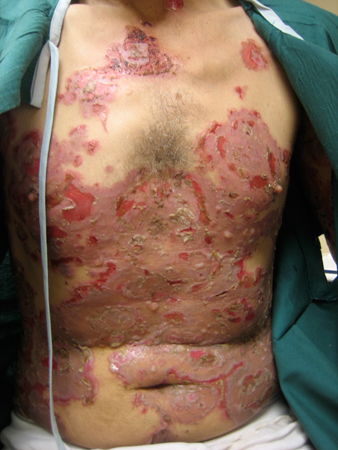
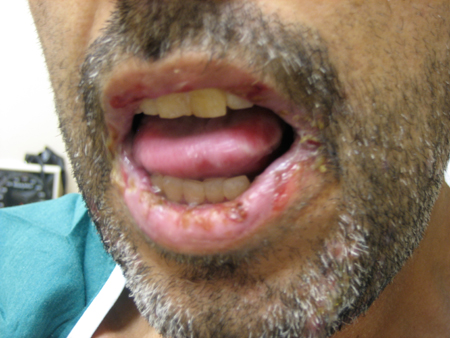
Summary
Differentials
Common
- Herpes simplex
- Herpes zoster (shingles)
- Varicella zoster, acute (chickenpox)
- Dermatophyte infections (inflammatory or bullous tinea pedis)
- Scabies
- Impetigo
- Friction blister
- Miliaria
- Eczematous dermatitis (allergic contact, nummular, and dyshidrotic)
- Thermal burn
- Frostbite
Uncommon
- Staphylococcal scalded skin syndrome
- Epidermolysis bullosa
- Coma bullae
- Nutritional deficiencies (zinc, biotin, niacin, essential fatty acids)
- Porphyria cutanea tarda
- Pseudoporphyria cutanea tarda
- Diabetic bullae (bullosis diabeticorum)
- Incontinentia pigmenti
- Bullous ichthyosiform erythroderma (epidermolytic hyperkeratosis)
- Mastocytosis
- Bullous arthropod bite reaction
- Erythema multiforme
- Stevens-Johnson syndrome
- Toxic epidermal necrolysis
- Amyloidosis
- Hand-foot-mouth disease
- Congenital syphilis
- Linear IgA disease
- Chronic bullous disease of childhood
- Pemphigus vulgaris
- Pemphigus foliaceus (fogo selvagem, pemphigus erythematosus)
- Paraneoplastic pemphigus
- Bullous pemphigoid
- Pemphigoid gestationis
- Mucous membrane pemphigoid (cicatricial pemphigoid)
- Epidermolysis bullosa acquisita
- Bullous lupus erythematosus
- Dermatitis herpetiformis
- Mpox
Contributors
Authors
Jon H. Meyerle, MD
Associate Professor
Department of Dermatology
Uniformed Services University of the Health Sciences
Bethesda
MD
Disclosures
JHM declares that he has no competing interests.
Acknowledgements
Dr Jon H. Meyerle would like to gratefully acknowledge Dr Keira L. Barr, a previous contributor to this topic.
Disclosures
KLB declares that she has no competing interests.
Peer reviewers
Hywel C. Williams, MSc, PhD, FRCP
Professor of Dermato-Epidemiology
Center of Evidence Based Dermatology
Nottingham University Hospitals
NHS Trust
Queen's Medical Centre
Nottingham
UK
Disclosures
HCW declares that he has no competing interests.
Dedee F. Murrell, MA, BMBCh, FAAD, MD
Head of Department
Department of Dermatology
St George Hospital
Conjoint Professor
University of New South Wales
Sydney
Australia
Disclosures
DFM declares that she has no competing interests.
Vesna Petronic-Rosic, MD, MSc
Associate Professor and Clinical Director
Section of Dermatology
University of Chicago
Chicago
IL
Disclosures
VPR declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Berger TG, James WD, Elston DM. Andrew's diseases of the skin, clinical dermatology, 10th edition. WB Saunders; 2008.
Joly P, Horvath B, Patsatsi Α, et al. Updated S2K guidelines on the management of pemphigus vulgaris and foliaceus initiated by the european academy of dermatology and venereology (EADV). J Eur Acad Dermatol Venereol. 2020 Sep;34(9):1900-13.Full text Abstract
Fine JD, Bruckner-Tuderman L, Eady RA, et al. Inherited epidermolysis bullosa: updated recommendations on diagnosis and classification. J Am Acad Dermatol. 2014 Jun;70(6):1103-26.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
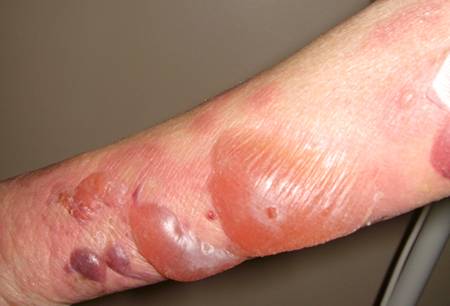
Patient information
Dermatitis (seborrheic) of the body
Eczema
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer