Summary
Definition
History and exam
Key diagnostic factors
- right upper quadrant abdominal pain
- hepatomegaly
- ascites
- jaundice
Other diagnostic factors
- splenomegaly
- gastrointestinal bleeding
- leg edema
- truncal venous collaterals
- hepatic encephalopathy
Risk factors
- female sex
- myeloproliferative disorders (MPD)
- thrombophilic disorders
- oral contraceptive pill use
- pregnancy and immediate postpartum period
Diagnostic tests
1st tests to order
- thrombophilia screening
- color and pulsed Doppler ultrasound
- LFTs
- BUN and creatinine
- coagulation profile
- CBC
- Janus kinase 2 (JAK2) mutation
- flow cytometry for CD55- and CD59-deficient blood cells
Tests to consider
- serum-ascites albumin gradient (SAAG)
- total ascitic protein
- CT abdomen
- MRI abdomen
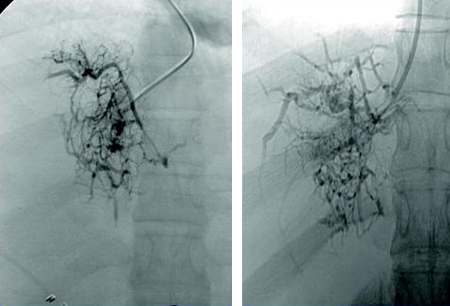
- hepatic venography
- contrast-enhanced 3-dimensional magnetic resonance angiography
- transjugular liver biopsy
- bone marrow biopsy
Treatment algorithm
primary: nonfulminant
primary: fulminant
secondary Budd-Chiari syndrome
Contributors
Authors
Soha Saoud Abdel Moneim, MD, PhD

Lecturer of Gastroenterology and Hepatology
Assiut University
Assiut
Egypt
Disclosures
SSAM declares that she has no competing interests.
Vijay H. Shah, MD

Professor of Medicine
Physiology and Cancer Cell Biology
Mayo Clinic
Rochester
MN
Disclosures
VHS is the author of studies referenced in this topic. VHS has been reimbursed by the following organizations for Advisory Board Meetings: Akaza Bioscience, AgomAb Therapeutics, Generon Shanghai, Intercept Pharmaceuticals, Inc., Mallinckrodt Pharmaceuticals, Resolution Therapeutics, Ltd., and Surrozen. Dr. Shah has been reimbursed by the following organizations for general consulting: Ambys Medicines, Durect Corporation, Genfit SA, HepaRegeniX, Korro Bio, Inc., Novartis Pharma AG, and Seal Rock Therapeutics, Inc..
Peer reviewers
Vikas Gupta, MD, PhD
Assistant Professor of Medicine
Yale School of Medicine
Department of Medicine
Section of Digestive Diseases
New Haven
CT
Disclosures
VG declares that he has no competing interests.
Philip Newsome, PhD, FRCPE
Senior Lecturer in Hepatology & Honorary Consultant Physician
Liver Research Group
Institute of Biomedical Research
The Medical School
University of Birmingham
Birmingham
UK
Disclosures
PN declares that he has no competing interests.
Muhammad Dawwas, MRCP
Specialist Registrar
Liver Unit
Addenbrooke's Hospital
Cambridge
UK
Disclosures
Not disclosed.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Northup PG, Garcia-Pagan JC, Garcia-Tsao G, et al. Vascular liver disorders, portal vein thrombosis, and procedural bleeding in patients with liver disease: 2020 practice guidance by the American Association for the Study of Liver Diseases. Hepatology. 2021 Jan;73(1):366-413.Full text Abstract
de Franchis R, Bosch J, Garcia-Tsao G, et al. Baveno VII - Renewing consensus in portal hypertension. J Hepatol. 2022 Apr;76(4):959-74.Full text Abstract
Valla DC. The diagnosis and management of the Budd-Chiari syndrome: consensus and controversies. Hepatology. 2003;38:793-803. Abstract
Menon KV, Shah V, Kamath PS. The Budd-Chiari syndrome. N Engl J Med. 2004;350:578-585. Abstract
European Association for the Study of the Liver. EASL clinical practice guidelines: vascular diseases of the liver. J Hepatol. 2016;64:179-202.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Sinusoidal obstruction syndrome (SOS) (veno-occlusive disease)
- Fulminant hepatic failure due to other etiologies
- Congestive hepatopathy
More DifferentialsGuidelines
- Baveno VII – Renewing consensus in portal hypertension
- Budd-Chiari syndrome: consensus guidance of the Asian Pacific Association for the Study of the Liver
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer