Resumen
Definición
Anamnesis y examen
Principales factores de diagnóstico
- dolor abdominal
- abdomen doloroso a la palpación
- presencia de factores de riesgo
Otros factores de diagnóstico
- hematoquecia/melena
- diarrea
- náuseas
- pérdida de peso
- soplo abdominal
- vasculitis
- aturdimiento, palidez, disnea
- miedo a ingerir alimentos (sitofobia)
Factores de riesgo
- edad avanzada
- antecedentes de tabaquismo
- estados de hipercoagulabilidad
- fibrilación auricular
- infarto de miocardio
- defectos estructurales del corazón
- antecedentes de vasculitis
- cirugía cardiovascular reciente
- shock
- insuficiencia cardíaca congestiva
- aterosclerosis
- síndrome del intestino irritable
- carcinoma colónico
- estreñimiento
- uso de laxantes a largo plazo
- uso de vasopresores, digoxina, cocaína
Pruebas diagnósticas
Primeras pruebas diagnósticas para solicitar
- exploración por tomografía computarizada (TC)/angiografía por TC
- hemograma completo (HC)
- Gasometría arterial y lactato sérico
- urea y electrolitos
- pruebas de función hepática
- proteína C-reactiva
- estudios de coagulación, agrupar y guardar y comparar
- electrocardiograma (ECG)
- radiografía de tórax (RT) en bipedestación
- sigmoidoscopia o colonoscopia
- endoscopia del tracto gastrointestinal superior
- dímero D
Pruebas diagnósticas que deben considerarse
- angiografía mesentérica
- ultrasonido dúplex/doppler mesentérico
- angiografía por resonancia magnética
- amilasa
- estudios para la detección de huevos, quistes y parásitos
- cultivo fecal
- Ensayo de toxina de Clostridium difficile
- radiografías de abdomen
Algoritmo de tratamiento
evidencia de infarto, perforación o peritonitis en la tomografía computarizada diagnóstica
no hay evidencia de infarto, perforación o peritonitis en la tomografía computarizada de diagnóstico
isquemia mesentérica crónica
Colitis por isquemia
isquemia colónica no aguda
Colaboradores
Consejeros especializados
Jennifer Straatman
Consultant Upper GI surgeon
Queen Alexandra Hospital
Portsmouth
UK
Divulgaciones
JS declares that she has no competing interests.
Agradecimientos
BMJ Best Practice would like to gratefully acknowledge the previous expert contributors, whose work has been retained in parts of the content:
Alex von Roon, MB, ChB, PhD, FRCS
Clinical Senior Lecturer
Honorary Consultant Colorectal Surgeon
Department of Surgery and Cancer
Imperial College London
London
UK
James Lewis, MBBS, BSc, MRCS
Clinical Research Fellow
Department of Surgery and Cancer
Imperial College London
London
UK
John Abercrombie FRCS
General and Colorectal Surgeon
Queen’s Medical Centre
Nottingham
UK
Divulgaciones
AVR and JL declare that they have no competing interests. JA is a member of the Council of The Royal College of Surgeons of England and Clinical Lead for General Surgery, Getting It Right First Time. JA provides expert advice regarding suitability of surgical treatments for Spire Healthcare.
Revisores por pares
Frances Howse, MA (Oxon), BM (Hons), FRCS (Eng)
Consultant
Acute and General Surgery
University Hospital Southampton NHS Foundation Trust
Southampton
UK
Divulgaciones
FH declares that she has no competing interests.
Agradecimiento de los revisores por pares
Los temas de BMJ Best Practice se actualizan de forma continua de acuerdo con los desarrollos en la evidencia y en las guías. Los revisores por pares listados aquí han revisado el contenido al menos una vez durante la historia del tema.
Divulgaciones
Las afiliaciones y divulgaciones de los revisores por pares se refieren al momento de la revisión.
Referencias
Artículos principales
Bala M, Catena F, Kashuk J, et al. Acute mesenteric ischemia: updated guidelines of the World Society of Emergency Surgery. World J Emerg Surg. 2022 Oct 19;17(1):54.Texto completo Resumen
Tilsed JV, Casamassima A, Kurihara H, et al. ESTES guidelines: acute mesenteric ischaemia. Eur J Trauma Emerg Surg. 2016 Apr;42(2):253-70.Texto completo Resumen
Terlouw LG, Moelker A, Abrahamsen J, et al. European guidelines on chronic mesenteric ischaemia: joint United European Gastroenterology, European Association for Gastroenterology, Endoscopy and Nutrition, European Society of Gastrointestinal and Abdominal Radiology, Netherlands Association of Hepatogastroenterologists, Hellenic Society of Gastroenterology, Cardiovascular and Interventional Radiological Society of Europe, and Dutch Mesenteric Ischemia Study group clinical guidelines on the diagnosis and treatment of patients with chronic mesenteric ischaemia. United European Gastroenterol J. 2020 May;8(4):371-95.Texto completo Resumen
Artículos de referencia
Una lista completa de las fuentes a las que se hace referencia en este tema está disponible para los usuarios con acceso a todo BMJ Best Practice.
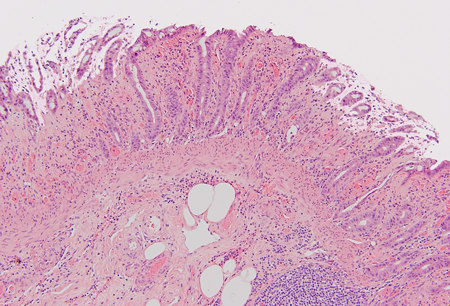
Diferenciales
- Colitis infecciosa
- Colitis ulcerosa
- Enfermedad de Crohn
Más DiferencialesGuías de práctica clínica
- Acute mesenteric ischemia
- ESTES guidelines: acute mesenteric ischaemia
Más Guías de práctica clínicaVideos
Demostración animada de como realizar un electrocardiograma (ECG)
Demostración animada de venopunción y flebotomía
Más vídeosFolletos para el paciente
Enfermedad isquémica intestinal: ¿qué es?
Enfermedad isquémica intestinal: ¿cuáles son las opciones de tratamiento?
Más Folletos para el pacienteInicie sesión o suscríbase para acceder a todo el BMJ Best Practice
El uso de este contenido está sujeto a nuestra cláusula de exención de responsabilidad