Summary
Definition
History and exam
Key diagnostic factors
- cold or numbness of affected extremity
- pain during rewarming
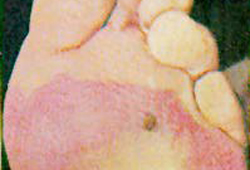
- purplish skin discoloration
- white or yellowish, waxy skin discoloration
- superficial skin vesiculation
- deep purple blisters
- tissue necrosis and mummification (dry gangrene)
Other diagnostic factors
- erythema
- joint dislocation
- fractures
Risk factors
- cold exposure
- previous frostbite
- vascular insufficiency
- high altitude
- hypoxia
- alcohol
- tobacco
- dehydration
- extremity trauma
- constrictive clothing or equipment
Diagnostic tests
1st tests to order
- clinical diagnosis
Tests to consider
- technetium-99m pertechnetate scintigraphy
- magnetic resonance angiography of affected extremity
- plain radiography
Emerging tests
- thermography and duplex imaging
Treatment algorithm
all patients
Contributors
Authors
Elizabeth A. Kaufman, MD, CAQ-SM
Attending Physician
Department of Orthopedics, Sports Medicine
Scripps Clinic
Attending Physician
Rady Children’s Hospital San Diego
Department of Orthopedics, Sports Medicine
San Diego
CA
Disclosures
EAK declares that she has no competing interests.
Christopher Imray, PhD, FRCS, FRCP, FRGS
Consultant Vascular and Renal Transplant Surgeon
University Hospital Coventry and Warwickshire NHS Trust
Professor Coventry University, Warwick Medical School, Exeter University
Coventry
UK
Disclosures
CI has been asked to provide expert testimony on frostbite. He has delivered lectures, and produced educational material on frostbite.
Acknowledgements
Professor Christopher Imray and Dr Elizabeth A. Kaufman would like to gratefully acknowledge Professor Paul S. Auerbach and Dr Claire Turchi, previous contributors to this topic. PSA and CT declare that they have no competing interests.
Peer reviewers
Luanne Freer, MD, FACEP, FAWM
Medical Director
Yellowstone National Park
WY
Founder/Director
Everest Base Camp Medical Clinic
Nepal
Disclosures
LF declares that she has no competing interests.
Grant S. Lipman, MD
Clinical Assistant Professor of Surgery and Emergency Medicine
Associate Director Wilderness Medicine Fellowship
Assistant Research Director
Stanford University School of Medicine
Palo Alto
CA
Disclosures
GSL declares that he has no competing interests.
Peter Hackett, MD
Director
Institute for Altitude Medicine
Telluride
CO
Disclosures
PH declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
McIntosh SE, Freer L, Grissom CK, et al. Wilderness Medical Society clinical practice guidelines for the prevention and treatment of frostbite: 2024 update. Wilderness Environ Med. 2024 Jun;35(2):183-97.Full text Abstract
Sheridan RL, Goverman JM, Walker TG. Diagnosis and treatment of frostbite. N Engl J Med. 2022 Jun 9;386(23):2213-20.
Rabold MB. Frostbite and other localized cold-related injuries. In: Tintinalli JE, Kelen GD, Stapczynski JS, et al. Tintinalli's emergency medicine: a comprehensive study guide. 6th ed. New York, NY: McGraw-Hill; 2004.
Roche-Nagle G, Murphy D, Collins A, et al. Frostbite: management options. Eur J Emerg Med. 2008 Jun;15(3):173-5. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Cutaneous burns
- Frostnip
- Raynaud phenomenon
More DifferentialsGuidelines
- 2024 American Heart Association and AmericanRed Cross Guidelines for First Aid
- Clinical practice guidelines for the prevention and treatment of frostbite: 2024 update
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer