Summary
Definition
History and exam
Key diagnostic factors
- history of inflammatory bowel disease
- history of exposure to infectious agents
- history of recent antibiotic use
- history of HIV/AIDS/immunosuppressed state
- fevers/chills
- tachycardia
- mental status changes
- hypotension
- abdominal distention
Other diagnostic factors
- diarrhea
- abdominal pain
- abdominal tenderness
Risk factors
- ulcerative colitis (UC)
- Crohn colitis
- pseudomembranous colitis
- infectious colitis
- HIV/AIDS/immunosuppression
- discontinuation of medications for inflammatory bowel disease
- antimotility agents
- chemotherapy/chemical immunosuppression
- electrolyte abnormalities
Diagnostic tests
1st tests to order
- CBC
- serum electrolytes
- serum albumin levels
- serum lactic acid
- stool studies
- CT abdomen/pelvis
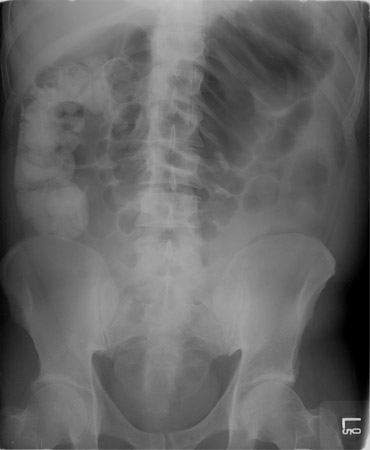
- abdominal x-ray
- chest x-ray
Tests to consider
- CRP
- erythrocyte sedimentation rate (ESR)
- blood cultures
- sigmoidoscopy
- rectal biopsy
- surgical specimen
Treatment algorithm
all patients
Contributors
Authors
Jan Rakinic, MD
Chief
Colorectal Surgery
Department of Surgery
Southern Illinois University School of Medicine
Springfield
IL
Disclosures
JR is the President of the American Board of Colon and Rectal Surgery.
V. Prasad Poola, MBBS, FACS, FASCRS
Associate Professor of Surgery
Department of Surgery
Southern Illinois University School of Medicine
Springfield
IL
Disclosures
VPP declares that he has no competing interests.
Acknowledgements
Dr Jan Rakinic and Dr V. Prasad Poola would like to gratefully acknowledge Dr Scott A. Strong, Dr Mukta V. Krane, and Dr Alessandro Fichera, previous contributors to this topic.
Disclosures
SAS, MVK, and AF declare that they have no competing interests.
Peer reviewers
Sharon Stein, MD
Assistant Professor of Surgery
Division of Colon and Rectal Surgery
University Hospital Case Medical Center
Cleveland
OH
Disclosures
SS received a fee for educational courses on laparoscopic surgery, paid for in part by Covidien, Olympus, and Applied Medical.
David J. Hackam, MD, PhD
Associate Professor of Pediatric Surgery
University of Pittsburgh School of Medicine
Pittsburgh
PA
Disclosures
DJH declares that he has no competing interests.
James Wheeler, MB, BCh, MD, FRCS
Consultant
Colorectal Surgeon
Addenbrookes Hospital
Cambridge
UK
Disclosures
JW declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Rubin DT, Ananthakrishnan AN, Siegel CA, et al. ACG clinical guideline: ulcerative colitis in adults. Am J Gastroenterol. 2019 Mar;114(3):384-413.Full text Abstract
McDonald LC, Gerding DN, Johnson S, et al. Clinical practice guidelines for Clostridium difficile infection in adults and children: 2017 update by the Infectious Diseases Society of America (IDSA) and Society for Healthcare Epidemiology of America (SHEA). Clin Infect Dis. 2018 Mar 19;66(7):987-94.Full text Abstract
Kelly CR, Fischer M, Allegretti JR, et al. ACG clinical guidelines: prevention, diagnosis, and treatment of Clostridioides difficile infections. Am J Gastroenterol. 2021 Jun 1;116(6):1124-47.Full text Abstract
Lightner AL, Vogel JD, Carmichael JC, et al. The American Society of Colon and Rectal Surgeons clinical practice guidelines for the surgical management of Crohn's disease. Dis Colon Rectum. 2020 Aug;63(8):1028-52.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Colonic pseudo-obstruction
- Acute mesenteric ischemia
- Large bowel obstruction
More DifferentialsGuidelines
- WSES-AAST guidelines: management of inflammatory bowel disease in the emergency setting
- Update on the treatment guidance document for Clostridium difficile infection
More GuidelinesVideos
Nasogastric tube insertion animated demonstration
More videosLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer