Magnesium deficiency is a state of decreased total body magnesium content. The human body contains 21-28 g of magnesium, the majority of which is localized in bone (>53%) and nonmuscular tissue (approximately 19%). Hypomagnesemia (low serum magnesium concentration) is generally defined as serum magnesium <1.5 mEq/L.[1]National Institutes of Health. Magnesium: Fact Sheet for Health Professionals. Jun 2022 [internet publication].
https://ods.od.nih.gov/factsheets/Magnesium-HealthProfessional/#en1
Serum magnesium level is a poor indicator of the total magnesium content and availability in the body, because only 1% of magnesium is found in the extracellular fluid. There is no simple, rapid, and accurate laboratory test to determine total body magnesium status in humans.[2]Franz KB. A functional biological marker is needed for diagnosing magnesium deficiency. J Am Coll Nutr. 2004 Dec;23(6):738S-41S.
http://www.ncbi.nlm.nih.gov/pubmed/15637224?tool=bestpractice.com
Evaluating a combination of serum, urinary, and dietary magnesium may be the most appropriate method to determine total body magnesium status.[3]Costello RB, Nielsen F. Interpreting magnesium status to enhance clinical care: key indicators. Curr Opin Clin Nutr Metab Care. 2017 Nov;20(6):504-11.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5812344
http://www.ncbi.nlm.nih.gov/pubmed/28806179?tool=bestpractice.com
[4]Nielsen FH. Guidance for the determination of status indicators and dietary requirements for magnesium. Magnes Res. 2016 Apr 1;29(4):154-60.
http://www.ncbi.nlm.nih.gov/pubmed/28132953?tool=bestpractice.com
Determination of a single 24-hour urinary magnesium level provides an indirect assessment of whole body magnesium content; it should be interpreted in combination with serum magnesium levels.[3]Costello RB, Nielsen F. Interpreting magnesium status to enhance clinical care: key indicators. Curr Opin Clin Nutr Metab Care. 2017 Nov;20(6):504-11.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5812344
http://www.ncbi.nlm.nih.gov/pubmed/28806179?tool=bestpractice.com
Multiple determinations of 24-hour urinary magnesium have been used in epidemiologic studies to assess reproducibility, but are not practical for routine measurement of magnesium status.[3]Costello RB, Nielsen F. Interpreting magnesium status to enhance clinical care: key indicators. Curr Opin Clin Nutr Metab Care. 2017 Nov;20(6):504-11.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5812344
http://www.ncbi.nlm.nih.gov/pubmed/28806179?tool=bestpractice.com
[5]Sun Q, Bertrand KA, Franke AA, et al. Reproducibility of urinary biomarkers in multiple 24-h urine samples. Am J Clin Nutr. 2017 Jan;105(1):159-68.
https://pmc.ncbi.nlm.nih.gov/articles/PMC5183728
http://www.ncbi.nlm.nih.gov/pubmed/28049663?tool=bestpractice.com
[6]Nielsen FH, Johnson LA. Data from controlled metabolic ward studies provide guidance for the determination of status indicators and dietary requirements for magnesium. Biol Trace Elem Res. 2017 May;177(1):43-52.
http://www.ncbi.nlm.nih.gov/pubmed/27778151?tool=bestpractice.com
Magnesium deficiency is usually detected because of the resultant hypomagnesemia. However, it may also be revealed by the development of clinical symptoms or associated hypokalemia or hypocalcemia.
Calcium competes with magnesium for uptake in the loop of Henle, and an increase in the filtered calcium load can impair magnesium reabsorption. Hypomagnesemia, in turn, leads to parathyroid hormone (PTH) resistance and a decrease in PTH secretion, both of which lead to hypocalcemia.
Hypokalemia is commonly seen in patients with hypomagnesemia, partly because the associated underlying disorders can produce both these disturbances. However, there is also evidence that hypomagnesemia can lead to increased renal potassium wasting.
Patients with abnormalities of magnesium homeostasis typically fall into one of three groups:
Patients with magnesium deficiency (low total body magnesium content) and a resultant hypomagnesemia (low serum magnesium concentration)
Patients with hypomagnesemia (low serum magnesium concentration) in the absence of magnesium deficiency (i.e., a normal total body magnesium content)
Patients with magnesium deficiency (low total body magnesium content) but no evidence of hypomagnesemia (i.e., a normal serum magnesium concentration).
Magnesium homeostasis
About 60% of magnesium in the serum is free, whereas approximately 33% is bound to proteins, and <7% is bound to citrate, bicarbonate, ATP, and phosphate.[7]Shils ME. Magnesium. In: Shils ME, Olson JA, Shike M, et al., eds. Modern nutrition in health and disease. 9th ed. New York, NY: Lippincott Williams & Wilkins; 1999:169-192.
Magnesium status is regulated by the intestines, which control absorption; the kidneys, which control excretion; and bone, which is the major storage site. Absorption and excretion are mediated by the selective magnesium channel TRPM6, whereas magnesium uptake and release from tissues outside the intestines and kidneys is controlled by TRPM7, which has an approximately 60% homology to TRPM6.[8]Schlingmann KP, Weber S, Peters M, et al. Hypomagnesemia with secondary hypocalcemia is caused by mutations in TRPM6, a new member of the TRPM gene family. Nat Genet. 2002 Jun;31(2):166-70.
http://www.ncbi.nlm.nih.gov/pubmed/12032568?tool=bestpractice.com
[9]Nadler MJ, Hermosura MC, Inabe K, et al. LTRPC7 is a Mg.ATP-regulated divalent cation channel required for cell viability. Nature. 2001 May 31;411(6837):590-5.
http://www.ncbi.nlm.nih.gov/pubmed/11385574?tool=bestpractice.com
Absorption: magnesium absorption is a saturable process that occurs throughout the small and large intestines, with most of the absorption taking place in the colon. The average daily intake of magnesium is approximately 320 mg in men and 240 mg in women; approximately two-thirds of this amount is eliminated with the feces, while one third is absorbed and passed into the circulation.[10]Wester PO. Magnesium. Am J Clin Nutr. 1987 May;45(5 Suppl):1305-12.
http://www.ncbi.nlm.nih.gov/pubmed/3578120?tool=bestpractice.com
Magnesium regulates the expression of TRPM6; a sustained fall in magnesium level results in increased expression, and increased magnesium absorption.[11]Groenestege WM, Hoenderop JG, van den Heuvel L, et al. The epithelial Mg2+ channel transient receptor potential melastatin 6 is regulated by dietary Mg2+ content and estrogens. J Am Soc Nephrol. 2006 Apr;17(4):1035-43.
http://jasn.asnjournals.org/content/17/4/1035.full
http://www.ncbi.nlm.nih.gov/pubmed/16524949?tool=bestpractice.com
[12]Cao G, Hoenderop JG, Bindels RJ. Insight into the molecular regulation of the epithelial magnesium channel TRPM6. Curr Opin Nephrol Hypertens. 2008 Jul;17(4):373-8.
http://www.ncbi.nlm.nih.gov/pubmed/18660673?tool=bestpractice.com
Excretion and reabsorption: the major site of reabsorption is the loop of Henle, although additional reabsorption takes place in the distal convoluted tubule.[13]Quamme GA, de Rouffignac C. Epithelial magnesium transport and regulation by the kidney. Front Biosci. 2000 Aug 1;5:D694-711.
http://www.ncbi.nlm.nih.gov/pubmed/10922295?tool=bestpractice.com
Approximately 2400 mg/day of magnesium passes through the kidneys, <5% of which is eventually excreted. Because magnesium regulates the expression of TRPM6, a sustained fall in magnesium level results in increased magnesium reabsorption.[11]Groenestege WM, Hoenderop JG, van den Heuvel L, et al. The epithelial Mg2+ channel transient receptor potential melastatin 6 is regulated by dietary Mg2+ content and estrogens. J Am Soc Nephrol. 2006 Apr;17(4):1035-43.
http://jasn.asnjournals.org/content/17/4/1035.full
http://www.ncbi.nlm.nih.gov/pubmed/16524949?tool=bestpractice.com
Although there is no direct hormonal control of magnesium absorption, excretion, and reabsorption, TRPM6 expression appears to be under estrogen modulation.
There is normally very little exchange between intracellular and extracellular magnesium. In the acute phase of a fall in magnesium content, intestinal absorption and renal reabsorption both increase. Hormones such as glucagon, catecholamines, and PTH can mobilize magnesium from bone and other tissues.[14]Romani AM, Scarpa A. Regulation of cellular magnesium. Front Biosci. 2000 Aug 1;5:D720-34.
http://www.ncbi.nlm.nih.gov/pubmed/10922296?tool=bestpractice.com
Magnesium, in turn, exhibits negative feedback on catecholamine release. Conversely, hormones such as insulin, antidiuretic hormone (ADH), and thyroid hormone promote magnesium uptake and storage.[14]Romani AM, Scarpa A. Regulation of cellular magnesium. Front Biosci. 2000 Aug 1;5:D720-34.
http://www.ncbi.nlm.nih.gov/pubmed/10922296?tool=bestpractice.com
Cellular functions of magnesium
Magnesium is a predominantly intracellular ion and is distributed between the nucleus, endoplasmic or sarcoplasmic reticulum, mitochondria, and cytoplasm.[15]Gunther T. Functional compartmentation of intracellular magnesium. Magnesium. 1986;5(2):53-9.
http://www.ncbi.nlm.nih.gov/pubmed/3086631?tool=bestpractice.com
Approximately 200 enzymes involved in cellular metabolism and the cell cycle require magnesium as a cofactor, including adenyl cyclase and ATPases. Magnesium is also an important cofactor for potassium and calcium channels, and therefore plays a role in regulating action potentials in cardiac and neural tissues, as well as calcium signaling in a wide range of tissues.[16]Romani A, Scarpa A. Regulation of cell magnesium. Arch Biochem Biophys. 1992 Oct;298(1):1-12.
http://www.ncbi.nlm.nih.gov/pubmed/1524417?tool=bestpractice.com
Recommended dietary allowance for magnesium
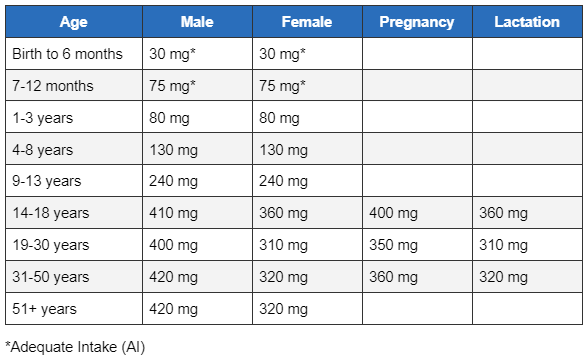
The recommended dietary allowance for magnesium varies according to age and sex as follows:[1]National Institutes of Health. Magnesium: Fact Sheet for Health Professionals. Jun 2022 [internet publication].
https://ods.od.nih.gov/factsheets/Magnesium-HealthProfessional/#en1
[Figure caption and citation for the preceding image starts]: Recommended Dietary Allowances (RDAs) for MagnesiumTable used with permission from the U.S. Department of Health and Human Services, National Institutes of Health. Original source for figures: Institute of Medicine (IOM). Food and Nutrition Board. Dietary reference intakes: calcium, phosphorus, magnesium, vitamin D and fluoride. Washington, DC: National Academy Press, 1997. [Citation ends].