Резюме
Определение
Анамнез и осмотр
Ключевые диагностические факторы
- presença de fatores de risco
- primeiro trimestre da gestação
- sangramento vaginal
- tamanho uterino incomum para a idade gestacional
Другие диагностические факторы
- pré-eclâmpsia de início precoce
- dispneia e desconforto respiratório
- náuseas e vômitos intensos
- taquicardia, tremor, insônia e diarreia
- palidez
- dor pélvica
- sangramento uterino
Факторы риска
- extremidades etárias maternas
- gravidez molar prévia
- gordura e caroteno reduzidos na dieta
Диагностические исследования
Исследования, которые показаны в первую очередь
- exame histológico do tecido placentário
- gonadotrofina coriônica humana (hCG) sérica
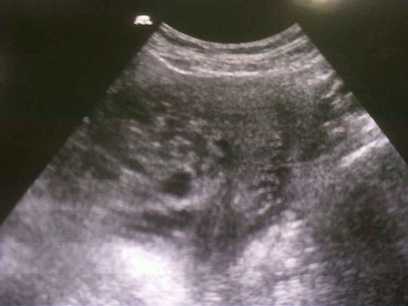
- ultrassonografia pélvica
Исследования, проведение которых нужно рассмотреть
- Hemograma completo
- tempo de protrombina (TP), tempo de tromboplastina parcial (TTP) séricos
- perfil metabólico sérico
- hormônio estimulante da tireoide (TSH) sérico
- tipagem sanguínea com rastreamento de anticorpos
- radiografia torácica
Алгоритм лечения
gravidez molar única: pacientes que desejam manter a fertilidade
gravidez molar única: pacientes que não desejam manter a fertilidade
feto gêmeo viável: interrupção eletiva não desejada
feto gêmeo viável: interrupção eletiva
após o manejo inicial: alto risco de neoplasia trofoblástica gestacional com conclusão do acompanhamento improvável
Составители
Авторы
Antonio Braga, MD
Associate Professor
Department of Obstetrics and Gynecology
Rio de Janeiro Federal University
Department of Maternal Child
Fluminense Federal University
Rio de Janeiro
Brazil
Раскрытие информации
AB is an author of references cited in this topic.
Kevin M. Elias, MD
Assistant Professor
Brigham and Women’s Hospital
Dana Farber Cancer Institute
New England Trophoblastic Disease Center
Division of Gynecologic Oncology
Department of Obstetrics, Gynecology and Reproductive Biology
Harvard Medical School
Boston
MA
Раскрытие информации
KME has been a paid consultant for AOA Dx and received research support from Aspira Women’s Health and Abcam, Inc. KME is an author of references cited in this topic.
Neil S. Horowitz, MD
Associate Professor
Brigham and Women’s Hospital
Dana Farber Cancer Institute
New England Trophoblastic Disease Center
Division of Gynecologic Oncology
Department of Obstetrics, Gynecology and Reproductive Biology
Harvard Medical School
Boston
MA
Раскрытие информации
NSH is an author of references cited in this topic.
Ross S. Berkowitz, MD
William H. Baker Professor of Gynecology
Brigham and Women’s Hospital
Dana Farber Cancer Institute
New England Trophoblastic Disease Center
Division of Gynecologic Oncology
Department of Obstetrics, Gynecology and Reproductive Biology
Harvard Medical School
Boston
MA
Раскрытие информации
RSB is an author of references cited in this topic.
Выражение благодарностей
Dr Ross S. Berkowitz, Dr Kevin M. Elias, Dr Neil S. Horowitz, and Dr Antonio Braga would like to gratefully acknowledge Dr John Soper and Dr Emma Rossi, previous contributors to this topic. JS and ER declare that they have no competing interests.
Рецензенты
Jane Stewart, PhD, MSc
Consultant Gynecologist
Subspecialist in Reproductive Medicine
Newcastle Fertility Centre at Life
Bioscience Centre
International Centre at Life
Newcastle upon Tyne
UK
Раскрытие информации
JS declares that she has no competing interests.
Philip Savage, PhD, FRCP
Consultant in Medical Oncology
Department of Medical Oncology
Charing Cross Hospital
London
UK
Раскрытие информации
PS declares that he has no competing interests.
Aparna Sundaram, DO, MBA, MPH
Physician Consultant
Preventive Medicine
Private Practice
Atlanta
GA
Раскрытие информации
AS declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
Список литературы
Основные статьи
Horowitz NS, Eskander RN, Adelman MR, et al. Epidemiology, diagnosis, and treatment of gestational trophoblastic disease: A Society of Gynecologic Oncology evidenced-based review and recommendation. Gynecol Oncol. 2021 Dec;163(3):605-13.Полный текст Аннотация
Ngan HYS, Seckl MJ, Berkowitz RS, et al. Diagnosis and management of gestational trophoblastic disease: 2021 update. Int J Gynaecol Obstet. 2021 Oct;155 Suppl 1(suppl 1):86-93.Полный текст Аннотация
Tidy, J, Seckl, M, Hancock, BW, on behalf of the Royal College of Obstetricians and Gynaecologists. Management of gestational trophoblastic disease. BJOG 2021;128: e1-e27.Полный текст
Lok C, van Trommel N, Massuger L, et al. Practical clinical guidelines of the EOTTD for treatment and referral of gestational trophoblastic disease. Eur J Cancer. 2020 May;130:228-40. Аннотация
Статьи, указанные как источники
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Отличия
- Hiperêmese gravídica
- Aborto espontâneo
- Gestação múltipla
Больше ОтличияРекомендации
- Diagnosis and treatment of gestational trophoblastic disease
- Epidemiology, diagnosis, and treatment of gestational trophoblastic disease
Больше РекомендацииВойдите в учетную запись или оформите подписку, чтобы получить полноценный доступ к BMJ Best Practice
Использование этого контента попадает под действие нашего заявления об отказе от ответственности