შეჯამება
განსაზღვრება
History and exam
Key diagnostic factors
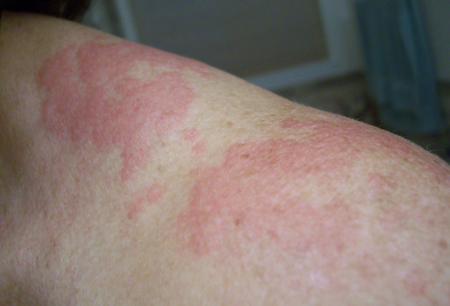
- erythematous edematous lesions
- pruritus
- resolution within 24 hours
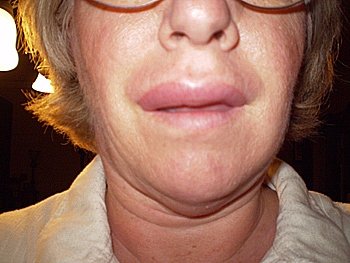
- swelling of face, tongue, or lips
Other diagnostic factors
- blanching lesions
- stridor
Risk factors
- positive family history
- female sex
- exposure to drug trigger
- exposure to food trigger
- recent viral infection
- recent insect bite or sting
Diagnostic tests
1st tests to order
- CBC with differential
- erythrocyte sedimentation rate (ESR)
- CRP
- C4 level
Tests to avoid
- IgG testing
Tests to consider
- thyroid-stimulating hormone (TSH)
- antinuclear antibodies (ANA)
- skin prick testing
- allergen avoidance diet
- serum tryptase
- skin biopsy
- C1 esterase inhibitor level
- C1 esterase inhibitor function
- C1q levels
- specific IgE to suspected allergen
Treatment algorithm
acute urticaria ± angioedema
hereditary angioedema
chronic urticaria ± angioedema
drug-induced angioedema without urticaria
idiopathic angioedema without urticaria
hereditary angioedema
Contributors
Authors
Jonathan Bernstein, MD
Professor of Medicine
Department of Internal Medicine
Division of Immunology/Allergy Section
University of Cincinnati
Cincinnati
OH
Disclosures
JB is a consultant, contracted researcher, and speaker for Sanofi-Regeneron, AstraZeneca, Novartis/Regeneron, Genentech, Shire/Takeda, CSL Behring, Pharming and Biocryst. He is also a consultant and contracted researcher for Amgen, Allakos, Celldex, Kalvista, Biomarin and IONIS. JB is a consultant for Escient, Ono and Pharvaris, he is on the board of directors for AAAAI, and is a member of the Joint Task Force practice parameter. JB has spoken on this topic at National, International and Regional/Local Educational meetings. JB is an author of abstracts and manuscripts related to these topics and is an author of a number of references cited in this topic.
Acknowledgements
Dr Jonathan Bernstein would like to gratefully acknowledge Dr S. Shahzad Mustafa and Dr Stephen Dreskin, previous contributors to this topic.
Disclosures
SM is on the speakers' panel and advisory board for Genentech. SD declares that he has no competing interests.
Peer reviewers
Frances Humphreys, MB BS, FRCP
Consultant Dermatologist
Warwick Hospital
Honorary Associate Professor
University of Warwick
Warwick Hospital
Warwick
UK
Disclosures
FH has attended educational events organised and funded by Almrall and Schering Plough; has received a speaker's fee from Steibel, Leo, and Schering Plough; and is an author of references cited in this topic.
Alexander M. Marsland, MRCP
Consultant in Dermatology
University Hospital of South Manchester
Manchester
UK
Disclosures
None declared.
Luz Fonacier, MD
Head of Allergy and Training Program Director
Winthrop University Hospital
Associate Professor of Clinical Medicine
SUNY at Stony Brook
Stony Brook
NY
Disclosures
LF declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Zuberbier T, Abdul Latiff AH, Abuzakouk M, et al. The international EAACI/GA²LEN/EuroGuiDerm/APAAACI guideline for the definition, classification, diagnosis, and management of urticaria. Allergy. 2022 Mar;77(3):734-66.Full text Abstract
Fine LM, Bernstein JA. Guideline of chronic urticaria beyond. Allergy Asthma Immunol Res. 2016 Sep;8(5):396-403.Full text Abstract
Powell RJ, Leech SC, Till S, et al. BSACI guideline for the management of chronic urticaria and angioedema. Clin Exp Allergy. 2015;45:547-565.Full text Abstract
Maurer M, Magerl M, Betschel S, et al. The international WAO/EAACI guideline for the management of hereditary angioedema-The 2021 revision and update. Allergy. 2022 Jul;77(7):1961-90.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Diferenciales
- Anaphylaxis
- Dermatographism
- Atopic dermatitis
More DiferencialesGuías de práctica clínica
- The international WAO/EAACI guideline for the management of hereditary angioedema: the 2021 revision and update
- Guidelines for the management of people with chronic urticaria
More Guías de práctica clínicaInicie sesión o suscríbase para acceder a todo el BMJ Best Practice
El uso de este contenido está sujeto a nuestra cláusula de exención de responsabilidad