Summary
Definition
History and exam
Key diagnostic factors
- history of anorectal, neurologic, or spinal abnormalities, or gastrointestinal surgery
- fecal soiling or diarrhea
- constipation
- perianal skin irritation
- abnormal rectal examination
- spinal deformities
- weakness and decreased or absent reflexes
Other diagnostic factors
- behavior problems
- painful bowel movements
- abdominal pain/cramping
- posturing described as tightening of buttocks
- enuresis
- anorectal malformation
- abnormal abdominal examination
- history of underlying medical condition
Risk factors
- chronic constipation
- male sex
- age: 5 to 6 years
- diet lacking in fiber
- inadequate fluid intake
- delayed or inadequate toilet training
- anorectal malformations
- Hirschsprung disease
- spinal abnormalities
- psychological or behavioral problems due to stressful family events
- psychiatric disorders
- medication overuse
Diagnostic tests
1st tests to order
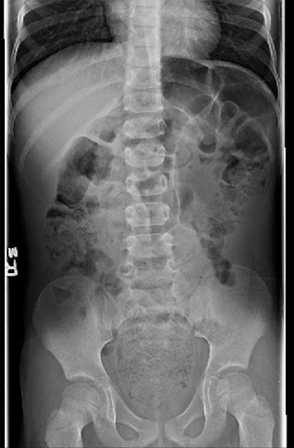
- abdominal x-ray
Tests to consider
- unprepared barium enema
- spinal x-ray
- MRI spine
- radiopaque marker transit radiograph
- colonic and rectal manometry studies
- rectal biopsy
- serum thyroid-stimulating hormone level
- serum free thyroxine (T4) level
- sweat chloride test
- tissue transglutaminase IgA
Treatment algorithm
with constipation and fecal impaction
without constipation
fecal impaction resolved
Contributors
Authors
Brian D. Riedel, MD
Clinical Associate Professor of Pediatrics Emeritus
Pediatric Gastroenterology, Hepatology and Nutrition
West Virginia University School of Medicine
Morgantown
WV
Disclosures
BDR declares that he has no competing interests.
Acknowledgements
Dr Brian D. Riedel would like to gratefully acknowledge Dr Linda S. Nield and Dr Uwe Blecker, previous contributors to this topic.
Disclosures
UB declares that he has no competing interests. LSN is an author of a reference cited in this topic.
Peer reviewers
John C. Thomas, MD
Assistant Professor
Division of Pediatric Urology
Monroe Carell Jr. Children's Hospital at Vanderbilt
Nashville
TN
Disclosures
JCT declares that he has no competing interests.
David C. A. Candy, MBBS, MSc, MD, FRCP, FRCPCH, FCU
Consultant Paediatrics Gastroenterologist
Western Sussex Hospitals NHS Trust
Chichester
Honorary Consultant Paediatric Gastroenterologist
Royal Alexandra Children's Hospital
Brighton and Sussex University Hospitals
Brighton
UK
Disclosures
DCAC has received research grants, consultancy fees, and reimbursement of conference expenses from Norgine UK, the manufacturer of Movicol. He is the author of a systematic review of polyethylene glycol-based laxatives; convenor of the Paris Consensus on Constipation Terminology Group; and external advisor of the National Institute for Health and Care Excellence pediatric constipation guideline development group.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Hyams JS, Di Lorenzo C, Saps M, et al. Functional disorders: children and adolescents. Gastroenterology. 2016 May;150(6):1456-68. Abstract
Levitt MA, Pena A. Anorectal malformations. Orphanet J Rare Dis. 2007 Jul 26;2:33.Full text Abstract
Bongers ME, Tabbers MM, Benninga MA. Functional nonretentive fecal incontinence in children. J Pediatr Gastroenterol Nutr. 2007 Jan;44(1):5-13.Full text Abstract
Abrams P, Andersson KE, Apostolidis A, et al. 6th International Consultation on Incontinence. Recommendations of the International Scientific Committee: evaluation and treatment of urinary incontinence, pelvic organ prolapse and faecal incontinence. Neurourol Urodyn. 2018 Sep;37(7):2271-2.Full text Abstract
Tabbers MM, DiLorenzo C, Berger MY, et al. Evaluation and treatment of functional constipation in infants and children: evidence-based recommendations from ESPGHAN and NASPGHAN. J Pediatr Gastroenterol Nutr. 2014 Feb;58(2):258-74.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Nonspecific toddler's diarrhea
- Irritable bowel syndrome (IBS) with alternating constipation and diarrhea
- Infectious diarrhea
More DifferentialsGuidelines
- Constipation
- Sixth International Consultation on Incontinence recommendations of the International Scientific Committee: evaluation and treatment of urinary incontinence, pelvic organ prolapse, and fecal incontinence
More GuidelinesPatient information
Constipation in children
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer