Summary
Definition
History and exam
Key diagnostic factors
- bowel sounds in chest
Other diagnostic factors
- heartburn
- regurgitation
- obesity
- chest pain
- dysphagia
- odynophagia
- hematemesis
- shortness of breath
- cough
- oropharyngitis
- wheezing
- nonbilious vomiting
- fever and chills
- confusion
Risk factors
- obesity
- increased age
- previous gastroesophageal procedure
- elevated intra-abdominal pressure
- male sex
- incisional, umbilical, or inguinal hernia
Diagnostic tests
1st tests to order
- chest x-ray
- upper gastrointestinal fluoroscopy with oral contrast
Tests to consider
- esophago-gastro-duodenoscopy
- CT scan or MRI scan
- high-resolution esophageal manometry and pH monitoring
Treatment algorithm
upper gastrointestinal hemorrhage and/or obstruction and/or volvulus
irreversible organ ischemia and/or necrosis
symptomatic gastroesophageal reflux disease (GERD)
type I refractory to medical therapy or patient prefers surgery
types II, III, and IV
Contributors
Authors
Constantine T. Frantzides, MD, PhD, FACS

Director
Chicago Institute of Minimally Invasive Surgery
St. Francis Hospital
Clinical Professor of Surgery
University of Illinois Chicago
Chicago
IL
Disclosures
CTF declares that he has no competing interests.
Acknowledgements
Dr Constantine T. Frantzides would like to gratefully acknowledge Dr Mark A. Carlson, Dr Amy J. Hargrove and Dr Minh B. Luu, previous contributors to this topic.
Disclosures
MAC, AJH and MBL declare they have no competing interests.
Peer reviewers
Frank A. Granderath, MD
Associate Professor
Department of General, Visceral and Transplant Surgery
University Hospital Tuebingen
Germany
Disclosures
FAG declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Society of American Gastrointestinal and Endoscopic Surgeons. Guidelines for the management of hiatal hernia. Apr 2013 [internet publication].Full text
Roman S, Kahrilas PJ. The diagnosis and management of hiatus hernia. BMJ. 2014 Oct 23;349:g6154. Abstract
Sfara A, Dumitrascu DL. The management of hiatal hernia: an update on diagnosis and treatment. Med Pharm Rep. 2019 Oct;92(4):321-25.Full text Abstract
Antoniou SA, Müller-Stich BP, Antoniou GA, et al. Laparoscopic augmentation of the diaphragmatic hiatus with biologic mesh versus suture repair: a systematic review and meta-analysis. Langenbecks Arch Surg. 2015 Jul;400(5):577-83. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
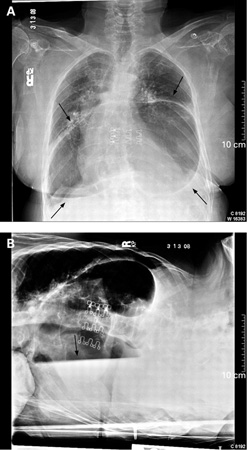
Differentials
- Angina pectoris
- Gastroesophageal reflux disease (GERD)
- Pneumonia
More DifferentialsGuidelines
- Guidelines for the surgical treatment of hiatal hernias
- ACR appropriateness criteria: epigastric pain
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer