Summary
Definition
History and exam
Key diagnostic factors
- recent history of immersion in spa water
- new medication commenced known to be associated with folliculitis
Other diagnostic factors
- recent history of shaving
- umbilicated, flesh-colored papules
- papules on one side of the face in the submaxillary area
- small, uniform papules and pustules
- background erythema
- alopecia/scalp scaling
- erythematous plaques with hemorrhagic crusts in a dermatomal distribution
Risk factors
- trauma, including shaving and extraction
- topical corticosteroid preparations
- diabetes mellitus
- immunosuppression
- occlusion and perspiration
- systemic antibiotics
- immersion in under-chlorinated water
- drugs
Diagnostic tests
Tests to consider
- bacterial skin swab
- viral skin swab
- skin scraping for mycology
- tissue culture
- skin biopsy
Treatment algorithm
uncomplicated superficial folliculitis, organism unknown
recurrent/deep folliculitis due to methicillin-susceptible Staphylococcus aureus (MSSA)
recurrent/deep folliculitis due to methicillin-resistant Staphylococcus aureus (MRSA)
gram-negative folliculitis
hot tub folliculitis due to Pseudomonas aeruginosa infection
dermatophytic folliculitis
Malassezia furfur (Pityrosporum folliculitis)
Candida folliculitis
HSV folliculitis
Demodex folliculorum folliculitis
drug-induced folliculitis
eosinophilic pustular folliculitis (Ofuji disease)
HIV-associated eosinophilic folliculitis
eosinophilic pustular folliculitis in infancy
Contributors
Authors
Joshua Hekmatjah, BS
Clinical Research Fellow
Dermatology Department
Keck School of Medicine of USC
University of Southern California
Los Angeles
CA
Disclosures
JH declares that he has no competing interests.
Nazanin Ehsani-Chimeh, MD
Clinical Research Fellow
Dermatology Department
Keck School of Medicine of USC
University of Southern California
Los Angeles
CA
Disclosures
NEC declares that she has no competing interests.
April W. Armstrong, MD, MPH

Associate Dean, Clinical Research
Associate Professor of Dermatology
Keck School of Medicine of USC
University of Southern California
Los Angeles
CA
Disclosures
AWA has served as an investigator for Abbvie, Bristol-Myers-Squibb, Dermavent, Janssen, Eli Lilly, Modernizing Medicine, Novartis, OrthoDermalogics, Pfizer, Regeneron Pharmaceuticals, Sanofi Genzyme, and Sun Pharma; has been a speaker for Abbvie, Regeneron, and Sanofi Genzyme; and is a member of the data safety monitoring board for Boehringer Ingelheim/Paraxel. Her institution has received funding from Bristol-Myers-Squibb, Dermavent, Dermira, Eli Lilly, Galderma, Janssen-Ortho, Kyowa Hakko Kirin, Leo Pharma, Pfizer, and UCB Pharma.
Acknowledgements
Joshua Hekmatjah, Dr Nazanin Ehsani-Chimeh, and Dr April W. Armstrong would like to gratefully acknowledge Professor Howard Baden, a previous contributor to this topic.
Disclosures
HB declares that he has no competing interests.
Peer reviewers
Lowell Goldsmith, MD
Professor of Dermatology
Dean Emeritus
School of Medicine and Dentistry
University of North Carolina
Chapel Hill
NC
Disclosures
LG is editor-in-chief and co-founder of Logicalimages, Inc, which has print and electronic products for education and point-of-care; he has stock and stock options in that corporation. He is on the clinical and scientific advisory boards of Anacor Inc, which is developing anti-inflammatory and anti-infective products that are in early clinical trials; he receives payments and stock options for those services.
Dedee F. Murrell, MA, BMBCh, FAAD, MD
Head of Department
Department of Dermatology
St George Hospital
Conjoint Professor
University of New South Wales
Sydney
Australia
Disclosures
DFM declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Lucky AW, Esterly NB, Heskel N, et al. Eosinophilic pustular folliculitis in infancy. Pediatric Dermatol. 1984 Jan;1(3):202-6. Abstract
Buckley DA, Munn SE, Higgins EM. Neonatal eosinophilic pustular folliculitis. Clinical Exp Dermatol. 2001 May;26(3):251-5. Abstract
Faergemann J. Pityrosporum infections. J Am Acad Dermatol. 1994 Sep;31(3 Pt 2):S18-20. Abstract
Ota T, Hata A, Tanikawa A, et al. Eosinophilic pustular folliculitis (Ofuji's disease): indomethacin as a first choice of treatment. Clin Exp Dermatol. 2001 Mar;26(2):179-81. Abstract
Oranje AP, Folkers E. The Tzanck smear: old, but still of inestimable value. Pediatr Dermatol. 1988 May;5(2):127-9. Abstract
Ranki A, Hyry H, Klimenko T, et al. Update on current care guidelines. Bacterial skin infections [in Finnish]. Duodecim. 2010;126(24):2883-4. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
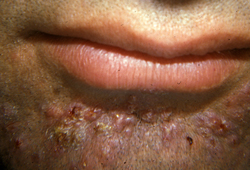
Differentials
- Pseudofolliculitis barbae
- Acne vulgaris
- Acne rosacea
More DifferentialsLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer