Summary
Definition
History and exam
Key diagnostic factors
- history of diabetes mellitus
- presence of risk factors
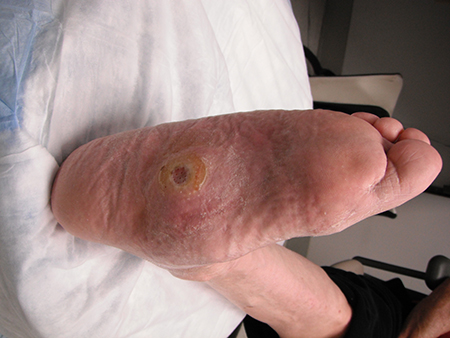
- foot ulcer
- foot pain
- loss of protective sensation
- foot deformity
- fever or chills
Other diagnostic factors
- malaise
- anorexia
- foot erythema
- edema of foot, ankle, or calf
- absent pedal pulses
- fluctuance
Risk factors
- sensory neuropathy
- previous history of foot ulcer
- previous history of amputation
- peripheral artery disease (PAD)
- end-stage renal disease (ESRD)
- foot deformities
- limited foot and/or ankle joint mobility
- visual impairment
- poor glucose control
- Charcot’s neuro-osteoarthropathy
- obesity
- obstructive sleep apnea (OSA)
Diagnostic tests
1st tests to order
- clinical diagnosis
Tests to consider
- CBC
- blood glucose level
- CRP
- erythrocyte sedimentation rate
- renal function
- microbiologic culture
- x-ray foot
- ankle/toe pressures and brachial indices
- pedal doppler waveforms with pulse volume recordings (PVR)
- duplex ultrasound
- catheter digital subtraction angiography (DSA)
- CT angiography
- MR angiography
- MRI foot
- CT foot
- 18F-fluorodeoxyglucose (FDG)-PET/CT
- 99mTc-exametazime hexa methyl propylene amine oxime (HMPAO)-labeled white blood cell scintigraphy
- 99mTc-labeled ubiquicidin (UBI) SPECT/CT single photon emission computed tomography (SPECT/CT)
Emerging tests
- serum procalcitonin
Treatment algorithm
at initial presentation
after initial definitive treatment
Contributors
Authors
Neal R. Barshes, MD, MPH, FACS
Assistant Professor
Division of Vascular Surgery and Endovascular Therapy
Michael E. DeBakey Department of Surgery
Baylor College of Medicine
Houston
TX
Disclosures
NRB is an author of several articles cited in this topic.
Joseph L. Mills Sr, MD
Professor and Chief
Division of Vascular Surgery and Endovascular Therapy
Michael E. DeBakey Department of Surgery
Baylor College of Medicine
Houston
TX
Disclosures
JLM has been reimbursed for consulting for AnGes and is an author of several articles cited in this topic.
David G. Armstrong, DPM, MD, PhD
Professor of Surgery and Neurological Surgery
Director of Southwestern Academic Limb Salvage Alliance (SALSA)
Keck School of Medicine of University of Southern California (USC)
Los Angeles
CA
Disclosures
DGA is an author of several articles cited in this topic.
Peer reviewers
Professor Vinod Panchbhavi, MD, FACS
Chief, Division of Foot and Ankle Surgery
Director, Foot and Ankle Fellowship Program
Department of Orthopedic Surgery
The University of Texas
Galveston
TX
Disclosures
VP declares that he has no competing interests.
Robert Hinchliffe, MD, FRCS
Reader and Honorary Consultant Vascular Surgeon
St George's Vascular Institute
London
UK
Disclosures
RH declares that he has no competing interests.
Lee C. Rogers, DPM
Associate Professor of Orthopaedics
University of Texas Health Science Center at San Antonio
San Antonio
TX
Disclosures
LR declares that he has no competing interests.
Judith Spratt, DPM
Highly Specialist Podiatrist
Lancashire Care Foundation NHS Trust
Preston
UK
Disclosures
JS declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
American Diabetes Association. Standards of care in diabetes - 2025. Diabetes Care. 2025 Jan 1;48(Suppl 1):S1-343.Full text
Schaper NC, van Netten JJ, Apelqvist J, et al. Practical guidelines on the prevention and management of diabetes-related foot disease (IWGDF 2023 update). Diabetes Metab Res Rev. 2024 Mar;40(3):e3657.Full text Abstract
Mills JL Sr, Conte MS, Armstrong DG, et al; Society for Vascular Surgery Lower Extremity Guidelines Committee. The Society for Vascular Surgery lower extremity threatened limb classification system: risk stratification based on wound, ischemia, and foot infection (WIfI). J Vasc Surg. 2014 Jan;59(1):220-34.Full text Abstract
Senneville É, Albalawi Z, van Asten SA, et al. IWGDF/IDSA guidelines on the diagnosis and treatment of diabetes-related foot infections (IWGDF/IDSA 2023). Diabetes Metab Res Rev. 2023 Oct 1:e3687.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Venous leg ulcer
- Gout
- Acute Charcot neuro-osteoarthropathy
More DifferentialsGuidelines
- ACR appropriateness criteria: suspected osteomyelitis of the foot in patients with diabetes mellitus
- Nutrition interventions in adults with diabetic foot ulcers
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer