Summary
Definition
History and exam
Key diagnostic factors
- inguinal lymphadenopathy
- nonspecific symptoms of proctocolitis
- groove sign of Greenblatt
- genital elephantiasis, saxophone penis, esthiomene
Other diagnostic factors
- fever, malaise, arthralgias
- lower abdominal or lower back pain
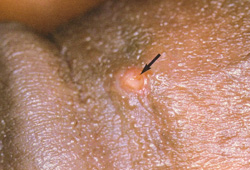
- genital or anal ulcer
- nonspecific symptoms of bacteremic spread
- erythema nodosum
- anogenital sinus tracts, strictures, or fistulae
Risk factors
- other STIs
- risky sexual behavior
- HIV-seropositivity
- age (20 to 40 years)
- unprotected intercourse in an area endemic for LGV
- male
Diagnostic tests
1st tests to order
- genital or lymph node specimens for nucleic acid amplification testing (NAAT)
- swab via anoscopy for Gram staining
- fluid or swab for LGV-specific molecular testing
- STI testing
Tests to consider
- endoscopy with histopathology
- serum for complement fixation
- serum for microimmunofluorescence (MIF)
- CT of abdomen and pelvis
- MRI of abdomen and pelvis
- fluid or swab for culture
Emerging tests
- fluid or swab for genovar typing
Treatment algorithm
asymptomatic adolescent and adult patients who have been exposed to lymphogranuloma venereum (LGV)
all stages of lymphogranuloma venereum (LGV)
Contributors
Authors
Benjamin D. Lorenz, MD
Assistant Professor
Division of Hospital Medicine
MedStar Georgetown University Hospital
Washington
DC
Disclosures
BDL declares that he has no competing interests.
Acknowledgements
Dr Benjamin D. Lorenz would like to gratefully acknowledge Dr Mettassebia Kanno, a previous contributor to this topic.
Disclosures
MK declares that she has no competing interests.
Peer reviewers
Cees van Nieuwkoop, MD
Department of General Internal Medicine
Leiden University Medical Centre
Leiden
The Netherlands
Disclosures
CvN declares that he has no competing interests.
David Chelmow, MD
Chair
Department of Obstetrics and Gynecology
Virginia Commonwealth University
Richmond
VA
Disclosures
DC declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
de Vries HJC, de Barbeyrac B, de Vrieze NHN, et al. 2019 European guideline on the management of lymphogranuloma venereum. J Eur Acad Dermatol Venereol. 2019 Jun 26;33(10):1821-8.Full text Abstract
Centers for Disease Control and Prevention. Lymphogranuloma venereum among men who have sex with men - Netherlands, 2003-2004. MMWR Morb Mortal Wkly Rep. 2004 Oct 29;53(42):985-8.Full text Abstract
Van der Bij AK, Spaargaren J, Morre SA, et al. Diagnostic and clinical implications of anorectal lymphogranuloma venereum in men who have sex with men: a retrospective case-control study. Clin Infect Dis. 2006 Jan 15;42(2):186-94.Full text Abstract
Stamm WE. Lymphogranuloma venereum. In: Holmes KK, Sparling PF, Stamm WE, et al., eds. Sexually transmitted diseases. 4th ed. New York, NY: McGraw Hill; 2007:595-606.
Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. MMWR Recomm Rep. 2021 Jul 23;70(4):1-187.Full text Abstract
Mabey D, Peeling RW. Lymphogranuloma venereum. Sex Transm Infect. 2002 Apr;78(2):90-2.Full text Abstract
Thorsteinsson SB. Lymphogranuloma venereum: review of clinical manifestations, epidemiology, diagnosis, and treatment. Scand J Infect Dis Suppl. 1982;32:127-31. Abstract
Annamuthodo H. Rectal lymphogranuloma venereum in Jamaica. Ann R Coll Surg Engl. 1961 Sep;29:141-59.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Syphilis (Treponema pallidum)
- Gonococcal proctitis
- Genital herpes (HSV)
More DifferentialsGuidelines
- BASHH summary guidance on testing for sexually transmitted infections, 2023
- Sexually transmitted infections treatment guidelines, 2021
More GuidelinesPatient information
Chlamydia
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer