Summary
Definition
History and exam
Key diagnostic factors
- scaling scalp lesions
- patchy alopecia
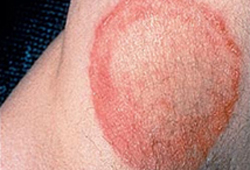
- erythematous, scaling skin lesions with central clearing
- erythematous, scaling rash with follicular pustules in beard or mustache
- erythematous, annular patches on face
- vesicles and scaling of hands
- fissuring, maceration, and scaling in the interdigital spaces of the fourth and fifth toes
- chronically, scaly, hyperkeratotic plantar skin with erythema of the soles, heels, and sides of the feet
- folliculitis with nodules
Other diagnostic factors
- thickened nail with subungual hyperkeratosis, onycholysis, and white-yellow to brown discoloration
- small, white speckled patches on the surface of the nail plate with crumbling nail
- lymphadenopathy
- black-dot alopecia
- milky white nail plate
- area of leukonychia in the proximal nail plate
Risk factors
- exposure to infected people, animals, or soil
- exposure to fomites, including hat, combs, hairbrushes, and upholstery
- chronic topical or oral corticosteroid use
- HIV
- diabetes mellitus and other metabolic disorders
- occlusive clothing
- hot, humid weather
- obesity
- hyperhidrosis
- frequenting public bathing areas while barefoot
- deformities of the feet
- recurrent trauma to the skin
- contact sports
- atopic dermatitis
- positive family history
- peripheral vascular disease
Diagnostic tests
1st tests to order
- potassium hydroxide (KOH) microscopy
Tests to consider
- dermoscopy
- fungal culture
- polymerase chain reaction (PCR)
- Wood lamp exam (ultraviolet light)
Emerging tests
- reflectance confocal microscopy
Treatment algorithm
tinea capitis
tinea barbae, tinea manuum, or Majocchi granuloma
tinea faciale, tinea corporis, tinea cruris, or tinea pedis
tinea unguium (onychomycosis)
Contributors
Authors
Antonella Tosti, MD
Professor of Clinical Dermatology
Dermatology and Cutaneous Surgery
University of Miami Health System
FL
Disclosures
AT received honorarium and travel reimbursement from Valeant, PharmaDerm, and Polichem, is on the speaker bureau for PharmaDerm, and is a consultant for Erchonia Laser and Almirall.
Acknowledgements
Dr Antonella Tosti would like to gratefully acknowledge Dr Keira L. Barr and Dr Barry L. Hainer, the previous contributors to this topic.
Disclosures
KLB declares that she has no competing interests. BLH is on the speaker bureaus for the vaccine programs of Merck and Sanofi-Pasteur pharmaceutical companies.
Peer reviewers
Nanette Silverberg, MD
Clinical Professor of Dermatology
Columbia University College of Physicians and Surgeons
New York City
NY
Disclosures
NS declares that she has no competing interests.
Christina M. Gelbard, MD
Department of Dermatology
UT Dermatology
Health Science Center of Houston
Houston
TX
Disclosures
CMG declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Ameen M, Lear JT, Madan V, et al. British Association of Dermatologists' guidelines for the management of onychomycosis 2014. Br J Dermatol. 2014 Nov;171(5):937-58.Full text Abstract
Fuller LC, Barton RC, Mohd Mustapa MF, et al. British Association of Dermatologists’ guidelines for the management of tinea capitis 2014. Br J Dermatol. 2014 Sep;171(3):454-63.Full text Abstract
Fuller LC, Barton RC, Mohd Mustapa MF, et al. British Association of Dermatologists’ guidelines for the management of tinea capitis 2014. Br J Dermatol. 2014 Sep;171(3):454-63.Full text Abstract
Foley K, Gupta AK, Versteeg S, et al. Topical and device-based treatments for fungal infections of the toenails. Cochrane Database Syst Rev. 2020 Jan 16;(1):CD012093.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Atopic dermatitis
- Dyshidrotic dermatitis
- Lichen simplex chronicus
More DifferentialsGuidelines
- Guidelines for the management of dermatomycosis
- Antifungal agents for common outpatient paediatric infections
More GuidelinesPatient information
Athlete's foot
Ringworm of the body
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer