A definitive diagnosis can only be considered if the appropriate clinical case definition has been met, and/or the diagnosis has been confirmed by laboratory testing.
A high index of suspicion is recommended when evaluating people with a characteristic rash, particularly if the patient meets the epidemiologic criteria. As the clinical presentation may be atypical, include mpox in the differential diagnosis when a patient presents with a sexually transmitted infection (STI)-associated or STI-like rash, even if the rash is localized and not (yet) diffuse.
Mpox is a notifiable condition and one case is considered an outbreak. Immediately report suspected cases to national or local public health authorities, regardless of whether you are also exploring other potential diagnoses.
Screening and triage
Perform screening and triage at the first point of contact with the health system for all people who present with a rash and fever or lymphadenopathy in order to identify people that have suspected or confirmed infection.[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
A simplified questionnaire and screening protocol based on the World Health Organization (WHO) case definition (and adapted to local epidemiology) can be implemented at the point of entry to health care.
Conduct screening activities while maintaining a distance of at least 3 feet (1 meter) from the patient and using a "no touch" approach. Screening may be performed using telemedicine in certain situations, according to local pathways.
Enter patients with symptoms that meet the case definition for suspected infection into the mpox clinical care pathway immediately. Provide the patient with a well-fitting medical mask and isolate them in a well-ventilated single room.
Triage patients with suspected infection using a standardized triage tool.
Infection prevention and control
Immediately contact your regional infectious disease unit if there is a clinical suspicion of infection.
This will trigger procedures to be activated for the safe transfer of the patient to a negative-pressure isolation facility and the notification of the public health team.
It is important to keep records of everyone who has been in close contact with the symptomatic patient (e.g., household contacts, paramedical and medical staff) and whether there are any potential animal carriers present.
All suspected cases should be managed by experts, including public health officials, to prevent a potential emergency situation.
Follow your local infection prevention and control protocols.[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
Standard, contact, and droplet precautions are recommended.
Airborne precautions are recommended when caring for suspected cases of mpox if chickenpox or measles are suspected and until they are excluded. Respirators are recommended when caring for patients with suspected or confirmed mpox when the ventilation is poor or unknown, or based on risk assessment. Airborne precautions are also recommended if aerosol-generating procedures are performed.
Treat all contaminated materials (e.g., linens, hospital gowns) and body fluids/solid waste of patients as potentially infectious.
Ideally all personnel likely to be in contact with the patient, bodily fluids, or fomites should have been vaccinated.
Postexposure vaccination may be recommended for unvaccinated contacts (see Prevention).
Healthcare workers who are pregnant or immunocompromised should not assess or provide care for patients with suspected or confirmed infection, where possible.[191]UK Health Security Agency. Biological principles for control of mpox in the UK: 4 nations consensus statement. Mar 2025 [internet publication].
https://www.gov.uk/guidance/biological-principles-for-control-of-mpox-in-the-uk-4-nations-consensus-statement
Consult your local guidelines for detailed guidance on infection prevention and control measures.
History
Take a thorough patient history to assess for possible exposures or epidemiologic risk factors, including a detailed sexual history.[51]Centers for Disease Control and Prevention. Clinical overview of monkeypox. Apr 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-overview/index.html
Consider the diagnosis in patients who present with an unexplained acute rash, particularly if the patient meets one of the epidemiologic criteria in the 21 days before symptom onset.
Epidemiologic criteria include:[77]World Health Organization. Surveillance, case investigation and contact tracing for mpox: interim guidance, 27 November 2024. Dec 2024 [internet publication].
https://www.who.int/publications/i/item/B09169
[192]UK Health Security Agency. Mpox: guidance on when to suspect a case of mpox. Jun 2025 [internet publication].
https://www.gov.uk/guidance/monkeypox-case-definitions
[193]Centers for Disease Control and Prevention. Monkeypox case definitions. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/case-definitions/index.html
Recent travel to an endemic country (or country with a current outbreak)
Contact with a suspected, probable, possible, or confirmed case (or contaminated materials)
Intimate physical contact (including sexual contact) with people in a social network currently experiencing mpox activity (e.g., men who have sex with men [MSM]), or multiple and/or casual sexual partners
Contact with African-endemic species of wild animals or exotic pets (dead or alive) or products derived from these animals
Epidemiologic criteria and case definitions vary between regions. Consult your local public health authority for more information. For case definitions, see Criteria.
However, it is important to remain vigilant for mpox in anyone who presents with a mpox-compatible rash, regardless of their epidemiologic risk. A surveillance study in the US among 196 patients evaluated at 13 emergency departments for an mpox-compatible rash, irrespective of epidemiologic risk, identified three cases (1.5%) of mpox. All cases were among unvaccinated MSM who had engaged with one or more partners they met through dating applications.[194]Berdahl CT, Krishnadasan A, Pathmarajah K, et al. Mpox surveillance based on rash characteristics - 13 emergency departments, United States, June-December 2023. MMWR Morb Mortal Wkly Rep. 2024 Jun 6;73(22):507-13.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC11166258
http://www.ncbi.nlm.nih.gov/pubmed/38843078?tool=bestpractice.com
It is important to note that not all at-risk MSM will identify as being at risk, or will disclose this information.[195]Mulka L, Cassell J. The changing face of monkeypox. BMJ. 2022 Aug 10;378:o1990.
https://www.bmj.com/content/378/bmj.o1990
http://www.ncbi.nlm.nih.gov/pubmed/35948354?tool=bestpractice.com
Determine the HIV status of all sexually active adults and adolescents, as patients with HIV-associated immunocompromise are at a higher risk for severe manifestations.[196]Centers for Disease Control and Prevention. Health alert network (HAN) health advisory: severe manifestations of monkeypox among people who are immunocompromised due to HIV or other conditions. Sep 2022 [internet publication].
https://archive.cdc.gov/#/details?url=https://www.cdc.gov/han/2022/han00475.html
Clinical presentation
During the incubation period (range 1-21 days), the patient usually does not have any symptoms and may report feeling fine. A person is not contagious during the incubation period. Patients typically develop a prodrome before the appearance of the rash/lesion(s), which may last 1-5 days. However, constitutional symptoms may occur after the appearance of the rash, and some patients may have no symptoms at all.[197]Centers for Disease Control and Prevention. Clinical features of monkeypox. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-signs/index.html
[198]Philpott D, Hughes CM, Alroy KA, et al. Epidemiologic and clinical characteristics of monkeypox cases: United States, May 17 – July 22, 2022. MMWR Morb Mortal Wkly Rep. 2022 Aug 12;71(32):1018-22.
https://www.cdc.gov/mmwr/volumes/71/wr/mm7132e3.htm
http://www.ncbi.nlm.nih.gov/pubmed/35951487?tool=bestpractice.com
[199]Patel A, Bilinska J, Tam JCH, et al. Clinical features and novel presentations of human monkeypox in a central London centre during the 2022 outbreak: descriptive case series. BMJ. 2022 Jul 28;378:e072410.
https://www.bmj.com/content/378/bmj-2022-072410
http://www.ncbi.nlm.nih.gov/pubmed/35902115?tool=bestpractice.com
[200]World Health Organization. Update 79: Monkeypox outbreak update: situation - transmission - countermeasures. August 2022 [internet publication].
https://www.who.int/publications/m/item/update-79-monkeypox-outbreak-update
The clinical presentation is typically the same for clade I mpox and clade II mpox.
Common symptoms include:[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
[99]Fenner F, Henderson DA, Arita I, et al. Chapter 29: Human monkeypox and other poxvirus infections of man. In: Smallpox and its eradication. Geneva: World Health Organization; 1988.
http://apps.who.int/iris/handle/10665/39485
[197]Centers for Disease Control and Prevention. Clinical features of monkeypox. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-signs/index.html
Rash/lesion(s)
Anorectal symptoms
Fever
Chills
Lymphadenopathy
Fatigue/asthenia/malaise
Myalgia
Headache
Sore throat
Backache
Cough
Nausea/vomiting
Less common symptoms include:[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
[99]Fenner F, Henderson DA, Arita I, et al. Chapter 29: Human monkeypox and other poxvirus infections of man. In: Smallpox and its eradication. Geneva: World Health Organization; 1988.
http://apps.who.int/iris/handle/10665/39485
Diarrhea
Delirium/confusion
Seizures
While skin lesions remain the typical symptom, their anatomic distribution has been different in more recent outbreaks. Genital involvement has been more common in the 2022 global clade II mpox outbreak compared with previous outbreaks. Anorectal symptoms have been unique to the outbreak, and were not described previously.[31]Li P, Li J, Ayada I, et al. Clinical features, antiviral treatment and patient outcomes: a systematic review and comparative analysis of the previous and the 2022 mpox outbreaks. J Infect Dis. 2023 Aug 16;228(4):391-401.
https://pmc.ncbi.nlm.nih.gov/articles/PMC10428207
http://www.ncbi.nlm.nih.gov/pubmed/36735342?tool=bestpractice.com
[56]Hatami H, Jamshidi P, Arbabi M, et al. Demographic, epidemiologic, and clinical characteristics of human Monkeypox disease pre- and post-2022 Outbreaks: a systematic review and meta-analysis. Biomedicines. 2023 Mar 20;11(3):957.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10045775
http://www.ncbi.nlm.nih.gov/pubmed/36979936?tool=bestpractice.com
Skin rash/lesion(s) (95%), fever (58%), and lymphadenopathy (53%) have been the most common symptoms reported, while anorectal pain/proctitis has been reported in 18.5% of patients.[16]Liu Q, Fu L, Wang B, et al. Clinical characteristics of human mpox (monkeypox) in 2022: a systematic review and meta-analysis. Pathogens. 2023 Jan 15;12(1):146.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9861547
http://www.ncbi.nlm.nih.gov/pubmed/36678494?tool=bestpractice.com
Severe and intense anorectal pain (including severe pain on defecation), tenesmus, rectal bleeding, or purulent or bloody stools associated with perianal/rectal lesions and proctitis has been an atypical presentation. Patients presenting with proctitis may have no signs of a rash.[197]Centers for Disease Control and Prevention. Clinical features of monkeypox. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-signs/index.html
[198]Philpott D, Hughes CM, Alroy KA, et al. Epidemiologic and clinical characteristics of monkeypox cases: United States, May 17 – July 22, 2022. MMWR Morb Mortal Wkly Rep. 2022 Aug 12;71(32):1018-22.
https://www.cdc.gov/mmwr/volumes/71/wr/mm7132e3.htm
http://www.ncbi.nlm.nih.gov/pubmed/35951487?tool=bestpractice.com
[199]Patel A, Bilinska J, Tam JCH, et al. Clinical features and novel presentations of human monkeypox in a central London centre during the 2022 outbreak: descriptive case series. BMJ. 2022 Jul 28;378:e072410.
https://www.bmj.com/content/378/bmj-2022-072410
http://www.ncbi.nlm.nih.gov/pubmed/35902115?tool=bestpractice.com
[201]Pfäfflin F, Wendisch D, Scherer R, et al. Monkeypox in-patients with severe anal pain. Infection. 2023 Apr;51(2):483-7.
https://pmc.ncbi.nlm.nih.gov/articles/PMC10042938
http://www.ncbi.nlm.nih.gov/pubmed/35960457?tool=bestpractice.com
[202]Yakubovsky M, Shasha D, Reich S, et al. Monkeypox presenting as proctitis in men who have sex with men. Clin Infect Dis. 2023 Feb 8;76(3):528-30.
https://academic.oup.com/cid/article/76/3/528/6692817
http://www.ncbi.nlm.nih.gov/pubmed/36066470?tool=bestpractice.com
Other anal symptoms may include pruritus, dyschezia, burning, swelling, and mucus discharge.[203]Rekik S, Pluart DL, Ferré V, et al. Anogenital symptoms and lesions in a series of 20 patients infected with monkeypox virus. Colorectal Dis. 2023 May;25(5):1002-5.
https://onlinelibrary.wiley.com/doi/10.1111/codi.16513
http://www.ncbi.nlm.nih.gov/pubmed/36756717?tool=bestpractice.com
Men who engaged in anal-receptive sex presented with proctitis more frequently than men who did not engage in anal-receptive sex.[204]Tarín-Vicente EJ, Alemany A, Agud-Dios M, et al. Clinical presentation and virological assessment of confirmed human monkeypox virus cases in Spain: a prospective observational cohort study. Lancet. 2022 Aug 27;400(10353):661-9.
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(22)01436-2/fulltext
http://www.ncbi.nlm.nih.gov/pubmed/35952705?tool=bestpractice.com
Otolaryngologic presentations (e.g., headache, sore throat, cough, cervical lymphadenopathy) were more prevalent in previous outbreaks.[205]Shah J, Saak TM, Desai AN, et al. Otolaryngologic manifestations among MPOX patients: a systematic review and meta-analysis. Am J Otolaryngol. 2023 Nov-Dec;44(6):103991.
http://www.ncbi.nlm.nih.gov/pubmed/37487464?tool=bestpractice.com
The clinical presentation of clade Ib mpox appears to be similar to the signs and symptoms reported in the 2022 global clade II mpox outbreak, and differs from other clade I outbreaks elsewhere in Africa, based on limited observational data.[28]Brosius I, Vakaniaki EH, Mukari G, et al. Epidemiological and clinical features of mpox during the clade Ib outbreak in South Kivu, Democratic Republic of the Congo: a prospective cohort study. Lancet. 2025 Feb 15;405(10478):547-59.
http://www.ncbi.nlm.nih.gov/pubmed/39892407?tool=bestpractice.com
Prodromal symptoms were reported in 88% of patients.
Other reported symptoms included:
Lesions were reported in 89% of adults, with mean lesion density highest in the genital area, consistent with sexual transmission; only 42% of children had genital lesions and, if present, they were part of a more uniform rash.
Fever and rash were the two most common symptoms in the current clade Ia and clade Ib mpox outbreaks, with genital or anorectal lesions being the most common location.[206]Wawina-Bokalanga T, Merritt S, Kinganda-Lusamaki E, et al. Epidemiology and phylogenomic characterisation of two distinct mpox outbreaks in Kinshasa, DR Congo, involving a new subclade Ia lineage: a retrospective, observational study. Lancet. 2025 Jul 5;406(10498):63-75.
http://www.ncbi.nlm.nih.gov/pubmed/40617661?tool=bestpractice.com
Special patient populations
Children and adolescents: clinical presentation is similar to adults.[33]Centers for Disease Control and Prevention. Clinical considerations for monkeypox in children and adolescents in the U.S. Aug 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-care/pediatric.html
Severe complications have been reported in infants and young children.[133]Huang YA, Howard-Jones AR, Durrani S, et al. Monkeypox: a clinical update for paediatricians. J Paediatr Child Health. 2022 Sep;58(9):1532-8.
https://onlinelibrary.wiley.com/doi/10.1111/jpc.16171
http://www.ncbi.nlm.nih.gov/pubmed/35979896?tool=bestpractice.com
Pregnant women: clinical presentation is similar to nonpregnant people.[135]Centers for Disease Control and Prevention. Monkeypox clinical care and treatment during pregnancy. Aug 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-care/pregnancy.html
Immunocompromised people (including people with advanced or uncontrolled HIV infection): may present with atypical manifestations or a more severe illness (e.g., sepsis, disseminated rash, hemorrhagic disease, numerous confluent lesions, necrotic lesions, severe lymphadenopathy that may be obstructing, ocular or periorbital infections, pulmonary involvement, encephalitis, myocarditis, or other complications requiring hospitalization).[34]Centers for Disease Control and Prevention. Clinical considerations for monkeypox in immunocompromised people. Aug 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-care/immunocompromised-people.html
[35]O'Shea J, Filardo TD, Morris SB, et al. Interim guidance for prevention and treatment of monkeypox in persons with HIV infection: United States, August 2022. MMWR Morb Mortal Wkly Rep. 2022 Aug 12;71(32):1023-8.
https://www.cdc.gov/mmwr/volumes/71/wr/mm7132e4.htm
http://www.ncbi.nlm.nih.gov/pubmed/35951495?tool=bestpractice.com
[207]Boesecke C, Monin MB, van Bremen K, et al. Severe monkeypox-virus infection in undiagnosed advanced HIV infection. Infection. 2022 Dec;50(6):1633-4.
https://link.springer.com/article/10.1007/s15010-022-01901-z
http://www.ncbi.nlm.nih.gov/pubmed/35969365?tool=bestpractice.com
Patients with HIV may be more likely to have diarrhea, perianal rash/lesions, rectal pain, anorectal abscess, phimosis, pneumonia, and a higher rash burden.[208]Chastain DB, Motoa G, Ortiz-Martínez Y, et al. Characteristics and clinical manifestations of monkeypox among people with and without HIV in the United States: a retrospective cohort. AIDS. 2023 Mar 15;37(4):611-6.
http://www.ncbi.nlm.nih.gov/pubmed/36729995?tool=bestpractice.com
[209]Angelo KM, Smith T, Camprubí-Ferrer D, et al. Epidemiological and clinical characteristics of patients with monkeypox in the GeoSentinel Network: a cross-sectional study. Lancet Infect Dis. 2023 Feb;23(2):196-206.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9546520
http://www.ncbi.nlm.nih.gov/pubmed/36216018?tool=bestpractice.com
Case definitions vary between regions. Consult your local public health authority for more information. For case definitions, see Criteria.
Physical exam
A rash or skin lesion(s) are usually the first sign of infection. Physical exam may reveal a rash or lesion(s), and possibly lymphadenopathy. Perform a thorough skin and mucosal (e.g., anal, vaginal, oral, nasal, ophthalmic) exam.[51]Centers for Disease Control and Prevention. Clinical overview of monkeypox. Apr 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-overview/index.html
Exam may reveal lesions that the patient may not be aware of, or may reveal no lesions at all.
Traditionally, patients develop a characteristic rash approximately 1-3 days after the onset of an acute febrile illness. The rash generally starts on the face and body and spreads centrifugally to the palms and soles (it may be preceded by a rash affecting the oropharynx and tongue in the 24 hours prior that often passes unnoticed). Lesions simultaneously progress through four stages - macular, papular, vesicular, and pustular - with each stage lasting 1-2 days, before scabbing over and resolving. Lesions are typically 5-10 mm in diameter, may be discrete or confluent, and may be few in number or several thousand. Vesicles are well-circumscribed and located deep in the dermis. The rash usually resolves over a period of 2-4 weeks.[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
[11]World Health Organization. Mpox: fact sheet. Aug 2024 [internet publication].
https://www.who.int/en/news-room/fact-sheets/detail/monkeypox
[99]Fenner F, Henderson DA, Arita I, et al. Chapter 29: Human monkeypox and other poxvirus infections of man. In: Smallpox and its eradication. Geneva: World Health Organization; 1988.
http://apps.who.int/iris/handle/10665/39485
[181]McCollum AM, Damon IK. Human monkeypox. Clin Infect Dis. 2014 Jan;58(2):260-7.
https://academic.oup.com/cid/article/58/2/260/335791
http://www.ncbi.nlm.nih.gov/pubmed/24158414?tool=bestpractice.com
[197]Centers for Disease Control and Prevention. Clinical features of monkeypox. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-signs/index.html
In more recent outbreaks, the presentation has been atypical, with the rash presenting primarily in the anogenital region.[55]Sukhdeo S, Mishra S, Walmsley S. Human monkeypox: a comparison of the characteristics of the new epidemic to the endemic disease. BMC Infect Dis. 2022 Dec 12;22(1):928.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9742013
http://www.ncbi.nlm.nih.gov/pubmed/36503476?tool=bestpractice.com
Lesions tend to be localized to the genital, perineal/perianal, or perioral areas and often do not spread further, suggesting that transmission occurs as a result of contact during sexual intercourse, with lesions possibly starting at the site of inoculation.[71]World Health Organization. Multi-country monkeypox outbreak: situation update. Jun 2022 [internet publication].
https://www.who.int/emergencies/disease-outbreak-news/item/2022-DON396
[197]Centers for Disease Control and Prevention. Clinical features of monkeypox. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-signs/index.html
[210]Girometti N, Byrne R, Bracchi M, et al. Demographic and clinical characteristics of confirmed human monkeypox virus cases in individuals attending a sexual health centre in London, UK: an observational analysis. Lancet Infect Dis. 2022 Sep;22(9):1321-8.
https://www.thelancet.com/journals/laninf/article/PIIS1473-3099(22)00411-X/fulltext
http://www.ncbi.nlm.nih.gov/pubmed/35785793?tool=bestpractice.com
[211]European Centre for Disease Prevention and Control. Monkeypox cases reported in UK and Portugal. May 2022 [internet publication].
https://www.ecdc.europa.eu/en/news-events/monkeypox-cases-reported-uk-and-portugal
[212]Patrocinio-Jesus R, Peruzzu F. Monkeypox genital lesions. N Engl J Med. 2022 Jul 7;387(1):66.
https://www.nejm.org/doi/10.1056/NEJMicm2206893
http://www.ncbi.nlm.nih.gov/pubmed/35704421?tool=bestpractice.com
[213]Orviz E, Negredo A, Ayerdi O, et al. Monkeypox outbreak in Madrid (Spain): clinical and virological aspects. J Infect. 2022 Oct;85(4):412-7.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9534097
http://www.ncbi.nlm.nih.gov/pubmed/35830908?tool=bestpractice.com
[214]Català A, Clavo Escribano P, Riera J, et al. Monkeypox outbreak in Spain: clinical and epidemiological findings in a prospective cross-sectional study of 185 cases. Br J Dermatol. 2022 Nov;187(5):765-72.
https://onlinelibrary.wiley.com/doi/10.1111/bjd.21790
http://www.ncbi.nlm.nih.gov/pubmed/35917191?tool=bestpractice.com
A larger number of lesions in the mouth and throat has been linked to oral sex, and a larger number of lesions in the perianal area has been linked to anal-receptive sex.[204]Tarín-Vicente EJ, Alemany A, Agud-Dios M, et al. Clinical presentation and virological assessment of confirmed human monkeypox virus cases in Spain: a prospective observational cohort study. Lancet. 2022 Aug 27;400(10353):661-9.
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(22)01436-2/fulltext
http://www.ncbi.nlm.nih.gov/pubmed/35952705?tool=bestpractice.com
Other atypical features include:[71]World Health Organization. Multi-country monkeypox outbreak: situation update. Jun 2022 [internet publication].
https://www.who.int/emergencies/disease-outbreak-news/item/2022-DON396
[197]Centers for Disease Control and Prevention. Clinical features of monkeypox. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-signs/index.html
[199]Patel A, Bilinska J, Tam JCH, et al. Clinical features and novel presentations of human monkeypox in a central London centre during the 2022 outbreak: descriptive case series. BMJ. 2022 Jul 28;378:e072410.
https://www.bmj.com/content/378/bmj-2022-072410
http://www.ncbi.nlm.nih.gov/pubmed/35902115?tool=bestpractice.com
[215]Quattri E, Avallone G, Maronese CA, et al. Unilesional monkeypox: a report of two cases from Italy. Travel Med Infect Dis. 2022 Aug 10;49:102424.
https://www.sciencedirect.com/science/article/pii/S1477893922001703
http://www.ncbi.nlm.nih.gov/pubmed/35961491?tool=bestpractice.com
Presentation of only a few lesions (or even just a single lesion) and may not be disseminated
Absence of skin lesions and anal pain and bleeding
Lesions appearing at different stages of development (asynchronous)
Rash does not always appear on palms and soles
Appearance of lesions before the prodrome
[Figure caption and citation for the preceding image starts]: Images of individual lesions (2022 global outbreak)UKHSA [Citation ends].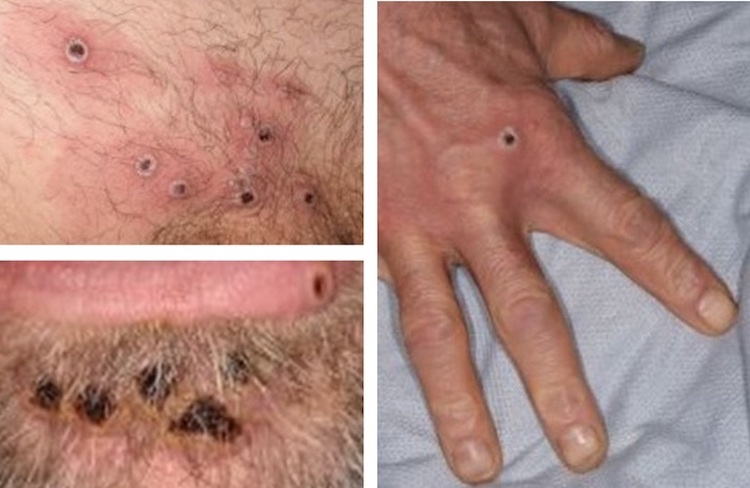
Most patients (64%) had <10 lesions, with approximately 10% of patients having only a single genital lesion in the 2022 global clade II mpox outbreak.[110]Thornhill JP, Barkati S, Walmsley S, et al. Monkeypox virus infection in humans across 16 countries: April–June 2022. N Engl J Med. 2022 Aug 25;387(8):679-91.
https://www.nejm.org/doi/full/10.1056/NEJMoa2207323
http://www.ncbi.nlm.nih.gov/pubmed/35866746?tool=bestpractice.com
Some patients may have no cutaneous/mucosal lesions and only systemic signs/symptoms at the time of diagnosis.[216]Ciccarese G, Brucci G, Di Biagio A, et al. Two cases of monkeypox virus infection without detectable cutaneous/mucosal lesions. Travel Med Infect Dis. 2023 Jul-Aug;54:102605.
https://www.sciencedirect.com/science/article/pii/S1477893923000650?via%3Dihub
Atypical single lesions can mimic abscesses and other deep-tissue phenomena.[195]Mulka L, Cassell J. The changing face of monkeypox. BMJ. 2022 Aug 10;378:o1990.
https://www.bmj.com/content/378/bmj.o1990
http://www.ncbi.nlm.nih.gov/pubmed/35948354?tool=bestpractice.com
Approximately one third of patients presented with lesions at different stages of evolution at a single time point in one study.[199]Patel A, Bilinska J, Tam JCH, et al. Clinical features and novel presentations of human monkeypox in a central London centre during the 2022 outbreak: descriptive case series. BMJ. 2022 Jul 28;378:e072410.
https://www.bmj.com/content/378/bmj-2022-072410
http://www.ncbi.nlm.nih.gov/pubmed/35902115?tool=bestpractice.com
The most common type of lesions in the 2022 global clade II mpox outbreak have been anogenital lesions (66%). Oropharyngeal/oral lesions have been present in 21% of patients.[16]Liu Q, Fu L, Wang B, et al. Clinical characteristics of human mpox (monkeypox) in 2022: a systematic review and meta-analysis. Pathogens. 2023 Jan 15;12(1):146.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9861547
http://www.ncbi.nlm.nih.gov/pubmed/36678494?tool=bestpractice.com
Oral lesions may be observed in different parts of the oral mucosa including the lips, tongue, and, most commonly, the tonsils. Lesions have also been reported in the esophagus.[217]Ardila CM, Arrubla-Escobar DE, Vivares-Builes AM. Oral lesions in patients with human monkeypox: a systematic scoping review. J Oral Pathol Med. 2023 Jul;52(6):459-67.
http://www.ncbi.nlm.nih.gov/pubmed/36263594?tool=bestpractice.com
[218]Mishra S, Khan R, Krizova A, et al. Esophageal monkeypox lesion. Clin Gastroenterol Hepatol. 2023 Jan;21(1):A17-8.
https://pmc.ncbi.nlm.nih.gov/articles/PMC9534271
http://www.ncbi.nlm.nih.gov/pubmed/36174941?tool=bestpractice.com
Rarely, auricular lesions may occur.[219]Williams G, Watters C, Watson N. Auricular manifestation of mpox (monkeypox). BMJ Case Rep. 2023 Jan 19;16(1):e252931.
https://casereports.bmj.com/content/16/1/e252931.long
http://www.ncbi.nlm.nih.gov/pubmed/36657823?tool=bestpractice.com
Although most patients in the 2022 global clade II mpox outbreak have been men, localized genital lesions (vulvar and intravaginal) and cervical lesions have been reported in women.[220]Portela-Dias J, Sereno S, Falcão-Reis I, et al. Monkeypox infection with localized genital lesions in women. Am J Obstet Gynecol. 2022 Dec;227(6):906.
https://pmc.ncbi.nlm.nih.gov/articles/PMC9534063
http://www.ncbi.nlm.nih.gov/pubmed/36030847?tool=bestpractice.com
[221]Vallée A, Chatelain A, Carbonnel M, et al. Monkeypox virus infection in 18-year-old woman after sexual intercourse, France, September 2022. Emerg Infect Dis. 2022 Nov 10;29(1).
https://wwwnc.cdc.gov/eid/article/29/1/22-1643_article
http://www.ncbi.nlm.nih.gov/pubmed/36355630?tool=bestpractice.com
[222]Zayat N, Huang S, Wafai J, et al. Monkeypox virus infection in 22-year-old woman after sexual intercourse, New York, USA. Emerg Infect Dis. 2022 Nov 10;29(1).
https://wwwnc.cdc.gov/eid/article/29/1/22-1662_article
http://www.ncbi.nlm.nih.gov/pubmed/36355634?tool=bestpractice.com
[223]Ramírez M, Delso V, Sánchez MJ, et al. Mpox (monkeypox) presenting as cervical and vulvar disease. Obstet Gynecol. 2023 Mar 1;141(3):613-7.
http://www.ncbi.nlm.nih.gov/pubmed/36626748?tool=bestpractice.com
Vulvovaginal lesions have been predominant in cisgender women and anorectal features have been predominant in transgender women, anatomically reflecting sexual practices.[36]Thornhill JP, Palich R, Ghosn J, et al. Human monkeypox virus infection in women and non-binary individuals during the 2022 outbreaks: a global case series. Lancet. 2022 Dec 3;400(10367):1953-65.
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(22)02187-0/fulltext
http://www.ncbi.nlm.nih.gov/pubmed/36403584?tool=bestpractice.com
Lesions may be classified as papules, vesicles, blisters, pustules, erosions, ulcers, or crusts.[224]Prasad S, Casas CG, Strahan AG, et al. A dermatologic assessment of 101 mpox (monkeypox) cases from 13 countries during the 2022 outbreak: skin lesion morphology, clinical course, and scarring. J Am Acad Dermatol. 2023 May;88(5):1066-73.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9833815
http://www.ncbi.nlm.nih.gov/pubmed/36641010?tool=bestpractice.com
They may be painful initially, and become itchy during the healing phase.
Lesions on the external genitalia may cause severe swelling and pain. Oral lesions may cause difficulties with eating and drinking, which may lead to dehydration and malnutrition. Patients may present with the following complications depending on the location of the rash/lesion(s) (see Complications):[199]Patel A, Bilinska J, Tam JCH, et al. Clinical features and novel presentations of human monkeypox in a central London centre during the 2022 outbreak: descriptive case series. BMJ. 2022 Jul 28;378:e072410.
https://www.bmj.com/content/378/bmj-2022-072410
http://www.ncbi.nlm.nih.gov/pubmed/35902115?tool=bestpractice.com
[200]World Health Organization. Update 79: Monkeypox outbreak update: situation - transmission - countermeasures. August 2022 [internet publication].
https://www.who.int/publications/m/item/update-79-monkeypox-outbreak-update
[225]Gomez-Garberi M, Sarrio-Sanz P, Martinez-Cayuelas L, et al. Genitourinary lesions due to monkeypox. Eur Urol. 2022 Dec;82(6):625-30.
https://www.sciencedirect.com/science/article/pii/S0302283822026252
http://www.ncbi.nlm.nih.gov/pubmed/36096858?tool=bestpractice.com
Severe penile or scrotal edema, paraphimosis/phimosis, balanitis
Tonsillitis, peritonsillar cellulitis, tonsillar/peritonsillar abscess, epiglottitis
Perianal/groin abscess, rectal perforation
Urinary retention, urethritis
Erythematous maculopapular, generalized purpuric, and morbilliform rashes have been reported in some patients.[199]Patel A, Bilinska J, Tam JCH, et al. Clinical features and novel presentations of human monkeypox in a central London centre during the 2022 outbreak: descriptive case series. BMJ. 2022 Jul 28;378:e072410.
https://www.bmj.com/content/378/bmj-2022-072410
http://www.ncbi.nlm.nih.gov/pubmed/35902115?tool=bestpractice.com
[224]Prasad S, Casas CG, Strahan AG, et al. A dermatologic assessment of 101 mpox (monkeypox) cases from 13 countries during the 2022 outbreak: skin lesion morphology, clinical course, and scarring. J Am Acad Dermatol. 2023 May;88(5):1066-73.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9833815
http://www.ncbi.nlm.nih.gov/pubmed/36641010?tool=bestpractice.com
[226]Simon-Gozalbo A, Gamo-Guerrero M, Alonso-Garcia S, et al. Haemorrhagic monkeypox infection in an immunosuppressed patient with human immunodeficiency virus: beyond the pustules. Clin Microbiol Infect. 2023 Jan;29(1):122-4.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9534161
http://www.ncbi.nlm.nih.gov/pubmed/36206864?tool=bestpractice.com
Lymphadenopathy
Lymphadenopathy may be generalized or localized to several areas. It typically occurs with onset of fever and preceding the rash or, rarely, with the onset of the rash. May be submandibular, cervical, axillary, or inguinal, and may occur on both sides of the body or just one side.
Enlarged lymph nodes are approximately 1-4 cm in diameter, firm, tender, and sometimes painful.[181]McCollum AM, Damon IK. Human monkeypox. Clin Infect Dis. 2014 Jan;58(2):260-7.
https://academic.oup.com/cid/article/58/2/260/335791
http://www.ncbi.nlm.nih.gov/pubmed/24158414?tool=bestpractice.com
Lymphadenopathy is a common distinguishing feature, but is rare in smallpox and other diseases in the differential diagnosis.[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
[46]Huhn GD, Bauer AM, Yorita K, et al. Clinical characteristics of human monkeypox, and risk factors for severe disease. Clin Infect Dis. 2005 Dec 15;41(12):1742-51.
https://academic.oup.com/cid/article/41/12/1742/344953
http://www.ncbi.nlm.nih.gov/pubmed/16288398?tool=bestpractice.com
[99]Fenner F, Henderson DA, Arita I, et al. Chapter 29: Human monkeypox and other poxvirus infections of man. In: Smallpox and its eradication. Geneva: World Health Organization; 1988.
http://apps.who.int/iris/handle/10665/39485
[181]McCollum AM, Damon IK. Human monkeypox. Clin Infect Dis. 2014 Jan;58(2):260-7.
https://academic.oup.com/cid/article/58/2/260/335791
http://www.ncbi.nlm.nih.gov/pubmed/24158414?tool=bestpractice.com
The clinical presentation of clade Ib mpox appears to be similar to the presentation in the 2022 global clade II mpox outbreak; genital lesions and lymphadenopathy are common.[28]Brosius I, Vakaniaki EH, Mukari G, et al. Epidemiological and clinical features of mpox during the clade Ib outbreak in South Kivu, Democratic Republic of the Congo: a prospective cohort study. Lancet. 2025 Feb 15;405(10478):547-59.
http://www.ncbi.nlm.nih.gov/pubmed/39892407?tool=bestpractice.com
Disease severity and risk factors for severe disease
Most cases are mild, but the spectrum of disease ranges from mild to severe, and can be fatal.
Disease severity depends on the initial health of the patient, their immune response, previous vaccination status, presence of comorbidities, the route of exposure, and the virus strain.[197]Centers for Disease Control and Prevention. Clinical features of monkeypox. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-signs/index.html
The clade II virus is associated with milder disease compared with the clade I virus.[5]Beer EM, Rao VB. A systematic review of the epidemiology of human monkeypox outbreaks and implications for outbreak strategy. PLoS Negl Trop Dis. 2019 Oct;13(10):e0007791.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6816577
http://www.ncbi.nlm.nih.gov/pubmed/31618206?tool=bestpractice.com
The severity of clade Ia mpox is high, with a significant burden of rash compared with clade IIb mpox, and increased case fatality rates.[50]World Health Organization. Risk evaluation of clade Ib monkeypox virus: review of evidence. Jan 2025 [internet publication].
https://www.who.int/publications/m/item/risk-evaluation-of-clade-1b-monkeypox-virus-review-of-evidence
The severity of clade Ib mpox is lower than that of clade Ia mpox with lower case fatality rates, similar to that of clade IIb.[50]World Health Organization. Risk evaluation of clade Ib monkeypox virus: review of evidence. Jan 2025 [internet publication].
https://www.who.int/publications/m/item/risk-evaluation-of-clade-1b-monkeypox-virus-review-of-evidence
Asymptomatic infection has been described, but the extent to which asymptomatic infection may occur is unknown.[99]Fenner F, Henderson DA, Arita I, et al. Chapter 29: Human monkeypox and other poxvirus infections of man. In: Smallpox and its eradication. Geneva: World Health Organization; 1988.
http://apps.who.int/iris/handle/10665/39485
[100]Reda A, El-Qushayri AE, Shah J. Asymptomatic monkeypox infection: a call for greater control of infection and transmission. Lancet Microbe. 2023 Jan;4(1):e15-6.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9536807
http://www.ncbi.nlm.nih.gov/pubmed/36209756?tool=bestpractice.com
Immunity from past smallpox vaccination substantially reduces the frequency and intensity of clinical signs and symptoms.[5]Beer EM, Rao VB. A systematic review of the epidemiology of human monkeypox outbreaks and implications for outbreak strategy. PLoS Negl Trop Dis. 2019 Oct;13(10):e0007791.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6816577
http://www.ncbi.nlm.nih.gov/pubmed/31618206?tool=bestpractice.com
There is limited evidence for a milder disease course in patients with a history of childhood smallpox vaccination, but hospitalization rates were not lower in vaccinated people.[227]Hoffmann C, Wolf E, Jessen H, et al. Is there any evidence for milder courses of monkeypox virus infections with childhood smallpox vaccination? Infection. 2023 Apr;51(2):535-6.
https://pmc.ncbi.nlm.nih.gov/articles/PMC10042975
http://www.ncbi.nlm.nih.gov/pubmed/36125626?tool=bestpractice.com
Evaluate the patient to determine whether they have signs and symptoms of severe or complicated disease.[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
Clinical signs and symptoms of complications:
Nausea and vomiting
Painful cervical lymphadenopathy causing dysphagia
Poor oral intake or dehydration
Eye pain or vision abnormalities
Hepatomegaly
Sepsis
Dehydration
Respiratory distress/pneumonia
Confusion
Laboratory abnormalities:
Skin lesion severity score:
Mild (<25 lesions)
Moderate (25-99 skin lesions)
Severe (100-250 skin lesions)
Very severe (>250 skin lesions)
In the US, the Centers for Disease Control and Prevention (CDC) defines severe disease as patients with:[228]Rao AK, Schrodt CA, Minhaj FS, et al. Interim clinical treatment considerations for severe manifestations of mpox: United States, February 2023. MMWR Morb Mortal Wkly Rep. 2023 Mar 3;72(9):232-43.
https://www.cdc.gov/mmwr/volumes/72/wr/mm7209a4.htm
http://www.ncbi.nlm.nih.gov/pubmed/36862595?tool=bestpractice.com
A large number of lesions such that they are confluent
Hemorrhagic disease
Necrotic lesions
Severe lymphadenopathy that can be necrotizing or obstructing (e.g., in airways or gastrointestinal tract)
Edema that is obstructing (e.g., lower gastrointestinal tract)
Involvement of multiple organ systems and associated comorbidities (e.g., sepsis, encephalitis, myocarditis, ocular or periorbital infections, pulmonary involvement with nodular lesions)
Evaluate the patient to determine whether there are any risk factors present. Patient groups at higher risk of severe disease or complications include:[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
[229]Centers for Disease Control and Prevention. Clinical treatment of monkeypox. Aug 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-care/index.html
Children (particularly ages <8 years)
Pregnant or breastfeeding women
Immunocompromised people (e.g., advanced or poorly controlled HIV infection, malignancy, transplant recipients, autoimmune disease with immunodeficiency)
People with acute or chronic skin conditions
When assessing patients with HIV infection, consider viral suppression and CD4 count when determining the patient’s risk of severe outcomes.[35]O'Shea J, Filardo TD, Morris SB, et al. Interim guidance for prevention and treatment of monkeypox in persons with HIV infection: United States, August 2022. MMWR Morb Mortal Wkly Rep. 2022 Aug 12;71(32):1023-8.
https://www.cdc.gov/mmwr/volumes/71/wr/mm7132e4.htm
http://www.ncbi.nlm.nih.gov/pubmed/35951495?tool=bestpractice.com
Initial investigations
Definitive diagnosis requires laboratory confirmation. Testing is available at regional public health laboratories.
Testing should be conducted in patients with suspected infection as soon as possible.[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
Offer testing to any person who meets the case definition for a suspected or probable case.[230]World Health Organization. Diagnostic testing for the monkeypox virus (MPXV): interim guidance. May 2024 [internet publication].
https://www.who.int/publications/i/item/WHO-MPX-Laboratory-2024.1
The decision to test should be based on both clinical and epidemiologic factors, linked to an assessment of the likelihood of infection.
Undertake diagnostic testing for other diseases in the differential diagnosis in parallel with mpox testing.
Patients should remain in isolation while their test result is pending.
Nucleic acid amplification testing (NAAT), using real-time reverse transcription polymerase chain reaction (RT-PCR) or conventional PCR, is the preferred laboratory test given its accuracy and sensitivity. It can be used alone or in combination with sequencing for clade determination.[230]World Health Organization. Diagnostic testing for the monkeypox virus (MPXV): interim guidance. May 2024 [internet publication].
https://www.who.int/publications/i/item/WHO-MPX-Laboratory-2024.1
[231]UK Health Security Agency. Mpox: diagnostic testing. Apr 2025 [internet publication].
https://www.gov.uk/guidance/monkeypox-diagnostic-testing
[232]Altindis M, Puca E, Shapo L. Diagnosis of monkeypox virus: an overview. Travel Med Infect Dis. 2022 Sep 13;50:102459.
https://www.sciencedirect.com/science/article/pii/S1477893922002058
http://www.ncbi.nlm.nih.gov/pubmed/36109000?tool=bestpractice.com
[233]Gul I, Liu C, Yuan X, et al. Current and perspective sensing methods for monkeypox virus. Bioengineering (Basel). 2022 Oct 18;9(10):571.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9598380
http://www.ncbi.nlm.nih.gov/pubmed/36290539?tool=bestpractice.com
[234]Centers for Disease Control and Prevention. Guidelines for collecting and handling specimens for monkeypox testing. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/diagnosis-testing/collecting-specimens.html
NAAT can be generic to Orthopoxvirus or specific to monkeypox virus (preferable). Positive detection using an Orthopoxvirus PCR assay should be followed by monkeypox virus PCR and/or sequencing or detection to confirm the diagnosis. If clade-specific NAATs fail to detect mpox, subsequent sequencing may be used for clade determination and genetic characterization.[230]World Health Organization. Diagnostic testing for the monkeypox virus (MPXV): interim guidance. May 2024 [internet publication].
https://www.who.int/publications/i/item/WHO-MPX-Laboratory-2024.1
Caution is required when interpreting a single test result in patients with a low pretest probability of infection (e.g., lack of epidemiologic link, non-MSM populations, signs/symptoms inconsistent with mpox) due to the risk of a false-positive result.[235]Minhaj FS, Petras JK, Brown JA, et al. Orthopoxvirus testing challenges for persons in populations at low risk or without known epidemiologic link to monkeypox: United States, 2022. MMWR Morb Mortal Wkly Rep. 2022 Sep 9;71(36):1155-8.
https://www.cdc.gov/mmwr/volumes/71/wr/mm7136e1.htm
http://www.ncbi.nlm.nih.gov/pubmed/36074752?tool=bestpractice.com
Repeat testing (re-extraction and retesting of the specimen) is recommended in patients with high RT-PCR cycle threshold values (i.e., ≥34), as this indicates a low level of viral DNA and poorly- or noninfectious specimens.[235]Minhaj FS, Petras JK, Brown JA, et al. Orthopoxvirus testing challenges for persons in populations at low risk or without known epidemiologic link to monkeypox: United States, 2022. MMWR Morb Mortal Wkly Rep. 2022 Sep 9;71(36):1155-8.
https://www.cdc.gov/mmwr/volumes/71/wr/mm7136e1.htm
http://www.ncbi.nlm.nih.gov/pubmed/36074752?tool=bestpractice.com
[236]Paran N, Yahalom-Ronen Y, Shifman O, et al. Monkeypox DNA levels correlate with virus infectivity in clinical samples, Israel, 2022. Euro Surveill. 2022 Sep;27(35).
https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2022.27.35.2200636
http://www.ncbi.nlm.nih.gov/pubmed/36052723?tool=bestpractice.com
Sequencing is useful to determine virus clade and to understand epidemiology. Following a cluster of sexually transmitted clade I infections first identified in 2023 (due to the newly identified clade Ib variant), clade confirmation is recommended in all individuals who test positive for mpox.[231]UK Health Security Agency. Mpox: diagnostic testing. Apr 2025 [internet publication].
https://www.gov.uk/guidance/monkeypox-diagnostic-testing
[237]McQuiston JH, Luce R, Kazadi DM, et al. U.S. preparedness and response to increasing clade I mpox cases in the Democratic Republic of the Congo - United States, 2024. MMWR Morb Mortal Wkly Rep. 2024 May 16;73(19):435-40.
https://www.cdc.gov/mmwr/volumes/73/wr/mm7319a3.htm
http://www.ncbi.nlm.nih.gov/pubmed/38753567?tool=bestpractice.com
The recommended specimen type is skin lesion material, including swabs of lesion exudate, roofs from more than one lesion, or lesion crusts.[230]World Health Organization. Diagnostic testing for the monkeypox virus (MPXV): interim guidance. May 2024 [internet publication].
https://www.who.int/publications/i/item/WHO-MPX-Laboratory-2024.1
[231]UK Health Security Agency. Mpox: diagnostic testing. Apr 2025 [internet publication].
https://www.gov.uk/guidance/monkeypox-diagnostic-testing
[234]Centers for Disease Control and Prevention. Guidelines for collecting and handling specimens for monkeypox testing. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/diagnosis-testing/collecting-specimens.html
Two samples are recommended to ensure sufficient material for confirmatory testing.[231]UK Health Security Agency. Mpox: diagnostic testing. Apr 2025 [internet publication].
https://www.gov.uk/guidance/monkeypox-diagnostic-testing
Skin lesion swabs are the most effective means of detecting monkeypox virus DNA using PCR.[238]Martins-Filho PR, Tanajura DM, Alves Dos Santos C. Polymerase chain reaction positivity and cycle threshold values in biological samples from patients with monkeypox: a meta-analysis. Travel Med Infect Dis. 2022 Sep 7;50:102448.
https://www.sciencedirect.com/science/article/pii/S1477893922001946
http://www.ncbi.nlm.nih.gov/pubmed/36087645?tool=bestpractice.com
[239]Hasso M, Perusini S, Eshaghi A, et al. Monkeypox virus detection in different clinical specimen types. Emerg Infect Dis. 2022 Oct 12;28(12).
https://wwwnc.cdc.gov/eid/article/28/12/22-1160_article
http://www.ncbi.nlm.nih.gov/pubmed/36223653?tool=bestpractice.com
Specimen type may vary depending on the phase of the rash. Alternative specimen types (e.g., oropharyngeal swabs) can be collected from contacts of suspected or confirmed cases but who have no visible skin or mucosal lesions. However, they may lack sensitivity in presymptomatic cases, and testing should be repeated on lesion material if a rash or mucosal lesions develop.[230]World Health Organization. Diagnostic testing for the monkeypox virus (MPXV): interim guidance. May 2024 [internet publication].
https://www.who.int/publications/i/item/WHO-MPX-Laboratory-2024.1
Aspiration or unroofing of lesions before swabbing is not necessary (or recommended) due to the risk for sharps injury.
Collect other diagnostic material as dictated by the reference laboratory protocol, such as oropharyngeal swabs, anorectal swabs, ethylenediamine tetra-acetic acid (EDTA) blood, semen, or urine.
Oropharyngeal swabs are recommended for high-risk contacts of a confirmed or highly probable case who have developed systemic symptoms but do not have a rash or lesion for sampling. A throat swab should also be taken if there are pharyngeal lesions.[231]UK Health Security Agency. Mpox: diagnostic testing. Apr 2025 [internet publication].
https://www.gov.uk/guidance/monkeypox-diagnostic-testing
However, viral load is higher in lesion swabs than in pharyngeal specimens, and oropharyngeal swabs are known to be unreliable standalone specimen types for primary diagnosis.[204]Tarín-Vicente EJ, Alemany A, Agud-Dios M, et al. Clinical presentation and virological assessment of confirmed human monkeypox virus cases in Spain: a prospective observational cohort study. Lancet. 2022 Aug 27;400(10353):661-9.
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(22)01436-2/fulltext
http://www.ncbi.nlm.nih.gov/pubmed/35952705?tool=bestpractice.com
[240]Nörz D, Brehm TT, Tang HT, et al. Clinical characteristics and comparison of longitudinal qPCR results from different specimen types in a cohort of ambulatory and hospitalized patients infected with monkeypox virus. J Clin Virol. 2022 Aug 11;155:105254.
https://www.sciencedirect.com/science/article/pii/S138665322200186X
http://www.ncbi.nlm.nih.gov/pubmed/36057206?tool=bestpractice.com
There are limited clinical data to support the use of sample types other than swab samples taken directly from a lesion (e.g., blood, saliva). Testing samples not taken from a lesion may lead to false positive results.[241]US Food and Drug Administration. For monkeypox testing, use lesion swab samples to avoid false results: FDA safety communication. Jul 2022 [internet publication].
https://www.fda.gov/medical-devices/emergency-situations-medical-devices/monkeypox-mpox-and-medical-devices
[242]Veintimilla C, Catalán P, Alonso R, et al. The relevance of multiple clinical specimens in the diagnosis of monkeypox virus, Spain, June 2022. Euro Surveill. 2022 Aug;27(33).
https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2022.27.33.2200598
http://www.ncbi.nlm.nih.gov/pubmed/35983771?tool=bestpractice.com
[243]Allan-Blitz LT, Carragher K, Sukhija-Cohen A, et al. Laboratory validation and clinical performance of a saliva-based test for monkeypox virus. J Med Virol. 2023 Jan;95(1):e28191.
https://onlinelibrary.wiley.com/doi/10.1002/jmv.28191
http://www.ncbi.nlm.nih.gov/pubmed/36183189?tool=bestpractice.com
Recommended specimens may differ between testing laboratories and you should always consult your local guidance.
Collect, label, package, and send specimens according to local or national protocols. Notify the laboratory of the possibility of mpox prior to sending specimens. There are local protocols in place for the safe handling of these specimens in the laboratory and onward transport of virologic materials to the reference laboratory. Testing may be expedited for suspected clade I infections; therefore, alert your local laboratory if this is the case. Package samples for testing for other infections separately.
Also order routine blood tests in patients, including:
Evaluate and test all sexually active adults and adolescents for HIV infection and other STIs, particularly those presenting with anal, genital, or perianal ulcers, proctitis, or diffuse rash.[1]World Health Organization. Clinical management and infection prevention and control for mpox: living guideline, May 2025. Jun 2025 [internet publication].
https://www.who.int/publications/i/item/B09434
[51]Centers for Disease Control and Prevention. Clinical overview of monkeypox. Apr 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-overview/index.html
[196]Centers for Disease Control and Prevention. Health alert network (HAN) health advisory: severe manifestations of monkeypox among people who are immunocompromised due to HIV or other conditions. Sep 2022 [internet publication].
https://archive.cdc.gov/#/details?url=https://www.cdc.gov/han/2022/han00475.html
Other investigations
Consider a computed tomography (CT) scan of the abdomen/pelvis in patients with severe anorectal proctitis. Contrast-enhanced CT may reveal circumferential anorectal mural thickening with broad discrete nonenhancing hypoattenuated zones due to intramural ulcers. Additional findings may include perirectal fat infiltration, presacral edema, ascites, and an increased number of small inguinal lymph nodes.[244]Messina MD, Wolf EL, Kanmaniraja D, et al. Imaging features of anorectal proctitis in monkeypox infection. Clin Imaging. 2022 Dec;92:109-11.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9583688
http://www.ncbi.nlm.nih.gov/pubmed/36302321?tool=bestpractice.com
Order a blood culture while the patient is in isolation and prior to antibiotic therapy, if there is suspicion of bacterial superinfection of cutaneous lesions or bacterial infection in a very sick patient.
Serology, cell culture, and antigen detection methods are not currently recommended for diagnosis.
Serology (paired serum samples collected at least 14-21 days apart, with the first collected during the first week of illness) can aid diagnosis if tested samples yield inconclusive results with molecular testing. Recent vaccination may interfere with serologic testing.[230]World Health Organization. Diagnostic testing for the monkeypox virus (MPXV): interim guidance. May 2024 [internet publication].
https://www.who.int/publications/i/item/WHO-MPX-Laboratory-2024.1
Serology may be helpful in epidemiologic investigations, retrospective diagnosis of past infections, and diagnosis of late clinical manifestations.[245]Titanji BK, Tegomoh B, Nematollahi S, et al. Monkeypox: a contemporary review for healthcare professionals. Open Forum Infect Dis. 2022 Jul;9(7):ofac310.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9307103
http://www.ncbi.nlm.nih.gov/pubmed/35891689?tool=bestpractice.com
Orthopoxviruses are serologically cross-reactive; therefore, serologic testing is not specific to mpox.[246]El Eid R, Allaw F, Haddad SF, et al. Human monkeypox: a review of the literature. PLoS Pathog. 2022 Sep;18(9):e1010768.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9498972
http://www.ncbi.nlm.nih.gov/pubmed/36136979?tool=bestpractice.com
Cell culture is restricted to accredited biosafety level 3 reference laboratories. The major disadvantage of culture-based diagnosis is the prolonged assay time, which is not suitable for mass testing scenarios.[233]Gul I, Liu C, Yuan X, et al. Current and perspective sensing methods for monkeypox virus. Bioengineering (Basel). 2022 Oct 18;9(10):571.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9598380
http://www.ncbi.nlm.nih.gov/pubmed/36290539?tool=bestpractice.com
[245]Titanji BK, Tegomoh B, Nematollahi S, et al. Monkeypox: a contemporary review for healthcare professionals. Open Forum Infect Dis. 2022 Jul;9(7):ofac310.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9307103
http://www.ncbi.nlm.nih.gov/pubmed/35891689?tool=bestpractice.com
Always rule out coinfection with malaria in any febrile patient who has been to a malaria-endemic area, especially in the 3 weeks prior to onset of fever. An antigen detection test poses less of an infection hazard to laboratory staff than preparation of thick and thin films.
Several diagnostic methods are emerging. Biopsy of affected tissue may be considered in patients who are severely immunocompromised to help better understand the cause of specific symptoms, but it may only be recommended in certain locations where testing is available.[247]Centers for Disease Control and Prevention. Additional testing of biopsy tissues in severe monkeypox infections. Sep 2024 [internet publication].
https://www.cdc.gov/monkeypox/hcp/diagnosis-testing/biopsy.html
CRISPR-based assays are in development as a faster alternative to PCR, but are not yet available.[248]Sui Y, Xu Q, Liu M, et al. CRISPR-Cas12a-based detection of monkeypox virus. J Infect. 2022 Dec;85(6):702-69.
https://www.journalofinfection.com/article/S0163-4453(22)00527-8/fulltext
http://www.ncbi.nlm.nih.gov/pubmed/36084670?tool=bestpractice.com
Loop-mediated isothermal amplification (LAMP) assays for the specific detection of monkeypox virus are also in development.[233]Gul I, Liu C, Yuan X, et al. Current and perspective sensing methods for monkeypox virus. Bioengineering (Basel). 2022 Oct 18;9(10):571.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9598380
http://www.ncbi.nlm.nih.gov/pubmed/36290539?tool=bestpractice.com
[249]Feng J, Xue G, Cui X, et al. Development of a loop-mediated isothermal amplification method for rapid and visual detection of monkeypox virus. Microbiol Spectr. 2022 Sep 26:e0271422.
https://journals.asm.org/doi/10.1128/spectrum.02714-22
http://www.ncbi.nlm.nih.gov/pubmed/36154444?tool=bestpractice.com
Image analysis-based tools are in development.[233]Gul I, Liu C, Yuan X, et al. Current and perspective sensing methods for monkeypox virus. Bioengineering (Basel). 2022 Oct 18;9(10):571.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9598380
http://www.ncbi.nlm.nih.gov/pubmed/36290539?tool=bestpractice.com
[250]Thieme AH, Zheng Y, Machiraju G, et al. A deep-learning algorithm to classify skin lesions from mpox virus infection. Nat Med. 2023 Mar;29(3):738-47.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10033450
http://www.ncbi.nlm.nih.gov/pubmed/36864252?tool=bestpractice.com
Differential diagnosis
The rash may be confused with other diseases that are more commonly encountered in clinical practice.[51]Centers for Disease Control and Prevention. Clinical overview of monkeypox. Apr 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-overview/index.html
[251]Hussain A, Kaler J, Lau G, et al. Clinical conundrums: differentiating monkeypox from similarly presenting infections. Cureus. 2022 Oct;14(10):e29929.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9634140
http://www.ncbi.nlm.nih.gov/pubmed/36348880?tool=bestpractice.com
Keep in mind possible differential diagnoses as these are far more likely to be the cause (mpox is usually rare but may be more common in certain populations in the event of an outbreak).
Clinical features may easily be confused with some STIs or other etiologies of proctitis. Therefore, it is important to comprehensively evaluate patients presenting with genital/perianal ulcers or proctitis for STIs, and to consider mpox in the differential diagnosis. However, STI coinfections are possible, and the presence of an STI does not rule out mpox.
Coinfections with other infectious agents that cause similar symptoms are also possible (e.g., severe acute respiratory syndrome coronavirus 2 [SARS-CoV-2], group A streptococcus).[252]El-Qushayri AE, Reda A, Shah J. COVID-19 and monkeypox co-infection: a rapid systematic review. Front Immunol. 2022 Dec 14;13:1094346.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9794570
http://www.ncbi.nlm.nih.gov/pubmed/36591217?tool=bestpractice.com
[253]Kaiser RM, Cash-Goldwasser S, Lehnertz N, et al. Pharyngeal co-infections with monkeypox virus and group A streptococcus, United States, 2022. Emerg Infect Dis. 2023 Sep;29(9):1855-8.
https://wwwnc.cdc.gov/eid/article/29/9/23-0469_article
http://www.ncbi.nlm.nih.gov/pubmed/37437558?tool=bestpractice.com
SARS-CoV-2 positivity and influenza-like symptoms should not exclude testing for mpox in a high-risk individual.[252]El-Qushayri AE, Reda A, Shah J. COVID-19 and monkeypox co-infection: a rapid systematic review. Front Immunol. 2022 Dec 14;13:1094346.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9794570
http://www.ncbi.nlm.nih.gov/pubmed/36591217?tool=bestpractice.com
Children and adolescents
The rash may be confused with other rash illnesses that are common in children (e.g., chickenpox, hand-foot-and-mouth disease, measles, scabies, molluscum contagiosum, allergic skin rashes, drug reactions). Children and adolescents presenting with signs and symptoms suspicious for mpox should be tested, particularly if they meet epidemiologic criteria.[33]Centers for Disease Control and Prevention. Clinical considerations for monkeypox in children and adolescents in the U.S. Aug 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-care/pediatric.html
Pregnancy
The cause of fever may be difficult to differentiate from other infections (e.g., chorioamnionitis) until the rash appears. A rash in a pregnant woman with risk factors for mpox needs to be differentiated from dermatoses of pregnancy.[135]Centers for Disease Control and Prevention. Monkeypox clinical care and treatment during pregnancy. Aug 2025 [internet publication].
https://www.cdc.gov/monkeypox/hcp/clinical-care/pregnancy.html
Common causes of a vesiculopustular rash in pregnant women (e.g., varicella zoster, syphilis, herpes simplex) can be excluded with PCR testing.[136]Dashraath P, Nielsen-Saines K, Rimoin A, et al. Monkeypox and pregnancy: virology, clinical presentation, and obstetric management. Am J Obstet Gynecol. 2022 Dec;227(6):849-61.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9534101
http://www.ncbi.nlm.nih.gov/pubmed/35985514?tool=bestpractice.com

