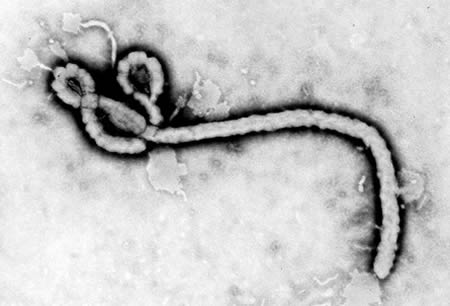
WHO declares DRC and Uganda outbreak a global public health emergency
The World Health Organization (WHO) has declared the Ebola outbreak in the Democratic Republic of the Congo (DRC) and Uganda a public health emergency of international concern (PHEIC). PHEIC status aims to accelerate funding, research, and international public health measures and co-operation to contain a disease.
This outbreak is caused by the Bundibugyo virus, one of three species of orthoebolaviruses known to cause disease in humans. Prior to this outbreak, there have only been two outbreaks of the disease caused by Bundibugyo virus: Uganda in 2007 and the DRC in 2012.
The first currently known suspected case in this outbreak was a health worker who first reported symptoms on 24 April 2026. The WHO was alerted to an outbreak of an unknown illness with high mortality in the Ituri Province on 5 May 2026. Subsequent laboratory testing confirmed Bundibugo virus in 8 out of 13 samples on 15 May 2026. This is the seventeenth Ebola outbreak in the DRC.
As of 19 May 2026, at least 536 suspected cases, 105 probable cases, 34 laboratory-confirmed cases, and 134 deaths have been reported by the DRC and Uganda Ministries of Health. This includes 2 confirmed cases in Uganda in people who traveled from the DRC. No further spread has been reported in Uganda.[31]
The situation is rapidly developing, and you should consult your local public health authority for current information on the situation. Information is available from the WHO, the Centers for Disease Control and Prevention (CDC), and the UK Health Security Agency (UKHSA).
There are a number of reasons for the WHO declaring a PHEIC for this outbreak including:[32]
Significant uncertainty about the true number of infected people and geographic spread at the present time. Also, there is limited understanding of the epidemiologic links with known or suspected cases. Early data point toward a potentially much larger outbreak than what is being detected and reported.
Cases have already been reported in Uganda; therefore, neighboring countries such as South Sudan are considered to be at high risk of further spread.
There is ongoing insecurity and a humanitarian crisis in the region.
There are currently no known vaccines or specific therapeutics for Bundibugyo virus.
The case fatality rate for disease caused by the Bundibugyo virus ranges from 30% to 50%, according to the WHO, although data vary based on whether laboratory-confirmed cases or suspected cases were used to calculate the rate.
The WHO has not advised any travel restrictions. However, travel notices are in place for the DRC and Uganda in some countries, and you should check your local government guidance for more information before traveling to these regions. Enhanced travel screening and entry restrictions have been instituted in countries outside of East and Central Africa.
Summary
Definition
History and exam
Key diagnostic factors
- exposure to an orthoebolavirus in previous 21 days
- fever
- myalgia
- conjunctival injection
Other diagnostic factors
- fatigue
- anorexia
- diarrhea
- vomiting
- severe headache
- abdominal pain or heartburn
- cough, dyspnea, chest pain
- sore throat
- prostration
- tachypnea
- maculopapular rash
- bleeding
- hepatomegaly
- lymphadenopathy
- hiccups
- tachycardia
- hypotension
- neurologic signs
Risk factors
- living or working in, or arrival from, endemic area in previous 21 days
- contact with infected body fluids
- occupational exposure
- butchering or consumption of meat from infected (or potentially infected) animals
- bioterrorism
Diagnostic tests
1st tests to order
- reverse transcriptase-polymerase chain reaction (RT-PCR)
- malaria investigations
Tests to consider
- serum electrolyte levels
- BUN/serum creatinine
- blood lactate
- ABG
- CBC
- coagulation studies
- urinalysis
- LFTs
- serum amylase level
- blood cultures
- serum blood glucose
- antigen-capture enzyme-linked immunosorbent assay (ELISA)
- serology
- chest x-ray
Treatment algorithm
Contributors
Authors
Catherine F. Houlihan, MSc, MB ChB, MRCP, DTM&H
Clinical Lecturer
University College London
Honorary Clinical Lecturer
London School of Hygiene and Tropical Medicine
London
UK
Disclosures
CFH declares that she has no competing interests.
Manuel Fenech, MD, MRCP, DTM&H
Specialist Trainee in Infectious Diseases
Royal Liverpool University Hospital
Liverpool
UK
Disclosures
MF declares that he has no competing interests.
Tom E. Fletcher, MBE, MBChB, MRCP, DTM&H
Wellcome Trust/MoD Research Fellow
Liverpool School of Tropical Medicine
Liverpool
UK
Disclosures
TEF is an author of a number of references cited in this monograph. TEF is a consultant/expert panel member to the World Health Organization, and is funded by the UK Surgeon General and the Wellcome Trust. TEF has received research grants from the Medical Research Council and the UK Public Health Rapid Support Team (UK-PHRST).
Acknowledgements
Dr Catherine F. Houlihan, Dr Manuel Fenech, and Dr Tom E. Fletcher would like to thank Dr Nicholas J. Beeching, a previous contributor to this topic, and Dr Colin Brown (Infectious Disease Lead, Kings Sierra Leone Partnership) for his helpful comments and insights.
Disclosures
NJB was partially supported by the National Institute of Health Research Health Protection Unit in Emerging and Zoonotic Infections at the University of Liverpool and Public Health England. NJB is an author of references cited in this topic. CB declares that he has no competing interests.
Peer reviewers
William A. Petri, Jr, MD, PhD, FACP
Wade Hampton Frost Professor of Epidemiology
Professor of Medicine, Microbiology, and Pathology
Chief
Division of Infectious Diseases and International Health
University of Virginia
Charlottesville
VA
Disclosures
WAP declares that he has no competing interests.
Luis Ostrosky-Zeichner, MD, FACP, FIDSA, FSHEA
Professor of Medicine and Epidemiology
UT Health Medical School
Medical Director of Epidemiology
Memorial Hermann Texas Medical Center
Houston
TX
Disclosures
LO-Z declares that he has no competing interests.
Stephen Mepham, MRCP (UK), FRCPATH, DTM&H, MD
Consultant in Microbiology and Infectious Diseases
Royal Free London NHS Foundation Trust
London
UK
Disclosures
SM declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
World Health Organization. Clinical care for survivors of Ebola virus disease: interim guidance. Apr 2016 [internet publication].Full text
World Health Organization. Guidelines for the management of pregnant and breastfeeding women in the context of Ebola virus disease. 2020 [internet publication].Full text
World Health Organization. Infection prevention and control guideline for Ebola and Marburg diseases. May 2026 [internet publication].Full text
World Health Organization. Optimized supportive care for Ebola virus disease. July 2019 [internet publication].Full text
Lamontagne F, Fowler RA, Adhikari NK, et al. Evidence-based guidelines for supportive care of patients with Ebola virus disease. Lancet. 2018 Feb 17;391(10121):700-8.Full text Abstract
World Health Organization. Clinical management of patients with viral haemorrhagic fever: a pocket guide for front-line health workers. Feb 2016 [internet publication].Full text
World Health Organization. Therapeutics for Ebola virus disease - Democratic Republic of the Congo. Aug 2022 [internet publication].Full text
Reference articles
A full list of sources referenced in this topic is available here.
Use of this content is subject to our disclaimer