Summary
Definition
History and exam
Key diagnostic factors
- history of opioid use disorder and dependence
- miosis
- bradypnea
- altered mental status
- dramatic response to naloxone
Other diagnostic factors
- fresh needle marks
- drug paraphernalia nearby
- decreased gastrointestinal motility
- old track marks on arms and legs
- pulmonary rales
- frothy pink sputum
- seizures
- dysrhythmias
Risk factors
- history of prescribed opioids
- opioid use disorder and dependence
- recent abstinence in chronic users
- taking opioids by injection
Diagnostic tests
1st tests to order
- therapeutic trial of naloxone
- Electrocardiogram (ECG)
Tests to consider
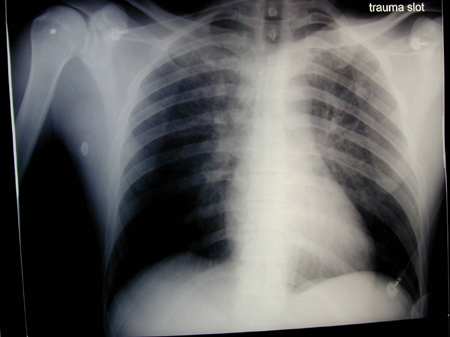
- chest x-ray
- abdominal CT scan
- abdominal x-ray
- opioid urine screen
- gas chromatography/ mass spectrometry
Treatment algorithm
without retained drug packages
with retained drug packages
Contributors
Authors
Ruben Thanacoody, MD, FRCP, FRCP(Edin), FEAPCCT
Consultant Physician and Clinical Toxicologist
Director, National Poisons Information Service (Newcastle)
Honorary Clinical Senior Lecturer, Newcastle University
Newcastle-upon-Tyne
UK
Disclosures
RT declares that he has contributed to the Royal College of Emergency Medicine best practice guidelines on management of opioid toxicity in emergency departments and delivered a lecture at the RCEM Annual Conference in Gateshead. He has not received any payment for this work.
Acknowledgements
Dr Ruben Thanacoody would like to gratefully acknowledge Dr Dean Olsen, a previous contributor to this topic.
Disclosures
DO declares that he has no competing interests.
Peer reviewers
Joseph Donroe, null
Associate Professor of Medicine
Yale School of Medicine
New Haven
CO
Disclosures
JD declares that he has no competing interests.
Anne-Maree Kelley, MD, MClinEd, FACEM
Director
Joseph Epstein Centre for Emergency Medicine Research
Western Health Sunshine Hospital
St Albans
Australia
Disclosures
AMK has received grant funding for research into intranasal delivery of naloxone in heroin overdose.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Dowell D, Ragan KR, Jones CM, et al. CDC clinical practice guideline for prescribing opioids for pain - United States, 2022. MMWR Recomm Rep. 2022 Nov 4;71(3):1-95.Full text Abstract
Dezfulian C, Orkin AM, Maron BA, et al. Opioid-associated out-of-hospital cardiac arrest: distinctive clinical features and implications for health care and public responses: a scientific statement from the American Heart Association. Circulation. 2021 Apr 20;143(16):e836-70.Full text Abstract
Resuscitation Council UK. 2021 resuscitation guidelines. 2021 [internet publication].Full text
Williams K, Lang ES, Panchal AR, et al. Evidence-based guidelines for EMS administration of naloxone. Prehosp Emerg Care. 2019 Nov-Dec;23(6):749-63.Full text Abstract
Lavonas EJ, Akpunonu PD, Arens AM, et al. 2023 American Heart Association focused update on the management of patients with cardiac arrest or life-threatening toxicity due to poisoning: an update to the American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2023 Oct 17;148(16):e149-84.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Gammahydroxybutyrate (GHB)/gammabutyrolactone (GBL) overdose
- Clonidine/imidazolines overdose
- Antipsychotic overdose
More DifferentialsGuidelines
- Joint RCEM and NPIS best practice guideline: assessment and management of acute opioid toxicity in adults in the emergency department
- 2023 American Heart Association focused update on the management of patients with cardiac arrest or life-threatening toxicity due to poisoning: an update to the American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer