Summary
Differentials
Common
- Septic nongonococcal arthritis
- Gonococcal arthritis
- Rheumatoid arthritis
- Gout
- Pseudogout
- Psoriatic arthritis
Uncommon
- Indolent infections
- Parvoviral syndrome
- Lyme disease
- Juvenile idiopathic arthritis (oligo-articular type)
- Acute rheumatic fever (ARF)
- Sarcoidosis
- Undifferentiated spondyloarthropathy
- Systemic lupus erythematosus (SLE)
- Adult-onset Still disease (AOSD)
- Reactive arthritis
- Ankylosing spondylitis (AS)
- Osteoarthritis
- Trauma
- Nontraumatic hemarthrosis
- Hypertrophic osteoarthropathy
- Intra-articular metastatic cancer
- Synovial sarcoma
- Arbovirus infections (e.g., chikungunya)
- Inflammatory bowel disease (ulcerative colitis and Crohn disease)
- Celiac disease
- Whipple disease
- Bowel-associated dermatosis arthritis syndrome
- Synovitis, acne, pustulosis, hyperostosis, and osteitis (SAPHO) syndrome
- Drug-induced
- Remitting seronegative symmetrical synovitis with pitting edema (RS3PE) syndrome
- Ebola disease
- Diffuse tenosynovial giant cell tumor (formerly, diffuse pigmented villonodular synovitis)
- Localized tenosynovial giant cell tumor (formerly, localized pigmented villonodular synovitis)
- Synovial osteochondromatosis
- Amyloid arthropathy
- Fibroblastic rheumatism
- Multicentric reticulohistiocytosis (MRH)
Contributors
Authors
Soumya Chatterjee, MD, MS, FRCP(UK), FACP, FACR
Professor of Medicine
Cleveland Clinic Lerner College of Medicine of Case Western Reserve University
Rheumatology Fellowship Program Director
Staff, Department of Rheumatic and Immunologic Diseases
Orthopedic and Rheumatologic Institute
Cleveland Clinic
Cleveland
OH
Disclosures
SC declares that he has no competing interests.
Peer reviewers
Hill Gaston, MA, PhD, BM BCh, FRCP, FMedSci
Professor of Rheumatology
University of Cambridge
Clinical Director
West Anglia CLRN
Cambridge
UK
Disclosures
HG declares that he has no competing interests.
Elena Myasoedova, MD, PhD
Professor
Mayo Clinic
Rochester
MN
Disclosures
EM declares no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Hazlewood GA, Aletaha D, Carmona L, et al. Algorithm for identification of undifferentiated peripheral inflammatory arthritis: a multinational collaboration through the 3e initiative. J Rheumatol Suppl. 2011 Mar;87:54-8. Abstract
Neogi T, Jansen TL, Dalbeth N, et al. 2015 Gout classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Ann Rheum Dis. 2015 Oct;74(10):1789-98.Full text Abstract
Aletaha D, Neogi T, Silman AJ, et al. 2010 Rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum. 2010 Sep;62(9):2569-81.Full text Abstract
Plagou A, Teh J, Grainger AJ, et al. Recommendations of the ESSR Arthritis Subcommittee on Ultrasonography in Inflammatory Joint Disease. Semin Musculoskelet Radiol. 2016 Nov;20(5):496-506. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Patient information
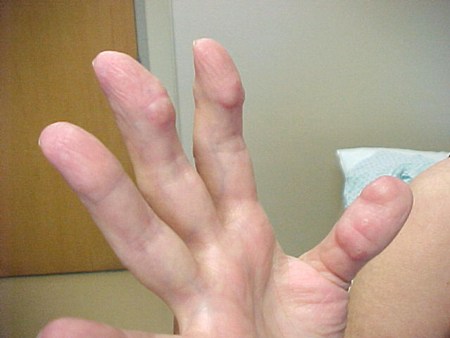
Rheumatoid arthritis
More Patient informationVideos
Aspiration and injection of the knee: animated demonstration
Aspiration and injection of the shoulder animated demonstration
More videosLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer