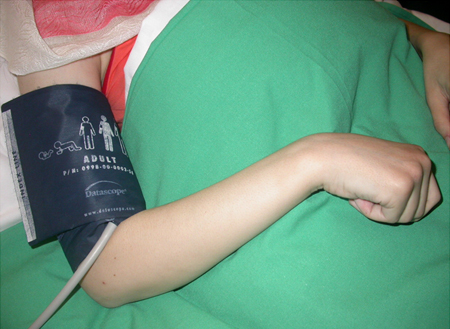
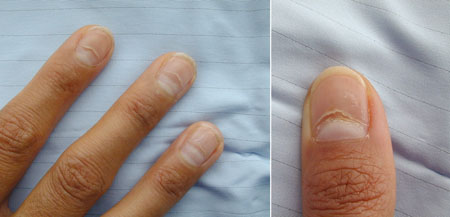
Summary
Differentials
Common
- Iatrogenic postsurgical hypoparathyroidism
- Vitamin D deficiency
- Hypomagnesemia
- Hyperventilation
Uncommon
- Isolated hypoparathyroidism
- Pseudohypoparathyroidism
- Autoimmune hypoparathyroidism
- HIV-related hypoparathyroidism
- Hypermagnesemia
- Hyperphosphatemia
- Hypercalciuria
- Sepsis
- Burns
- Renal failure
- Acute pancreatitis
- Extensive osteoblastic skeletal metastasis
- Hungry bone syndrome
- Drug-induced hypocalcemia
- Multiple transfusions
- Hypoalbuminemia
- Drug interference with assay
- Infiltrative hypoparathyroidism
- DiGeorge syndrome and other developmental complexes
- Rhabdomyolysis
- Tumor lysis syndrome
- Constitutively activating calcium sensing receptor (CaSR) abnormalities (mutations or autoimmune activation)
- Vitamin D resistance or receptor mutations
Contributors
Authors
John Ayuk, MD, FRCP
Consultant Endocrinologist/Service Lead for Endocrinology
Department of Endocrinology
Queen Elizabeth Medical Centre
Queen Elizabeth Hospital
Birmingham
UK
Disclosures
JA declares that he has no competing interests.
Neil Gittoes, BSc, MB ChB, PhD, FRCP
Consultant Endocrinologist and Honorary Professor of Endocrinology
Department of Endocrinology
Centre for Endocrinology, Diabetes and Metabolism
Queen Elizabeth Medical Centre
Queen Elizabeth Hospital
Birmingham
UK
Disclosures
NG has received consultancy fees from Takeda and Ascendis for work on hypoparathyroidism. NG is an author of references cited in this topic.
Acknowledgements
Dr John Ayuk and Prof Neil Gittoes would like to gratefully acknowledge Dr Berhane Seyoum, a previous contributor to this topic.
Disclosures
BS declares that he has no competing interests.
Peer reviewers
Shehzad Basaria, MD
Assistant Professor
Johns Hopkins University School of Medicine
Baltimore
MD
Disclosures
SB declares that he has no competing interests.
Lawrence Kirschner, MD, PhD
Associate Professor of Medicine
The Ohio State University
Columbus
OH
Disclosures
LK declares that he has no competing interests.
Richard Quinton, MD
Consultant and Senior Lecturer
Endocrine Unit
Newcastle University and Royal Victoria Infirmary
Newcastle-upon-Tyne
UK
Disclosures
RQ has been reimbursed by Amgen, the manufacturer of cinacalcet, for attending a conference and for giving an educational seminar (total under £1,200 over past 3 years).
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Cooper MS, Gittoes NJ. Diagnosis and management of hypocalcaemia. BMJ. 2008 Jun 7;336(7656):1298-302.Full text Abstract
Turner J, Gittoes N, Selby P, et al. Society for endocrinology endocrine emergency guidance: emergency management of acute hypocalcaemia in adult patients. Endocr Connect. 2016 Sep;5(5):G7-8.Full text Abstract
Hannan FM, Thakker RV. Investigating hypocalcaemia. BMJ. 2013 May 9;346:f2213.
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Use of this content is subject to our disclaimer