Summary
Definition
History and exam
Key diagnostic factors
- fever
Other diagnostic factors
- nausea and vomiting
- dysuria, frequency, or urgency
- flank pain or costovertebral angle tenderness
Risk factors
- urinary tract infection
- diabetes mellitus
- stress incontinence
- foreign body in urinary tract (e.g., calculus, catheter)
- anatomic/functional urinary abnormality
- immunosuppressive state
- pregnancy
- frequent sexual intercourse
- mother with urinary tract infection history
- new sex partner
- spermicide use
- age between 18 and 50 years
- age >60 years
Diagnostic tests
1st tests to order
- urinalysis
- Gram stain
- urine culture
- complete blood count
- erythrocyte sedimentation rate
- C-reactive protein
- blood culture
Tests to consider
- renal ultrasound
- contrast-enhanced spiral computed tomography
- magnetic resonance imaging
- procalcitonin
Emerging tests
- interleukin
- copeptin
Treatment algorithm
high index of suspicion with mild-to-moderate symptoms confined to the kidneys: nonpregnant
high index of suspicion with severe disease or with complicating factors: nonpregnant
high index of suspicion with any disease severity: pregnant
mild-to-moderate symptoms confined to the kidneys: nonpregnant
severe disease or with complicating factors: nonpregnant
any disease severity: pregnant
recurrent disease within 1 to 2 weeks
Contributors
Expert advisers
Lynda A. Frassetto, MD
Professor of Medicine
Division of Nephrology
University of California
San Francisco, CA
Disclosures
LAF declares that she has no competing interests.
Acknowledgements
Dr Lynda A. Frassetto would like to gratefully acknowledge the assistance of Donna M. Frassetto.
Disclosures
DMF declares that she has no competing interests.
Peer reviewers
John Lam, MD
Attending Urologist
Providence Saint Joseph Medical Center
Burbank
Assistant Clinical Professor of Urology
Department of Urology
David Geffen School of Medicine at UCLA
Los Angeles, CA
Disclosures
JL declares that he has no competing interests.
Robert Mactier, MD, FRCP
Consultant Nephrologist/Lead Clinician
Renal Unit
Glasgow Royal Infirmary
NHS Greater Glasgow and Clyde
Glasgow
UK
Disclosures
RM declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Trautner BW, Cortes-Penfield NW, Gupta K, et al. IDSA 2025 guideline update on complicated urinary tract infections. Jul 2025 [internet publication].Full text
European Association of Urology. EAU guidelines on urological infections. 2025 [internet publication].Full text
Tamma PD, Heil EL, Justo JA, et al. Infectious Diseases Society of America 2024 guidance on the treatment of antimicrobial-resistant gram-negative infections. Clin Infect Dis. 2024 Aug 7:ciae403.Full text Abstract
Glaser AP, Schaeffer AJ. Urinary tract infection and bacteriuria in pregnancy. Urol Clin North Am. 2015 Nov;42(4):547-60. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
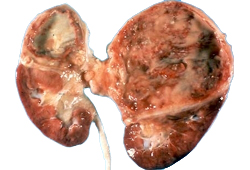
Differentials
- Chronic pyelonephritis
- Pelvic inflammatory disease
- Pelvic pain syndrome
More DifferentialsGuidelines
- EAU guidelines on urological infections
- IDSA 2025 guideline update on complicated urinary tract infections
More GuidelinesPatient information
Kidney infection
Kidney stones
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer