Summary
Definition
History and exam
Key diagnostic factors
- abdominal pain
- constipation/failure to pass flatus or stool
- vomiting
- abdominal distention
- abdominal tenderness
- peritonitis
- presence of risk factors
- palpable abdominal mass
Other diagnostic factors
- nausea
- fever
- tachycardia
- tachypnea
- severe lethargy
- hypotension
- diarrhea
- groin swelling
Risk factors
- previous abdominal surgery
- intestinal malignancy
- malrotation
- Crohn disease
- hernia
- intussusception
- volvulus
- intestinal atresia
- appendicitis
- foreign body ingestion
Diagnostic tests
1st tests to order
- abdominal CT scan
- CBC
- BUN
- electrolyte panel
Tests to consider
- abdominal x-rays
- water-soluble contrast study
- laparotomy/laparoscopy
- abdominal ultrasound
- abdominal MRI
Treatment algorithm
complicated or strangulated SBO: surgical candidate
complicated or strangulated SBO: surgery not indicated
simple SBO
Contributors
Expert advisers
Adrian Maung, MD, MBA, FACS, FCCM
Associate Professor of Surgery
Division of General Surgery, Trauma and Surgical Critical Care
Department of Surgery
Yale School of Medicine
New Haven, CT
Disclosures
AM declares that he has no competing interests.
Acknowledgements
Dr Adrian Maung would like to gratefully acknowledge Dr John T. Jenkins, Dr Edward T. Pring, Dr George Malietzis, Dr Frances J. McNicol, and Dr David J. Hackam, previous contributors to this topic.
Disclosures
JTJ , ETP, GM, FJM, and DJH declare that they have no competing interests.
Peer reviewers
Steven D. Wexner, MD, FACS, FRCS, FRCS (Ed)
Chief Academic Officer
Emeritus Chief of Staff (1997-2007)
Chairman Department of Colorectal Surgery
Professor of Surgery Ohio State University
Affiliate Professor Department of Surgery
Division of General Surgery
University of South Florida College of Medicine
Cleveland Clinic Florida, FL
Disclosures
SDW declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Maung AA, Johnson DC, Piper GL, et al; Eastern Association for the Surgery of Trauma. Evaluation and management of small-bowel obstruction: an Eastern Association for the Surgery of Trauma practice management guideline. J Trauma Acute Care Surg. 2012 Nov;73(5 suppl 4):S362-9.Full text Abstract
Jackson P, Vigiola Cruz M. Intestinal obstruction: evaluation and management. Am Fam Physician. 2018 Sep 15;98(6):362-7. Abstract
American College of Radiology. ACR appropriateness criteria: suspected small-bowel obstruction. 2019 [internet publication].Full text
Ten Broek RPG, Krielen P, Di Saverio S, et al. Bologna guidelines for diagnosis and management of adhesive small bowel obstruction (ASBO): 2017 update of the evidence-based guidelines from the World Society of Emergency Surgery ASBO Working Group. World J Emerg Surg. 2018 Jun 19;13:24.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
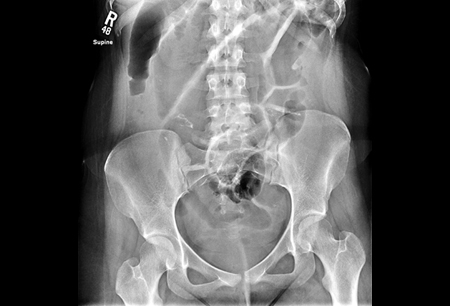
Differentials
- Ileus
- Infectious gastroenteritis
- Large bowel obstruction
More DifferentialsGuidelines
- ACR-SPR practice parameter for the performance of a contrast small bowel examination
- ACR appropriateness criteria: suspected small-bowel obstruction
More GuidelinesVideos
Venepuncture and phlebotomy: animated demonstration
Central venous catheter insertion: animated demonstration
More videosPatient information
Small bowel obstruction
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer