Summary
Definition
History and exam
Key diagnostic factors
- maladaptive pattern of opioid use
- high Addiction Severity Index (ASI) score
- blunting of pleasurable opioid effects
- miosis
- dilated pupils
- shallow/slow respirations or apnea
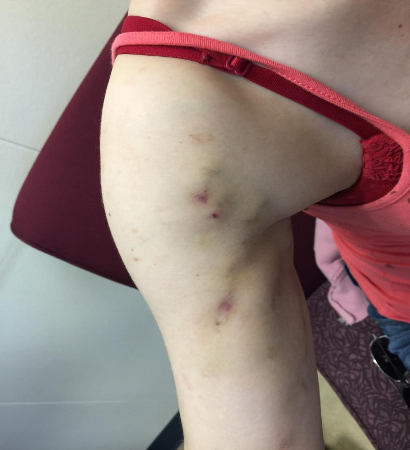
- needle marks, scars, or necrosis on skin near veins
- unconsciousness
- pulse <40 bpm
Other diagnostic factors
- chronic constipation
- weight loss
- nausea/vomiting
- sedation
- restless sleep/insomnia
- memory impairment
- sneezing
- yawning
- abdominal cramps
- diarrhea
- backache/muscle spasms
- hot and cold flashes
- hypotension
- sedation
- confusion
- slurred speech
- aggressive behavior
- excess perspiration or lacrimation
- rhinorrhea
- restlessness
- piloerection
- tachypnea
- hypertension
- arrhythmias
- seizures
Risk factors
- young age
- history of a mental health disorder
- history of substance use
- long-term opioid therapy
- childhood trauma
- homelessness/housing instability
- family history of substance use
- criminal justice system involvement
Diagnostic tests
1st tests to order
- Addiction Severity Index (ASI)
- clinical opiate withdrawal scale (COWS)
- urine or saliva drug screen
- gas chromatography-mass spectroscopy (GC-MS)
- serum electrolytes
- CBC
- BUN/creatinine
- LFTs
- hepatitis serology
- HIV serology
- purified protein derivative (PPD) skin test
Tests to consider
- rapid plasma reagin
- blood cultures
- beta human chorionic gonadotropin (beta-hCG)
Treatment algorithm
nonpregnant adults in inpatient/outpatient medically supervised withdrawal program
nonpregnant adolescents in inpatient/outpatient medically supervised withdrawal program
pregnant women in inpatient/outpatient medically supervised withdrawal program
nonpregnant adults after medically supervised withdrawal or suitable for initial or early maintenance therapy
nonpregnant adolescents after medically supervised withdrawal or suitable for initial or early maintenance therapy
pregnant women after medically supervised withdrawal or suitable for initial or early maintenance therapy
Contributors
Authors
Ashwin A. Patkar, MD, MRCPsych
Associate Professor
Medical Director
Duke Addictions Program
Department of Psychiatry and Behavioral Sciences
Duke University Medical Center
Durham
NC
Disclosures
AAP is a stockholder in Generys Biopharmaceuticals that has compounds in development for drug addiction (for stimulant use disorder). AAP provides expert testimony for United States Federal Agencies and is an expert reviewer for North Carolina Medical Board. AAP is the author of references cited in this topic.
Jonathan C. Lee, MD
Medical Director
The Farley Center at Williamsburg Place
Williamsburg
Community Assistant Professor
Department of Family Medicine
Eastern Virginia Medical School
Norfolk
Assistant Clinical Professor
Department of Psychiatry
Virginia Commonwealth University
Richmond
VA
Affiliate Assistant Professor
Department of Psychiatric Medicine
East Carolina University
Greenville
NC
Disclosures
JCL declares that he has no competing interests.
Isabel Patton, B.S, B.A
Medical Assistant
Department of Psychology
Emory University
Atlanta
Georgia
Disclosures
IP declares being an employee of AAP who has declared interests above. IP has co-authored a manuscript with AAP which has not yet been published.
Acknowledgements
Dr Ashwin A. Patkar, Dr Jonathan C. Lee, and Isabel Patton would like to gratefully acknowledge Dr Douglas M. Burgess, Dr Kamal Bhatia and Dr Srilakshmi Musham, previous contributors to this topic.
Disclosures
DMB declares that he has no competing interests. KB declares that he has received grant support from National Institutes of Health, Lundbeck, Pfizer, and Titan Pharmaceuticals. SM declares that she has received grant support from Pfizer, Titan Pharmaceuticals, Shire, and the Forest Research Institute.
Peer reviewers
Christos Kouimtsidis, MBBS, MSc, MRCPsych, PhD
Consultant Psychiatrist and Honorary Senior Lecturer
Institute of Psychiatry
King's College London
London
UK
Disclosures
CK declares that he has no competing interests.
George E. Woody, MD
Emeritus Professor
Department of Psychiatry
Perelman School of Medicine
University of Pennsylvania
Philadelphia
PA
Disclosures
GEW declares that he has no competing interests. GEW is an author of a number of references cited in this topic.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
American Psychiatric Association. Diagnostic and statistical manual of mental disorders, 5th ed, text revision (DSM-5-TR). Washington, DC: American Psychiatric Association; 2022.Full text
World Health Organization. WHO releases 2025 update to the International Classification of Diseases (ICD-11). Feb 2025 [Internet publication].Full text
American Society of Addiction Medicine. The ASAM national practice guideline for the treatment of opioid use disorder: 2020 focused update. 2020 Mar/Apr;14(2S suppl 1):1-91.Full text Abstract
Substance Abuse and Mental Health Services Administration. TIP 63: medications for opioid use disorder. Jul 2021 [internet publication].Full text
National Institute for Health and Care Excellence. Drug misuse in over 16s: opioid detoxification. Jul 2007 (reaffirmed 2019) [internet publication].Full text
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Alcohol intoxication
- Sedative intoxication
- Anticholinergic intoxication
More DifferentialsGuidelines
- Management of opioid use disorder: 2024 update to the national clinical practice guideline
- Comprehensive, evidence-based, consensus guidelines for prescription of opioids for chronic non-cancer pain
More GuidelinesPatient information
Opioid-use disorder
More Patient informationCalculators
Clinical Opioid Withdrawal Scale (COWS) for adults and adolescents
More CalculatorsLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer