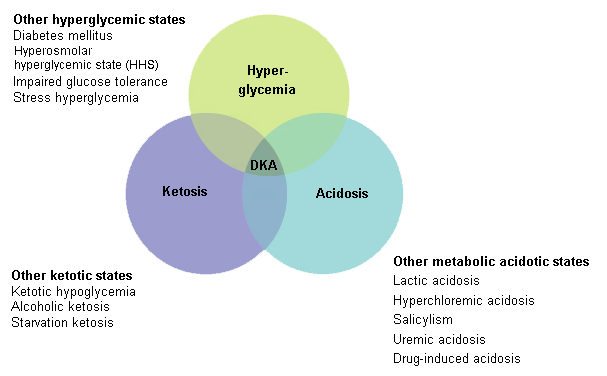
Summary
Definition
History and exam
Other diagnostic factors
- polyuria
- polyphagia
- polydipsia
- weight loss
- weakness
- nausea or vomiting
- abdominal pain
- dry mucous membranes
- poor skin turgor
- sunken eyes
- tachycardia
- hypotension
- Kussmaul respiration
- acetone breath
- altered mental status
- hypothermia
Risk factors
- type 1 diabetes
- inadequate or inappropriate insulin therapy
- infection
- myocardial infarction
- previous episode of hyperglycemic or hypoglycemic crisis
- high hemoglobin A1c (HbA1c)
- adverse social determinants of health
- age <45 years
- presence of other diabetes-related complications
- presence of other chronic health conditions
- pancreatitis
- stroke
- acromegaly
- hyperthyroidism
- use of certain drugs
- Cushing syndrome
- Hispanic, Asian, or black ancestry
- bariatric surgery
- prolonged fasting or carbohydrate restriction
- pregnancy
- dementia
- mental health disorders
- alcohol and/or substance use
Diagnostic tests
1st tests to order
- plasma glucose
- ABG
- capillary or serum ketones
- urinalysis
- serum BUN
- serum creatinine
- serum sodium
- serum potassium
- serum chloride
- serum magnesium
- serum phosphate
- anion gap calculation
- serum lactate
- LFT
- serum amylase
- serum lipase
- serum osmolality
- CBC
- ECG
Tests to consider
- serum creatine kinase (CK)
- CXR
- high-sensitivity cardiac troponin
- blood, urine, or sputum cultures
Treatment algorithm
Contributors
Expert advisers
Aidar R. Gosmanov, MD, PhD, FACE
Associate Professor of Medicine
Division of Endocrinology
Albany Medical College
Chief, Endocrinology Section
Albany VAMC
Albany, NY
Disclosures
ARG declares that he has no competing interests.
Laleh Razavi Nematollahi, MD
Assistant Professor of Medicine
Cleveland Clinic Lerner College of Medicine
Case Western Reserve University
Cleveland, OH
Disclosures
LRN declares that she has no competing interests.
Acknowledgements
Dr Aidar Gosmanov and Dr Laleh Razavi Nematollahi would like to gratefully acknowledge Professor Abbas E. Kitabchi, the previous contributor to this topic.
Disclosures
AEK is an author of a number of references in this topic.
Peer reviewers
David Jenkins, DM, FRCP
Consultant Physician
Worcestershire Royal Hospital
Worcester
UK
Disclosures
DJ declares that he has no competing interests.
Udaya M. Kabadi, MD, FRCP(C), FACP, FACE
Professor of Medicine
University of Iowa
Iowa City, IA
Disclosures
UMK declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Umpierrez GE, Davis GM, ElSayed NA, et al. Hyperglycaemic crises in adults with diabetes: a consensus report. Diabetologia. 2024 Aug;67(8):1455-79.Full text Abstract
American Diabetes Association. Standards of care in diabetes - 2025. Diabetes Care. 2025 Jan;48(suppl 1):S1-352.Full text
Dhatariya KK, Glaser NS, Codner E, et al. Diabetic ketoacidosis. Nat Rev Dis Primers. 2020 May 14;6(1):40. Abstract
Umpierrez G, Korytkowski M. Diabetic emergencies - ketoacidosis, hyperglycaemic hyperosmolar state and hypoglycaemia. Nat Rev Endocrinol. 2016 Apr;12(4):222-32. Abstract
Reference articles
A full list of sources referenced in this topic is available here.
Use of this content is subject to our disclaimer