus. Characteristic history and physical exam findings are usually sufficient to make the diagnosis of sunburn. Primary prevention via sun avoidance, physical protection, and the appropriate use of sunscreen is key to preventing the condition, as cellular damage caused by UV radiation is irreversible and may with time increase the risk of skin cancer. |
Contributors
Authors
Editorial Team
BMJ Publishing Group
Disclosures
This overview has been compiled using the information in existing sub-topics.
References
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.

Patient information
Skin cancer (melanoma)
Skin cancer (squamous cell)
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer