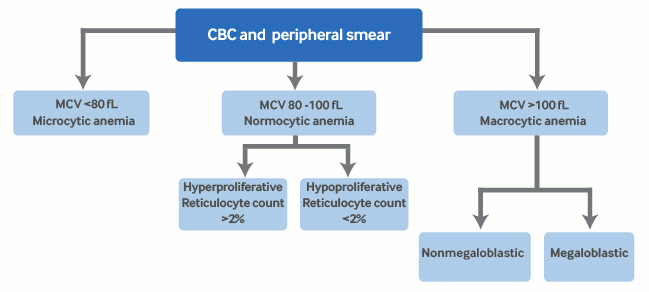
Summary
Differentials
Common
- Trauma
- Acute gastrointestinal bleeding
- Rupture of a vascular aneurysm
- Surgery
- Menorrhagia
- Iron deficiency
- Vitamin B12 deficiency
- Folate deficiency
- Myelodysplastic syndrome
- Acute lymphoblastic leukemia
- Acute myeloid leukemia
- Chronic myeloid leukemia
- Hairy cell leukemia
- Acquired aplastic anemia
- Infiltration by secondary malignancy
- Pure red cell aplasia
- Drug toxicity
- Anemia of chronic disease
- Chronic kidney disease
- Chronic liver disease
- Pregnancy
Uncommon
- Generalized malnutrition
- Cytotoxic chemotherapy
- Radiation therapy
- Alcohol misuse
- Lead toxicity
- Hypothyroidism
- Autoimmune hemolytic anemia
- Transfusion reaction
- Malaria
- Viral hepatitis
- Toxoplasmosis
- Leishmaniasis
- Parvovirus B19 infection
- Infectious mononucleosis
- Cytomegalovirus (CMV)
- Sickle cell anemia
- Thalassemias
- Hereditary spherocytosis
- Glucose-6-phosphate dehydrogenase deficiency (G6PD)
- Bone marrow failure syndromes
- Hemolytic uremic syndrome
- Disseminated intravascular coagulation (DIC)
- Thrombotic thrombocytopenic purpura
- Hemangioma
- Malignant hypertension
- Prosthetic valves and surfaces
- Cutaneous burns
Contributors
Authors
Robert Zaiden, MD
Hematologist Oncologist
Baptist MD Anderson Cancer Center
Jacksonville
FL
Disclosures
RZ declares that he has no competing interests.
Acknowledgements
Dr Robert Zaiden would like to gratefully acknowledge Dr Fauzia Rana, a previous contributor to this topic.
Disclosures
FR declares that she has no competing interests.
Peer reviewers
Christoph Pechlaner, MD
Associate Professor of Medicine
Innsbruck Medical University
Innsbruck
Austria
Disclosures
CP declares that he has no competing interests.
John Densmore, MD, PhD
Associate Professor of Clinical Medicine
Department of Medicine
Division of Hematology/Oncology
University of Virginia
Charlottesville
VA
Disclosures
JD declares that he has no competing interests.
Carlos Aravena, MD
Internal Medicine Instructor
Member of Evidence Based Medicine Unit
Catholic University of Chile
Santiago
Chile
Disclosures
CA declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Snook J, Bhala N, Beales ILP, et al. British Society of Gastroenterology guidelines for the management of iron deficiency anaemia in adults. Gut. 2021 Nov;70(11):2030-51.Full text Abstract
Ko CW, Siddique SM, Patel A, et al. AGA clinical practice guidelines on the gastrointestinal evaluation of iron deficiency anemia. Gastroenterology. 2020 Sep;159(3):1085-94.Full text Abstract
Kulasekararaj A, Cavenagh J, Dokal I, et al. Guidelines for the diagnosis and management of adult aplastic anaemia: a British Society for Haematology guideline. Br J Haematol. 2024 Mar;204(3):784-804.Full text Abstract
Bain BJ, Daniel Y, Henthorn J, et al. Significant haemoglobinopathies: a guideline for screening and diagnosis. Br J Haematol. 2023 Jun;201(6):1047-65.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
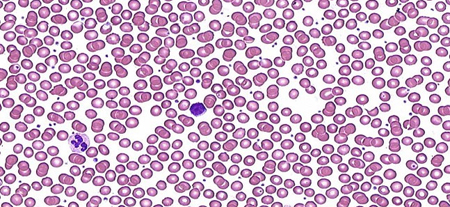
Patient information
Anemia, iron deficiency
More Patient informationVideos
Venepuncture and phlebotomy: animated demonstration
More videosLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer