Summary
Definition
History and exam
Key diagnostic factors
- Family history
- onset in childhood (MPS, Pompe, Gaucher, Fabry, Niemann-Pick type A)
- onset in adolescence (Fabry, Pompe, Gaucher types 1, 3, mucopolysaccharidosis, Niemann-Pick types B, C)
- onset in adulthood (Fabry, Gaucher type 1, Pompe)
- hepatomegaly and/or splenomegaly
- hyperacusis
- history of renal failure
- skin rash/cutaneous lesions
- large head circumference
- macular "cherry red spot" on ophthalmoscopy
- optic atrophy or retinitis pigmentosa on ophthalmoscopy
- corneal clouding on ophthalmoscopy
- fatigue
Other diagnostic factors
- neurodevelopmental delay
- hearing impairment/sudden deafness
- cataract on ophthalmoscopy
- eye movement disorder
- progressive dementia and ataxia or gait disturbance
- failure to thrive
- joint contracture
- depression
- skeletal abnormalities including spinal gibbus
- hydrocephalus
- history of recurrent respiratory tract infections
- psychosis
- movement disorders
- premature stroke/transient ischemic attack
- cardiomegaly
- valvular cardiac disease
Risk factors
- male sex (mucopolysaccharidosis [MPS] II, Fabry disease)
- Ashkenazi ethnicity
Diagnostic tests
1st tests to order
- enzyme assay
- substrate assay
- DNA analysis
- CBC
Tests to consider
- ECG
- echocardiogram
- pulmonary function tests
- bone marrow biopsy
- muscle biopsy
- CT/MRI of enlarged organ (Gaucher)
- ultrasound/MRI (Fabry)
- CT/x-ray (mucopolysaccharidosis)
Treatment algorithm
type 1 Gaucher disease
type 2 Gaucher disease
type 3 Gaucher disease
Fabry disease
mucopolysaccharidosis (MPS)
Pompe disease
Tay-Sachs disease
Niemann-Pick disease
Contributors
Authors
Atul B. Mehta, MA, MB BChir, MD, FRCP, FRCPath
Consultant Haematologist
Emeritus Professor in Haematology
University College London
London
UK
Disclosures
ABM has participated in educational activities for Sanofi Genzyme, Takeda and Amicus including advisory boards for which he has received honoraria and travel grants. He has also received research funding from Sanofi Genzyme, Takeda and Amicus. He is also an author of a number of references cited in this topic.
Peer reviewers
Gregory M. Pastores, MD
Associate Professor
Departments of Neurology and Pediatrics
NYU School of Medicine
New York
NY
Disclosures
GMP declares that he has no competing interests.
Uma Ramaswami, MD, FRCPCH
Consultant Paediatrician
Paediatric Metabolic Unit
Cambridge University Hospitals
Cambridge
UK
Disclosures
UR has received travel grants, honoraria for lectures, and funding for clinical trials from Shire HGT, Genzyme, and Actelion.
Elmer V. Villanueva, MD, ScM, FRIPH
Associate Professor of Public Health
Director of Research
Gippsland Medical School
Monash University
Churchill
Australia
Disclosures
EVV declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Stirnemann J, Belmatoug N, Camou F, et al. A review of Gaucher disease pathophysiology, clinical presentation and treatments. Int J Mol Sci. 2017 Feb 17;18(2):441.Full text Abstract
Patterson MC, Clayton P, Gissen P, et al. Recommendations for the detection and diagnosis of Niemann-Pick disease type C: an update. Neurol Clin Pract. 2017 Dec;7(6):499-511.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
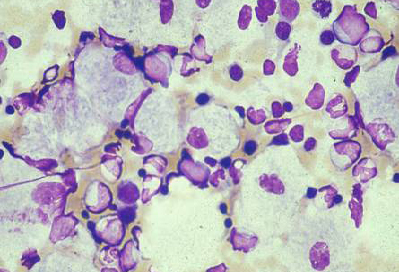
Differentials
- Langerhans cell histiocytosis (differential diagnosis of type 2 and 3 Gaucher disease)
- Rheumatic fever (differential diagnosis of Fabry)
- Bacterial endocarditis (differential diagnosis of Fabry)
More DifferentialsGuidelines
- Cipaglucosidase alfa for treating late onset Pompe disease
- Pegunigalsidase alfa for treating Fabry disease
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer