Summary
Definition
History and exam
Key diagnostic factors
- primary skin lesion
- nodular lymphangitis lesions
Other diagnostic factors
- respiratory symptoms
- joint swelling/erythema
- male 30 to 60 years old
- fever
- lymphadenopathy
- meningitis-like symptoms
Risk factors
- trauma to the skin
- outdoor occupation/hobbies
- animal bites and scratches
- alcohol use disorder
- diabetes mellitus
- HIV/AIDS
- COPD
- corticosteroid treatment
- chemotherapy in patients with hematologic malignancy
- hematopoietic stem cell/solid organ transplantation
- tumor necrosis factor (TNF)-alpha inhibitor therapy
Diagnostic tests
1st tests to order
- skin lesion fungal culture
- skin lesion histopathology (Gomori methenamine silver, periodic acid-Schiff staining)
- CBC
- erythrocyte sedimentation rate
- joint x-ray
- fungal culture of arthrocentesis synovial fluid
- sputum or bronchoalveolar lavage (BAL) fungal culture
- lumbar puncture for cerebrospinal fluid analysis
- cerebrospinal fluid (CSF) fungal culture
- fungal blood culture
Tests to consider
- synovial tissue biopsy for fungal culture
- synovial tissue histopathology (Gomori methenamine silver, periodic acid-Schiff staining)
- bronchial biopsy fungal culture
- bronchial biopsy histopathology
- CXR
- CT of chest
- serum itraconazole levels
- serum BUN
- serum creatinine
- LFTs
Emerging tests
- immunohistochemical staining
- polymerase chain reaction (PCR)
Treatment algorithm
nonpregnant: lymphocutaneous/cutaneous
nonpregnant: extracutaneous mild/moderate disease
nonpregnant: extracutaneous severe/life-threatening disease
pregnant: cutaneous
pregnant: lymphocutaneous
pregnant: extracutaneous
Contributors
Authors
Michail Lionakis, MD, ScD
Chief
Fungal Pathogenesis Section
Laboratory of Clinical Immunology and Microbiology
National Institutes of Allergy and Infectious Diseases
National Institutes of Health
Bethesda
MD
Disclosures
ML declares that he has no competing interests.
John E. Bennett, MD
Chief
Clinical Mycology Section
Laboratory of Clinical Immunology and Microbiology
National Institute of Allergy and Infectious Diseases
National Institutes of Health
Bethesda
MD
Disclosures
JEB declares that he has no competing interests.
Peer reviewers
George Samonis, MD
Professor of Internal Medicine/Infectious Diseases
University of Crete
Department of Internal Medicine
Gallos University Campus
Crete
Greece
Disclosures
GS declares that he has no competing interests.
Amy Xu, MD, MA
Assistant Professor of Medicine
Section of Dermatology
University of Chicago
Chicago
IL
Disclosures
AX declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Rex JH, Okhuysen PC. Sporothrix schenckii. In Bennett JE, Dolin R, Blaser MJ, eds. Principles and practice of infectious diseases. 9th ed. Philadelphia, PA: Elsevier, 2020: 3131-6.
Orofino-Costa R, Macedo PM, Rodrigues AM, et al. Sporotrichosis: an update on epidemiology, etiopathogenesis, laboratory and clinical therapeutics. An Bras Dermatol. 2017 Sep-Oct;92(5):606-20.Full text Abstract
Kauffman CA, Bustamante B, Chapman SW, et al. Clinical practice guidelines for the management of sporotrichosis: 2007 update by the Infectious Diseases Society of America. Clin Infect Dis. 2007 Nov 15;45(10):1255-65.Full text Abstract
Sharkey-Mathis PK, Kauffman CA, Graybill JR, et al. Treatment of sporotrichosis with itraconazole. NIAID Mycoses Study Group. Am J Med. 1993 Sep;95(3):279-85. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
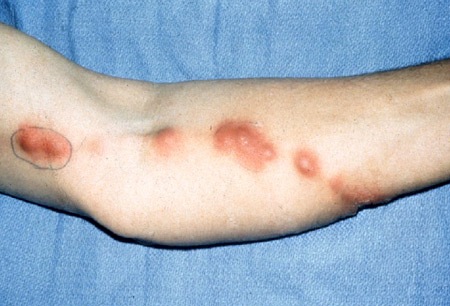
Differentials
- Primary cutaneous nocardiosis
- Cutaneous Mycobacterium marinum infection
- Cutaneous leishmaniasis
More DifferentialsLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer