Summary
Definition
History and exam
Key diagnostic factors
- periorbital/retro-ocular pain
- loss of visual acuity with scotoma
- color desaturation/loss of color vision
- relative afferent papillary defect (RAPD)
Other diagnostic factors
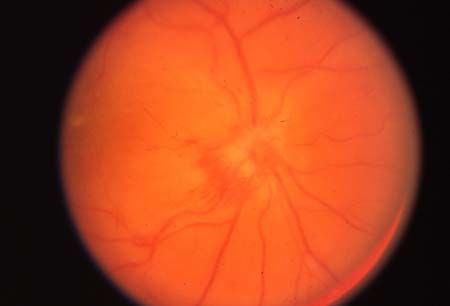
- optic disk swelling
- neurologic abnormalities of multiple sclerosis
- Uhthoff phenomenon
- phosphenes
- Pulfrich phenomenon
- perivenous sheathing
Risk factors
- age 30 to 50 years
- female sex
- white ethnicity
- HLA-DRB1*1501 genotype
- risk factors for multiple sclerosis (MS; Epstein-Barr virus [EBV] infection, vitamin D deficiency, and smoking)
- childhood in higher latitudes
- presence of autoimmune disease
- exposure to infectious diseases, such as Lyme disease and syphilis
Diagnostic tests
1st tests to order
- MRI - brain
- CBC
- ESR
- C-reactive protein
- venereal disease research laboratory (VDRL)
- aquaporin-4 (AQP4) antibody, myelin oligodendrocyte glycoprotein (MOG) antibody, and collapsin response mediator protein 5 (CRMP5) antibody
- uric acid
- serum ACE
- ANA
- B12 and folate
Tests to consider
- Lyme titer
- cerebrospinal fluid analysis
Treatment algorithm
acute episode
coexisting inflammatory diseases (e.g., NMOSD, MOGAD, SLE or sarcoidosis)
Contributors
Authors
Cris S. Constantinescu, MD, PhD
Chair of Neurology Emeritus
Academic Unit of Mental Health and Clinical Neuroscience
University of Nottingham
Nottingham
UK
Attending Neurologist
Professor of Neurology
Cooper Neuroscience Institute
Camden
New Jersey
Disclosures
CSC has received research support or consultancy fees from Biogen, GW, Merck, Morphosys, Novartis, Roche, Sanofi-Pasteur, MSD, and Teva. CSC is an author of a number of references cited in this topic.
Thomas M. Bosley, MD

Knights Templar Eye Foundation Professor of Ophthalmology
Wilmer Eye Institute
Johns Hopkins University
Baltimore
MD
Disclosures
TMB declares that he has no competing interests.
Peer reviewers
Gus Gazzard, MA, MBBChir, MD, FRCOphth
Consultant Ophthalmic Surgeon
King's College Hospital
Honorary Research Fellow
Institute of Ophthalmology
London
UK
Disclosures
GG declares that he has no competing interests.
John Selhorst, MD
Professor
Department of Neurology and Psychiatry
Saint Louis University
St. Louis
MO
Disclosures
JS declares that he has no competing interests.
Efstratios Mendrinos, MD
Department of Ophthalmology
Geneva University Hospitals
Geneva
Switzerland
Disclosures
EM declares that he has no competing interests.
Jonathan Smith, MD
Specialist Registrar in Ophthalmology
Royal Victoria Infirmary
Newcastle
UK
Disclosures
JS declares that he has no competing interests.
Peter Sguigna, MD
Assistant Professor
Department of Neurology
The University of Texas
Southwestern Medical Center
Dallas
TX
Disclosures
PS has received grant support from National Multiple Sclerosis Society, International Progressive Multiple Sclerosis Alliance, National Institute of Health (NIH), Center for Translational Medicine, Physician Scientist Training Program, and Department of Defense (DOD). He has received research support from Genentech, Clene Nanomedicine, and Patient Centered Outcomes Research Institute. He has received consulting fees from Medical Logix LLC, Genentech, EMD Serono, Horizon Therapeutics, and Bristol Myers Squibb. He is the inventor on a patent for OCT technology that is held by UT Southwestern Medical Center.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Petzold A, Fraser CL, Abegg M, et al. Diagnosis and classification of optic neuritis. Lancet Neurol. 2022 Dec;21(12):1120-34. Abstract
American Academy of Ophthalmology. Optic neuritis - 2012. Jul 2012 [internet publication].Full text
Beck RW, Cleary PA, Anderson MM Jr, et al. A randomized, controlled trial of corticosteroids in the treatment of acute optic neuritis. The Optic Neuritis Study Group. N Engl J Med. 1992 Feb 27;326(9):581-8. Abstract
Thompson AJ, Banwell BL, Barkhof F, et al. Diagnosis of multiple sclerosis: 2017 revisions of the McDonald criteria. Lancet Neurol. 2018 Feb;17(2):162-73.Full text Abstract
Sellner J, Boggild M, Clanet M, et al. EFNS guidelines on diagnosis and management of neuromyelitis optica. Eur J Neurol. 2010 Aug;17(8):1019-32.Full text Abstract
Gal RL, Vedula SS, Beck R. Corticosteroids for treating optic neuritis. Cochrane Database Syst Rev. 2015 Aug 14;(8):CD001430.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Lyme disease
- Syphilis
- HIV infection
More DifferentialsGuidelines
- Optic neuritis
- Guidelines on diagnosis and management of neuromyelitis optica
More GuidelinesPatient information
Lyme disease
Multiple sclerosis
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer