Summary
Definition
History and exam
Key diagnostic factors
- midsystolic click
- late-systolic murmur
Other diagnostic factors
- palpitations
Risk factors
- family history
- slim body type
- connective tissue disorders
- mitral annular disjunction (MAD)
Diagnostic tests
1st tests to order
- echocardiogram
Tests to consider
- Holter or event monitor
- cardiac MRI
Treatment algorithm
asymptomatic
symptomatic
Contributors
Authors
Sheila Klassen, MD
Assistant Professor of Medicine
Harvard Medical School
Associate Director of Cardiovascular Integration
Center for Integration Science
Brigham and Women's Hospital
Boston
MA
Disclosures
SK declares that he has no competing interests.
Acknowledgements
Dr Sheila Klassen would like to gratefully acknowledge Dr Brian Griffin, Dr Shaberio Lo Presti, Dr Carmel Halley, and Dr Serge Harb, previous contributors to this topic.
Disclosures
BG, SLP, CH, and SH declared that they had no competing interests.
Peer reviewers
John Dent, MD
Associate Professor of Internal Medicine
Director of Stress Testing Laboratory and Echocardiography
University of Virginia Health System
Cardiovascular Fellowship Program
Charlottesville
VA
Disclosures
JD declares that he has no competing interests.
Prakash Punjabi, MBBS
Honorary Clinical Senior Lecturer
National Heart and Lung Institute
Imperial College London
London
UK
Disclosures
PP declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Otto CM, Nishimura RA, Bonow RO, et al. 2020 ACC/AHA guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2021 Feb 2;143(5):e72-e227.Full text Abstract
Delgado V, Ajmone Marsan N, de Waha S, et al. 2023 ESC guidelines for the management of endocarditis. Eur Heart J. 2023 Oct 14;44(39):3948-4042.Full text
Vahanian A, Beyersdorf F, Praz F, et al. 2021 ESC/EACTS guidelines for the management of valvular heart disease. Eur Heart J. 2021 Aug 28:ehab395.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
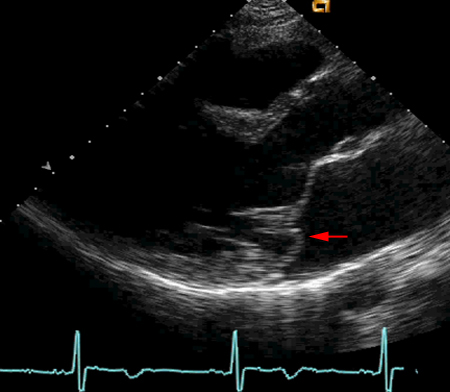
Differentials
- Aortic valve disease
- Pulmonic valve disease
- Atrial myxoma
More DifferentialsGuidelines
- 2023 ESC guidelines for the management of endocarditis
- 2021 ESC/EACTS guidelines for the management of valvular heart disease
More GuidelinesPatient information
Mitral valve prolapse
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer