Summary
Definition
History and exam
Key diagnostic factors
- female of reproductive age
- irregular menstruation
- infertility
- hirsutism
Other diagnostic factors
- acne
- overweight or obesity
- hypertension
- scalp hair loss
- oily skin or excessive sweating
- acanthosis nigricans
Risk factors
- family history of PCOS
- premature adrenarche
- obesity
- low birth weight
- fetal androgen exposure
- environmental endocrine disruptors
Diagnostic tests
1st tests to order
- serum 17-hydroxyprogesterone
- serum prolactin
- serum thyroid-stimulating hormone
- oral glucose tolerance test
- fasting lipid panel
Tests to consider
- serum total and free testosterone
- serum dehydroepiandrosterone sulfate (DHEAS)
- serum androstenedione
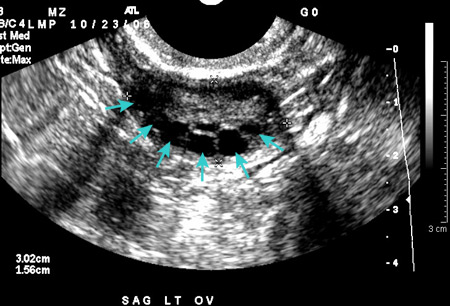
- pelvic ultrasound
- serum anti-Mullerian hormone
- basal body temperature monitoring
- luteal phase progesterone measurement
- serum LH and follicle-stimulating hormone (FSH)
- hemoglobin A1c or fasting plasma glucose
Treatment algorithm
with infertility and desiring fertility
not desiring current fertility
Contributors
Authors
Mark O. Goodarzi, MD, PhD

Division of Endocrinology, Diabetes & Metabolism
Eris M. Field Chair in Diabetes Research
Professor of Medicine
Cedars-Sinai Medical Center
Los Angeles
CA
Disclosures
MOG has been reimbursed for one-time participation in an advisory board for Nestle Health Science on the topic of exocrine pancreatic dysfunction. MOG is an author of a number of references cited in this topic.
Peer reviewers
Antoni Duleba, MD
Professor
Department of Obstetrics and Gynecology
University of California Davis
Sacramento
CA
Disclosures
AD declares that he has no competing interests.
Richard S. Legro, MD
Professor
Department of Obstetrics and Gynecology
Penn State Hershey College of Medicine
Hershey
PA
Disclosures
RSL has been reimbursed by Serono for attending a medical conference and received a lecture fee, and has consulted for Ferring. He has received research funding from the NIH, the Commonwealth of Pennsylvania, and Parke Davis. He is an author of a number of references cited in this topic.
Cornelis B. (Nils) Lambalk, MD, PhD
Gynaecologist/Fertility Specialist
Division of Reproductive Medicine
Department of Obstetrics and Gynaecology
VU University Medical Centre
Amsterdam
The Netherlands
Disclosures
CBL declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Azziz R, Carmina E, Chen Z, et al. Polycystic ovary syndrome. Nat Rev Dis Primers. 2016 Aug 11;2:16057. Abstract
Teede HJ, Tay CT, Laven JJE, et al. Recommendations from the 2023 international evidence-based guideline for the assessment and management of polycystic ovary syndrome. J Clin Endocrinol Metab. 2023 Sep 18;108(10):2447-69.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- 21-hydroxylase deficiency
- Thyroid dysfunction
- Hyperprolactinemia
More DifferentialsGuidelines
- International evidence-based guideline for the assessment and management of polycystic ovary syndrome
- ACOG practice bulletin: polycystic ovary syndrome
More GuidelinesPatient information
Polycystic ovary syndrome: what is it?
Polycystic ovary syndrome: what are the treatment options?
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer