Recurrent miscarriage is defined by the European Society for Human Reproduction and Embryology and the American Society for Reproductive Medicine as 2 or more failed clinical pregnancies (i.e., documented by ultrasound or histopathology).[1]European Society of Human Reproduction and Embryology (ESHRE). Guideline on the management of recurrent pregnancy loss. Feb 2023 [internet publication].
https://www.eshre.eu/Guidelines-and-Legal
[2]Practice Committee of the American Society for Reproductive Medicine. Evaluation and treatment of recurrent pregnancy loss: a committee opinion. Fertil Steril. 2012 Nov;98(5):1103-11.
http://www.ncbi.nlm.nih.gov/pubmed/22835448?tool=bestpractice.com
It affects about 1% of all fertile couples trying to conceive, in comparison with sporadic nonconsecutive miscarriages, which occur in about 15% to 20% of all pregnancies.[3]Stirrat GM. Recurrent miscarriage. Lancet. 1990 Sep 15;336(8716):673-5.
http://www.ncbi.nlm.nih.gov/pubmed/1975862?tool=bestpractice.com
[4]Ng KYB, Cherian G, Kermack AJ, et al. Systematic review and meta-analysis of female lifestyle factors and risk of recurrent pregnancy loss. Sci Rep. 2021 Mar 29;11(1):7081.
https://www.nature.com/articles/s41598-021-86445-2
http://www.ncbi.nlm.nih.gov/pubmed/33782474?tool=bestpractice.com
A miscarriage includes any pregnancy that ends before the age of viability, which currently stands at 24 weeks' gestation. A miscarriage that occurs before 12 weeks' gestation is commonly termed an early or first-trimester miscarriage, and one that occurs between 13 and 24 weeks' gestation is known as a late or second-trimester miscarriage.
Evaluation can start after 2 or 3 consecutive miscarriages, as prevalence of causes is similar in those with 2, 3, or more miscarriages.[5]Habayeb OM, Konje JC. The one-stop recurrent miscarriage clinic: an evaluation of its effectiveness and outcome. Hum Reprod. 2004 Dec;19(12):2952-8.
https://humrep.oxfordjournals.org/cgi/content/full/19/12/2952
http://www.ncbi.nlm.nih.gov/pubmed/15388685?tool=bestpractice.com
[6]Toth B, Bohlmann M, Hancke K, et al. Recurrent miscarriage: diagnostic and therapeutic procedures. Guideline of the DGGG, OEGGG and SGGG (S2k-Level, AWMF Registry No. 015/050, May 2022). Geburtshilfe Frauenheilkd. 2023 Jan;83(1):49-78.
https://www.thieme-connect.com/products/ejournals/abstract/10.1055/a-1895-9940
http://www.ncbi.nlm.nih.gov/pubmed/37415921?tool=bestpractice.com
Despite a wide range of investigations, no apparent cause is found in >50% of cases of recurrent miscarriage.[7]Quenby SM, Farquharson RG. Predicting recurring miscarriage: what is important? Obstet Gynecol. 1993 Jul;82(1):132-8.
http://www.ncbi.nlm.nih.gov/pubmed/8515913?tool=bestpractice.com
About 70% of patients with no cause found will achieve a live birth in the subsequent pregnancy depending on the age of the woman and the number of previous miscarriages.[5]Habayeb OM, Konje JC. The one-stop recurrent miscarriage clinic: an evaluation of its effectiveness and outcome. Hum Reprod. 2004 Dec;19(12):2952-8.
https://humrep.oxfordjournals.org/cgi/content/full/19/12/2952
http://www.ncbi.nlm.nih.gov/pubmed/15388685?tool=bestpractice.com
[7]Quenby SM, Farquharson RG. Predicting recurring miscarriage: what is important? Obstet Gynecol. 1993 Jul;82(1):132-8.
http://www.ncbi.nlm.nih.gov/pubmed/8515913?tool=bestpractice.com
[Figure caption and citation for the preceding image starts]: Predicted percentage success rate of subsequent pregnancy according to age and previous miscarriage historyCreated by the BMJ Group; data from Brigham SA, et al. Hum Reprod. 1999;14:2868-2871 [Citation ends].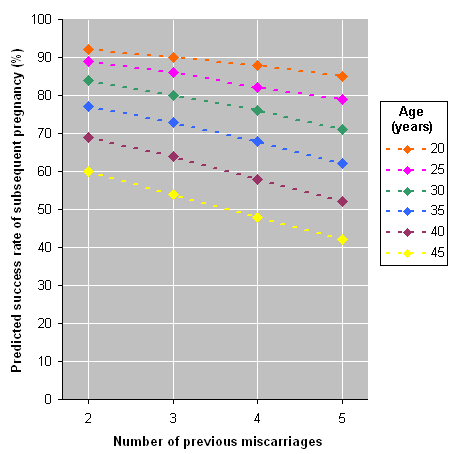
Definite associations of recurrent miscarriage include chromosomal abnormalities, antiphospholipid syndrome, certain structural uterine abnormalities such as septate uterus, and certain thrombophilias. However, a reduction in risk of miscarriage in a subsequent pregnancy following treatment has not been proven unequivocally for most of these conditions. Controversy surrounds the possible association of other conditions with recurrent miscarriage, including immunologic factors, other uterine abnormalities (e.g., cervical insufficiency), infection, and male and endocrinologic factors. There is a need for high-quality and methodologically sound research to guide management of these patients.[8]Hennessy M, Dennehy R, Meaney S, et al. Clinical practice guidelines for recurrent miscarriage in high-income countries: a systematic review. Reprod Biomed Online. 2021 Jun;42(6):1146-71.
https://www.rbmojournal.com/article/S1472-6483(21)00100-0/fulltext
http://www.ncbi.nlm.nih.gov/pubmed/33895080?tool=bestpractice.com
Risk factors
Increasing maternal age reduces the chance of a successful live birth. Women ages 20 years with 2 previous miscarriages have a 92% chance of success in the next pregnancy compared with only a 60% chance of success in women ages 45 years with 2 previous miscarriages.[9]Brigham SA, Conlon C, Farquharson RG. A longitudinal study of pregnancy outcome following idiopathic recurrent miscarriage. Hum Reprod. 1999 Nov;14(11):2868-71.
https://humrep.oxfordjournals.org/cgi/content/full/14/11/2868
http://www.ncbi.nlm.nih.gov/pubmed/10548638?tool=bestpractice.com
Advanced paternal age also appears to be associated with greater risk for spontaneous miscarriage.[10]Kleinhaus K, Perrin M, Friedlander Y, et al. Paternal age and spontaneous abortion. Obstet Gynecol. 2006 Aug;108(2):369-77.
http://www.ncbi.nlm.nih.gov/pubmed/16880308?tool=bestpractice.com
[11]Nguyen BT, Chang EJ, Bendikson KA. Advanced paternal age and the risk of spontaneous abortion: an analysis of the combined 2011-2013 and 2013-2015 National Survey of Family Growth. Am J Obstet Gynecol. 2019 Nov;221(5):476.e1-7.
http://www.ncbi.nlm.nih.gov/pubmed/31128112?tool=bestpractice.com
[12]du Fossé NA, van der Hoorn MP, van Lith JMM, et al. Advanced paternal age is associated with an increased risk of spontaneous miscarriage: a systematic review and meta-analysis. Hum Reprod Update. 2020 Sep 1;26(5):650-69.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7456349
http://www.ncbi.nlm.nih.gov/pubmed/32358607?tool=bestpractice.com
Increased frequency of chromosomal anomalies in sperm has been implicated.[13]Slama R, Bouyer J, Windham G, et al. Influence of paternal age on the risk of spontaneous abortion. Am J Epidemiol. 2005 May 1;161(9):816-23.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7456349
http://www.ncbi.nlm.nih.gov/pubmed/15840613?tool=bestpractice.com
In one systematic review and meta-analysis, risk for pregnancy loss <20 weeks was increased by 23% and 43% among men ages 40-44 and ≥45 years, respectively (compared with men ages 25-29 years).[12]du Fossé NA, van der Hoorn MP, van Lith JMM, et al. Advanced paternal age is associated with an increased risk of spontaneous miscarriage: a systematic review and meta-analysis. Hum Reprod Update. 2020 Sep 1;26(5):650-69.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7456349
http://www.ncbi.nlm.nih.gov/pubmed/32358607?tool=bestpractice.com
Primigravidas and patients who consistently have successful pregnancies have only about 5% risk of miscarriage, compared with 24% in patients who have previously miscarried.[14]Regan L, Braude PR, Trembath PL. Influence of past reproductive performance on risk of spontaneous abortion. BMJ. 1989 Aug 26;299(6698):541-5.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1837397
http://www.ncbi.nlm.nih.gov/pubmed/2507063?tool=bestpractice.com
Other studies similarly show a trend of miscarriage rate increasing with the number of previous miscarriages.[9]Brigham SA, Conlon C, Farquharson RG. A longitudinal study of pregnancy outcome following idiopathic recurrent miscarriage. Hum Reprod. 1999 Nov;14(11):2868-71.
https://humrep.oxfordjournals.org/cgi/content/full/14/11/2868
http://www.ncbi.nlm.nih.gov/pubmed/10548638?tool=bestpractice.com
[15]Ogasawara M, Aoki K, Okada S, et al. Embryonic karyotype of abortuses in relation to the number of previous miscarriages. Fertil Steril. 2000 Feb;73(2):300-4.
http://www.ncbi.nlm.nih.gov/pubmed/10685533?tool=bestpractice.com
Therefore, the risk of miscarriage is directly related to the outcome of previous pregnancies.
Recurrent miscarriage is a stressful condition, so alongside medical investigations and appropriate treatment, patient education, counseling, and support should be provided.
Log in or subscribe to access all of BMJ Best Practice
