Summary
Definition
History and exam
Key diagnostic factors
- myasthenia gravis
- muscle weakness
- facial and upper extremity edema
- facial plethora
- distended veins in the neck, chest and/or abdominal wall
- left-arm swelling
Other diagnostic factors
- cough
- dyspnea
- fever and/or weight loss
Risk factors
- history of myasthenia gravis
- age >45 years
Diagnostic tests
1st tests to order
- chest x-ray
- chest CT with intravenous contrast medium
Tests to consider
- chest MRI
- tissue biopsy
- acetylcholine receptor antibodies
- CBC
- PET/CT scan
- serum alpha-fetoprotein (AFP)
- serum beta-human chorionic gonadotropin (beta-hCG)
Treatment algorithm
resectable tumor
locally advanced tumor
recurrent tumor
Contributors
Authors
Douglas Z. Liou, MD
Clinical Associate Professor of Cardiothoracic Surgery
Division of Thoracic Surgery
Stanford University School of Medicine / Stanford Cancer Institute
Stanford
CA
Disclosures
DZL declares that he has no competing interests.
Joseph B. Shrager, MD
Professor of Cardiothoracic Surgery
Chief, Division of Thoracic Surgery
Medical Director, Thoracic Oncology CCP
Stanford University School of Medicine / Stanford Cancer Institute
Stanford
CA
Disclosures
JBS declares that he has no competing interests.
Nathaniel J. Myall, MD
Clinical Assistant Professor of Medical Oncology
Stanford University School of Medicine / Stanford Cancer Institute
Stanford
CA
Disclosures
NJM has received research funding from Genentech.
Kavitha Ramchandran, MD
Professor of Medical Oncology
Stanford University School of Medicine / Stanford Cancer Institute
Stanford
CA
Disclosures
KR has been compensated for consulting services by Varian Medical Systems and Curio Bioscience. She has served on the advisory council for Group Well and Pathomiq and has received honorarium from the Binaytara Foundation for speaking at a conference.
Lucas Kas Vitzthum, MD
Clinical Assistant Professor of Radiation Oncology
Department of Radiation Oncology
Stanford University School of Medicine
Stanford
CA
Disclosures
LKV declares that he has no competing interests.
Acknowledgements
Dr Douglas Z. Liou, Dr Joseph B. Shrager, Dr Nathaniel J. Myall, Dr Kavitha Ramchandran, and Dr Lucas Kas Vitzthum would like to gratefully acknowledge Dr Tracey Evans, Dr Nicholas Choong, Dr Mario Gasparri, and Dr Cameron Wright, previous contributors to this topic.
Disclosures
TE has received consultancy fees from Genentech and Celgene. She is a board member of Wissahickon Hospice. Educational events include an annual thoracic educational series sponsored by Imedex. NC and MG declare that they have no competing interests. CW is an author of a number of references cited in this topic.
Peer reviewers
Enrico Ruffini, MD
Associate Professor
Thoracic Surgery
University of Torino
Torino
Italy
Disclosures
ER is an author of a reference cited in this topic.
James R. Jett, MD
Emeritus Professor of Medicine
National Jewish Health
Denver
CO
Disclosures
JRJ is co-editor of the section on thymoma in Up To Date. He is also co-chief medical officer for Biodesix Inc.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Girard N, Ruffini E, Marx A, et al. Thymic epithelial tumours: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2015;26(suppl 5):v40-v55.Full text Abstract
Phan AT, Öberg K, Choi J, et al. NANETS consensus guideline for the diagnosis and management of neuroendocrine tumors: well-differentiated neuroendocrine tumors of the thorax (includes lung and thymus). Pancreas. 2010;39:784-98.Full text Abstract
National Comprehensive Cancer Network. NCCN clinical practice guidelines in oncology: thymomas and thymic carcinomas [internet publication].Full text
Baudin E, Caplin M, Garcia-Carbonero R, et al. Lung and thymic carcinoids: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2021 Apr;32(4):439-51.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
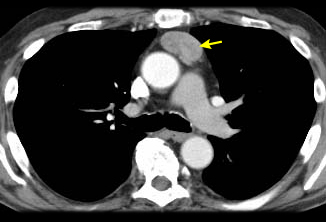
Differentials
- Lymphoma
- Malignant mediastinal germ cell tumor: seminoma
- Malignant mediastinal germ cell tumor: nonseminoma
More DifferentialsGuidelines
- NCCN clinical practice guidelines in oncology: thymomas and thymic carcinomas
- The Society of Thoracic Surgeons expert consensus document on the surgical management of thymomas
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer