Summary
Definition
History and exam
Key diagnostic factors
- presence since birth
- asymmetric, indistinct or irregularly bordered, variably colored papules with diameter >5 mm
- history of change in shape and color
- asymptomatic (usually)
- multiple lesions
- flat, brown macule
- dome-shaped papule
- light brown background with speckled darker brown spots within
- blue-gray dome-shaped papule
- central pink-to-brown papule with a surrounding depigmented white ring
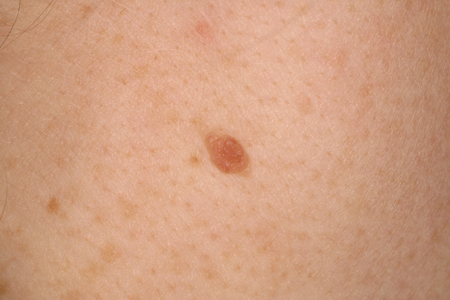
- pinkish-brown papule
Risk factors
- genetic predisposition
- fair skin
- age: older children and young adults
- ultraviolet exposure
Diagnostic tests
1st tests to order
- dermatoscopy
Tests to consider
- non-invasive imaging technologies
- total body photography
- biopsy
Emerging tests
- whole genome sequencing
- pigmented lesion assay (PLA)
Treatment algorithm
clinically benign
clinically suspicious for melanoma
Contributors
Authors
Jason B. Lee, MD

Professor of Dermatology & Cutaneous Biology
Clinical Vice-Chair
Director of Dermatopathology Fellowship
Director of Pigmented Lesion Clinic
Thomas Jefferson University
Philadelphia
PA
Disclosures
JBL declares that he has no competing interests.
Acknowledgements
Dr Jason B. Lee would like to gratefully acknowledge Dr Laurel R. Schwartz, a previous contributor to this topic.
Disclosures
LRS declares that she has no competing interests.
Peer reviewers
Craig G. Burkhart, MD
Clinical Professor
Department of Medicine
Medical College of Ohio
Toledo
OH
Disclosures
CGB declares that he has no competing interests.
Mark Hurt, MD
Dermatologist
Cutaneous Pathology
WCP Laboratories
Missouri
MO
Disclosures
MH declares that he has no competing interests.
Veronique Bataille, MBBS
Consultant Dermatologist
West Herts NHS Trust and King's College London
London
UK
Disclosures
VB declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Duffy K, Grossman D. The dysplastic nevus: from historical perspective to management in the modern era: part I. Historical, histologic, and clinical aspects. J Am Acad Dermatol. 2012 Jul;67(1):1.e1-16. Abstract
Duffy K, Grossman D. The dysplastic nevus: from historical perspective to management in the modern era. Part II. Molecular aspects and clinical management. J Am Acad Dermatol. 2012 Jul;67(1):19.e1-12. Abstract
US Preventive Services Task Force. Final recommendation statement. Skin cancer: screening. Apr 2023 [internet publication].Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Melanoma
- Seborrheic keratosis
- Solar lentigo
More DifferentialsGuidelines
- Skin cancer: screening
- The 2018 World Health Organization classification of cutaneous, mucosal, and uveal melanoma: detailed analysis of 9 distinct subtypes defined by their evolutionary pathway
More GuidelinesPatient information
Skin cancer (melanoma): what is it?
Skin cancer (melanoma): how is it diagnosed and treated?
More Patient informationVideos
Intradermal injection animation demonstration
More videosLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer