Resumo
Definição
História e exame físico
Principais fatores diagnósticos
- family history of PDB
- asymptomatic
Outros fatores diagnósticos
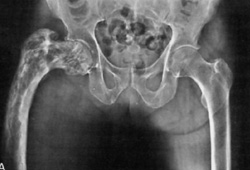
- femoral, pelvis, and/or skull involvement
- long-bone or back pain
- pathologic fracture
- bony deformities (e.g., frontal bossing, prognathism, bone bowing)
- increased local temperature
- hearing loss
- facial pain
- loosening teeth or disturbance in chewing
- isolated raised alkaline phosphatase
Fatores de risco
- family history of PDB
- age >50 years
- male sex (45- to 74-years age group)
Investigações diagnósticas
Primeiras investigações a serem solicitadas
- plain x-ray
- bone scan
- total serum alkaline phosphatase
- bone-specific alkaline phosphatase
- serum calcium
- serum procollagen 1 N-terminal peptide (P1NP)
- serum C-terminal propeptide of type 1 collagen (CTX)
- liver function tests
- serum 25-hydroxyvitamin D
Investigações a serem consideradas
- CT scan or MRI
- bone biopsy
Algoritmo de tratamento
asymptomatic patients, incidental diagnosis
symptomatic patients
Colaboradores
Autores
Roberto Civitelli, MD
Sydney M. & Stella H. Schoenberg Professor of Medicine
Professor of Orthopaedic Surgery and Cell Biology and Physiology
Chief, Division of Bone and Mineral Diseases
Musculoskeletal Research Center
Washington University School of Medicine
St. Louis
MO
Disclosures
RC is Editor-in-Chief of the Journal of Bone and Mineral Research (position ending 31/12/2022).
Mahshid Mohseni, MD, MSci
Assistant Professor
Director, Clinical Research Unit
Co-Director, Clinical Operations
Division of Bone and Mineral Diseases
Department of Medicine
Washington University School of Medicine
St. Louis
MO
Disclosures
MM declares that he has no competing interests.
Acknowledgements
Dr Roberto Civitelli and Dr Mahshid Mohseni would like to gratefully acknowledge Dr Julia F. Charles, Dr Camilo Restrepo, and Dr Javad Parvizi, previous contributors to this topic.
Disclosures
JFC has received royalties from Up To Date, Waltham, MA, for authorship on articles relating to PDB; received grant funding from the National Institues of Health, the Rheumatology Research Foundation, and Brigham and Women's Hospital for research into regulation of osteoclast function, but not specifically relating to PDB; and had a manuscript published from a collaboration with Dr Jae Shim describing a pagetic phenotype in mice with osteoclast-specific loss of Chmp5. CR and JP are authors of a reference cited in this topic.
Peer reviewers
Frederick Singer, MD
Director
Endocrine/Bone Disease Program
John Wayne Cancer Institute
Santa Monica
CA
Disclosures
FS declares that he has no competing interests.
Joseph Lane, MD
Orthopaedic Surgeon
Hospital for Special Surgery
New York
NY
Disclosures
JL declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Tuck SP, Walker J. Adult Paget's disease of bone. Clin Med (Lond). 2020 Nov;20(6):568-71.Full text Abstract
Singer FR, Bone HG 3rd, Hosking DJ, et al. Paget's disease of bone: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2014 Dec;99(12):4408-22.Full text Abstract
Whitehouse RW. Paget's disease of bone. Semin Musculoskelet Radiol. 2002 Dec;6(4):313-22. Abstract
Ralston SH, Corral-Gudino L, Cooper C, et al. Diagnosis and management of Paget's disease of bone in adults: a clinical guideline. J Bone Miner Res. 2019 Apr;34(4):579-604.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Osteomalacia
- Fibrous dysplasia
More DifferentialsGuidelines
- Diagnosis and management of Paget's disease of bone in adults
- Paget’s disease of bone
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer