This page compiles our content related to dermatitis. For further information on diagnosis and treatment, follow the links below to our full BMJ Best Practice topics on the relevant conditions and symptoms.
Introduction
Relevant conditions
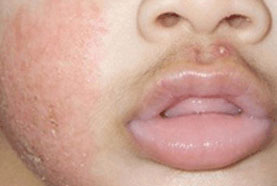
Atopic dermatitis | go to our full topic on Atopic dermatitis Atopic dermatitis is characterized by dry, pruritic skin with a chronic relapsing course. One systematic review reported 12-month atopic dermatitis prevalence of 1.8% to 17.0% in children in Europe, and 0.94% to 22.6% in children in Asia.[1] Atopic dermatitis has a multifactorial etiology, with a combination of genetic susceptibility and environmental factors contributing to disease development. Typically there is erythema, scaling, vesicles, or lichenification in skin flexures. In infants, the extensor surfaces, cheeks, scalp, and forehead are preferentially affected.[2] Patients often have a personal or family history of other atopic diseases such as asthma or allergic rhinitis.[2][3][4] Can be described as acute or chronic. Acute atopic dermatitis is used to describe a flare-up of symptoms. Chronic atopic dermatitis is used to describe the condition when the patient develops signs of chronic inflammation (e.g., lichenification). Diagnosis is primarily clinical.[Figure caption and citation for the preceding image starts]: Acute atopic dermatitis on the face of an infantPersonal collection of Dr A. Hebert [Citation ends]. |
|---|---|
Contact dermatitis | go to our full topic on Contact dermatitis Irritant contact dermatitis (ICD) is caused by direct toxicity and can occur in any person without prior sensitization, whereas allergic contact dermatitis is a delayed hypersensitivity reaction. In one meta-analysis of 28 studies of over 20,000 individuals, the worldwide prevalence of contact dermatitis in the general population is estimated to be 20.1%.[5] ICD is the most common form of contact dermatitis and is due to direct, cytotoxic barrier damage. Common causes of ICD include chronic exposure to mild irritants (water, soaps, solvents, cutting fluids) or from acute exposure to more toxic agents (acids, alkalis, strong oxidizing or reducing agents, organic solvents, and gasses). Patients generally report pruritus, burning, erythema, swelling, and blistering with acute contact dermatitis, and pruritus, burning, erythema or hyperpigmentation, fissuring, and scaling with chronic contact dermatitis. The clinical presentation of contact dermatitis is highly variable, depending on the causative agent, the affected body areas, and the duration of symptoms. |
Poison ivy, oak, and sumac | go to our full topic on Poison ivy, oak, and sumac Poison ivy, oak, and sumac dermatitis is the prototypical allergic contact dermatitis of the northern US. It is caused by skin contact with soluble oleoresins (urushiols) from the poison ivy, oak, and sumac plants (Toxicodendron species), resulting in severe acute dermatitis.[6][7][8][9] Contact can result in a severe, itchy dermatitis, which often persists for 10 to 15 days. The main goal of treatment is to prevent exposure to poison ivy, oak, and sumac plants by patient education and by wearing protective clothing.[7][10][11] Immediate washing of the skin after inadvertent contact may prevent development of the allergic response. First-line treatment is corticosteroids: topically for mild to moderate cases, and orally for severe reactions. |
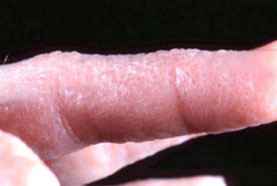
Dyshidrotic dermatitis | go to our full topic on Dyshidrotic dermatitis A form of chronic dermatitis affecting the hands and feet. Characterized by recurrent crops of 1- to 2-mm vesicles, on the palms, soles, often appearing on the medial and lateral aspects of the fingers and toes.[12] Pompholyx is a term often used synonymously with dyshidrotic dermatitis, but it is better used to describe more acute, severe eruptions of large bullae on the hands and feet.[13] An analysis of insurance claims for dyshidrotic atopic dermatitis from 27 million people in the US with private healthcare coverage revealed 34,932 patients were diagnosed in 2018 with 214,974 visits in that year. The average age was 37.1 years and most patients (61.0%) were female.[14] The common exacerbating factor is irritation, as seen in frequent hand washing, hyperhidrosis, and stress. However, the underlying etiology is unknown. Diagnosis is based on characteristic history and physical exam. [Figure caption and citation for the preceding image starts]: Dyshidrotic eczemaPhotograph courtesy of Dr Spencer Holmes, MD [Citation ends]. |
Seborrheic dermatitis | 访问我们的完整专题Seborrheic dermatitis A common inflammatory skin disorder that usually manifests as erythema and scaling of the scalp, nasolabial folds, glabella, and occasionally central face and anterior chest. It tends to worsen with stress.[15] The adult scalp form is commonly termed dandruff or pityriasis capitis. Seborrheic dermatitis is common, with a prevalence of about 1% to 3% in adults living with immunocompetency.[16] It has a variable course that seldom completely subsides. An infant form (cradle cap) usually resolves within the first few months of life. Key risk factors include HIV infection, and age <3 months. Characteristic history and physical exam findings are usually sufficient to diagnose the condition.[Figure caption and citation for the preceding image starts]: Seborrheic dermatitis, glabella, with scaling and mild erythemaPersonal collection of Dr Robert A. Schwartz [Citation ends]. |
Diaper rash | Inflammation of the skin in the area of the body covered by a diaper. It is primarily an ICD. The key irritants are moisture from urine and feces as well as fecal enzymes (ureases, proteases, and lipases). It is most common in the first 2 years of life, but can occur in any person who routinely wears diapers. Key risk factors include young age (<2 years), history of diarrhea, underlying dermatologic disorder, infrequent diaper changes, excess use of baby care products, plastic underpants, and no diaper-free time. Diagnosis is made by characteristic skin findings in the area of the body covered by a diaper; erythema of the convex surfaces of the buttocks is the classic finding. |
Lichen simplex chronicus | ir para nosso tópico completo sobre Lichen simplex chronicus Lichen simplex chronicus (LCS; also known as neurodermatitis) is a common cutaneous disorder characterized by well-circumscribed erythematous, often hyperpigmented, patches and plaques of thickened lichenified skin. LSC is a common disease, with an estimated prevalence of 12%.[17] It most commonly occurs on the neck, ankles, scalp, pubis, vulva, scrotum, and extensor forearms as a result of chronic scratching and rubbing.[18] LSC patches or plaques can arise on skin affected by an underlying dermatosis such as atopic dermatitis, allergic contact dermatitis, stasis dermatitis, superficial fungal (tinea and candidiasis) and dermatophyte infections, lichen sclerosis, viral warts, scabies, lice, an arthropod bite, or a cutaneous neoplasia.[18][19] Several risk factors are associated with the development of LSC including atopic diathesis, environmental irritants, psychiatric disorders, and dermatologic disease. Characteristic history and physical exam findings are normally sufficient for the diagnosis of LSC.[20] [Figure caption and citation for the preceding image starts]: Secondary lichen simplex chronicus in the setting of atopic dermatitisPersonal collection of Dr Swick [Citation ends]. |
Sunburn | ir para nosso tópico completo sobre Sunburn An acute inflammatory reaction of the skin induced by overexposure to ultraviolet (UV) radiation that exceeds the individual’s minimal erythema dose. Skin findings include erythema and edema, with or without vesiculation, followed by desquamation. Symptoms include pain and/or pruritus. In the UK, a 2022 survey found that 40% of adults reported at least one episode of sunburn in the past year, with this percentage increasing to 56% with young people (ages 18-34 years).[21] Key risk factors include Fitzpatrick skin types I-III, photo-sensitizing drug, intentional tanning, and lack of or improper use of sunscreen. Primary prevention is critical, as cellular damage caused by UV radiation is irreversible and may with time increase the risk of skin cancer. Characteristic history and physical exam findings are usually sufficient to make the diagnosis of sunburn. |
Evaluation of pruritus | ir para nosso tópico completo sobre Evaluation of pruritus An unpleasant sensation that causes a desire to scratch. The most subjective symptom in dermatology is itching, which may occur with or without visible skin lesions. Pruritus can be either acute or chronic, with the chronic form lasting for 6 weeks or longer.[22] Chronic pruritus may be classified as being of dermatologic, systemic, neurologic, psychogenic/psychosomatic, mixed, or unknown etiology. Pruritus is a subjective sensation; therefore, the diagnosis is based solely on the patient's symptoms. During clinical evaluation, it is important to identify a possible cause or disease responsible for itching, as well as determining the intensity and timeframe of the pruritus. A detailed history must also be collected regarding the concomitant symptoms, coexistent diseases, and medical problems, as well as drugs taken by the patient.[23] |
Evaluation of rash in children | ir para nosso tópico completo sobre Evaluation of rash in children Rash in children is common. A rash may be categorized as maculopapular, pustular, vesiculobullous, diffuse/erythematous, or petechial/purpuric in nature. Initial considerations in evaluating a rash in children include its morphology, duration, and distribution. Age, sex, family history, medications, known allergies, and exposures are also of primary importance. The primary differential diagnoses to consider for any rash presenting in childhood are viral exanthems, inflammatory dermatoses, local bacterial, fungal, or parasitic infections, tick-borne disease, drug eruptions, systemic bacterial infections, anaphylactic reactions, hematologic disorders, and vasculitic and rheumatologic conditions. |
Evaluation of dermatologic disorders in HIV | ir para nosso tópico completo sobre Evaluation of dermatologic disorders in HIV Dermatologic disorders in HIV may be categorized as infectious, inflammatory, neoplastic, drug reaction, and metabolic. The dermatologic manifestations of HIV are protean and often multiple in people living with HIV. HIV-specific dermatoses include HIV-related lipodystrophy, eosinophilic folliculitis, oral hairy leukoplakia, papular pruritic eruption of HIV, and HIV photodermatitis. Some skin diseases that appear in non-HIV-infected populations may have altered presentation in people living with HIV. Seborrheic dermatitis occurs with strikingly increased prevalence in people living with HIV.[24][25] Atopic dermatitis has a high prevalence in adult as well as pediatric populations with HIV.[26] Toxic epidermal necrolysis/Stevens-Johnson Syndrome must be recognized immediately, as this is a potentially life-threatening condition. |
Colaboradores
Autores
Editorial Team
BMJ Publishing Group
Declarações
This overview has been compiled using the information in existing sub-topics.
Referências
Artigos de referência
Uma lista completa das fontes referenciadas neste tópico está disponível para os usuários com acesso total ao BMJ Best Practice.
Folhetos informativos para os pacientes
Dermatitis
Eczema
Mais Folhetos informativos para os pacientesConectar-se ou assinar para acessar todo o BMJ Best Practice
O uso deste conteúdo está sujeito ao nosso aviso legal