Summary
Definition
History and exam
Key diagnostic factors
- visual field loss
Other diagnostic factors
- headache
- transient visual obscurations
- pulse-synchronous tinnitus
- photophobia
- retrobulbar pain
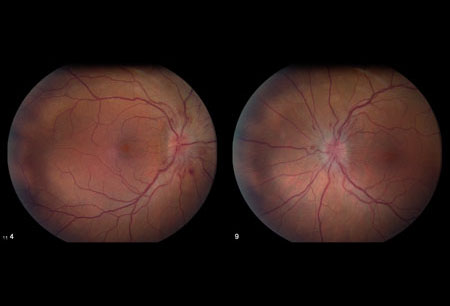
- optical disk swelling
- decreased visual acuity
- ocular motility disturbances
- relative afferent pupillary defect
Risk factors
- female sex
- obesity and weight gain
- certain medication use
- associated causal diseases
- sleep apnea
- family history
Diagnostic tests
1st tests to order
- visual field testing (perimetry)
- dilated fundoscopy
- visual acuity
- MRI of brain with or without contrast
- lumbar puncture at spinal L3/L4
Tests to consider
- magnetic resonance venogram of head
- optical coherence tomography
Treatment algorithm
all patients
Contributors
Authors
Michael Wall, MD
Professor
Department of Neurology and Department of Ophthalmology & Visual Sciences
University of Iowa Hospitals & Clinics and Iowa City VA Health Care System
Iowa City
IA
Disclosures
MW is an author of a number of references cited in this topic.
Mansoor Mughal, MD
Retina Fellow
Rutgers University
Robert Wood Johnson University Hospital
New Brunswick
NJ
Disclosures
MM declares that he has no competing interests.
Peer reviewers
Paul W. Brazis, MD
Consultant in Neurology and Neuro-Ophthalmology
Mayo Clinic Florida
Jacksonville
FL
Disclosures
PWB declares that he has no competing interests.
Tim D. Matthews, MBBS
Consultant Neuro-ophthalmologist
Birmingham Neuro-ophthalmology Unit
University Hospital Birmingham
Birmingham
UK
Disclosures
TDM declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Wall M. Idiopathic intracranial hypertension. Neurol Clin. 2010 Aug;28(3):593-617.Full text Abstract
Johnson LN, Krohel GB, Madsen RW, et al. The role of weight loss and acetazolamide in the treatment of idiopathic intracranial hypertension (pseudotumor cerebri). Ophthalmology. 1998 Dec;105(12):2313-7. Abstract
Hayreh SS. Pathogenesis of oedema of the optic disc (papilloedema): a preliminary report. Br J Ophthalmol. 1964 Oct;48:522-43.Full text Abstract
Smith JL. Whence pseudotumor cerebri? J Clin Neuroophthalmol. 1985 Mar;5(1):55-6. Abstract
Frisen L. Swelling of the optic nerve head: a staging scheme. J Neurol Neurosurg Psychiatry. 1982 Jan;45(1):13-8.Full text Abstract
NORDIC Idiopathic Intracranial Hypertension Study Group Writing Committee; Wall M, McDermott MP, Kieburtz KD, et al. Effect of acetazolamide on visual function in patients with idiopathic intracranial hypertension and mild visual loss: the idiopathic intracranial hypertension treatment trial. JAMA. 2014 Apr 23-30;311(16):1641-51.Full text Abstract
Hoffmann J, Mollan SP, Paemeleire K, et al. European Headache Federation guideline on idiopathic intracranial hypertension. J Headache Pain. 2018 Oct 8;19(1):93.Full text Abstract
Sinclair AJ, Burdon MA, Nightingale PG, et al. Low energy diet and intracranial pressure in women with idiopathic intracranial hypertension: prospective cohort study. BMJ. 2010 Jul 7;341:c2701.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Intracranial structural anomalies
More DifferentialsGuidelines
- European Headache Federation guideline on idiopathic intracranial hypertension
More GuidelinesPatient information
Obesity - drugs and surgery
Tinnitus
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer