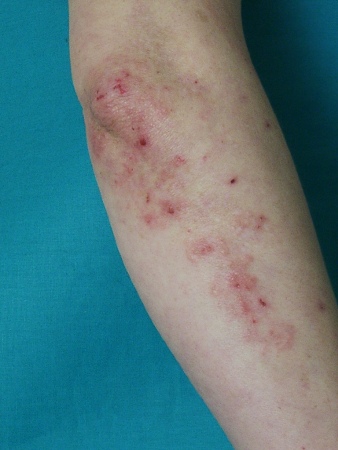
Summary
Differentials
Common
- Oral allergy syndrome
- Atopic dermatitis
- Food protein-induced proctocolitis
- Celiac disease
- Lactose intolerance
Uncommon
- Food-induced anaphylaxis
- Food-dependent exercise-induced anaphylaxis
- Eosinophilic esophagitis
- Food protein-induced enterocolitis
- Congenital sucrase isomaltase deficiency
- Monosodium glutamate (MSG) reactions
- Tyramine reactions
- Sulfite sensitivity
- Galactose-alpha-1,3-galactose (alpha-gal) allergy (tick borne)
Contributors
Authors
J. Andrew Bird, MD
Associate Professor
Department of Pediatrics
Division of Allergy and Immunology
University of Texas Southwestern Medical Center
Dallas
TX
Disclosures
JAB has received grant funding from DBV Technologies, FARE, and Aimmune Therapeutics, and he has received advisory board fees from DBV Technologies, FARE, Pharm-Olam International Ltd, Aimmune Therapeutics, Pfizer Pharmaceuticals, Allergy Therapeutics Ltd, and AllerGenis. He has received speaking fees from Abbott, DBV Technologies, and Aimmune Therapeutics.
A. Wesley Burks, MD

Curnen Distinguished Professor and Chair
Department of Pediatrics
University of North Carolina
Chapel Hill
NC
Disclosures
AWB receives grant support to his institution from the National Institutes of Health, Food Allergy Research & Education, and Allergen Research Corporation; royalties from UpToDate; consulting honorariums from Aravax, Astella Pharma Global Development, DBV Technologies and N-Fold, LLC, as well as Aimmune Therapeutics, Consortia TX, Inc., Intrommune Therapeutics, and Prota Therapeutics for his service on their respective Scientific Advisory Boards. AWB has consulted for the following companies (which are all now expired): Biomerica, Inc., Evelo Biosciences/Epiva, Genentech, Insys Therapeutics, PPD Development, Sanofi US Services, Valeant Pharmaceuticals North America, LLC, LEK Consulting, LLC, Hycor Biomedical. AWB has received payments for speaking at the Gordon Research Conferences, the Pediatric Allergy and Asthma Meeting, and the American College of Allergy Asthma and Immunology. AWB is a minority stockholder of both Allertein and Mastcell Pharmaceuticals stock. These interests do not directly relate to the article but are being shared for full disclosure. AWB is an author of references cited in this topic.
Acknowledgements
Dr J. Andrew Bird and Dr A. Wesley Burks would like to gratefully acknowledge Dr Alison Church, previous contributor to this topic.
Disclosures
AC declares that she has no competing interests.
Peer reviewers
Aaron Lerner, MD
Head of Pediatric Gastroenterology and Nutrition Unit
Carmel Medical Center
Haifa
Israel
Disclosures
AL declares that he has no competing interests.
Roy Gerth van Wijk, MD, PhD
Professor of Allergology
Head of Section of Allergology
Department of Internal Medicine
Erasmus Medical Center
Rotterdam
The Netherlands
Disclosures
RGvW declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Shaker MS, Wallace DV, Golden DBK, et al. Anaphylaxis-a 2020 practice parameter update, systematic review, and Grading of Recommendations, Assessment, Development and Evaluation (GRADE) analysis. J Allergy Clin Immunol. 2020 Apr;145(4):1082-123.Full text Abstract
Lieberman P, Nicklas RA, Randolph C, et al. Anaphylaxis - a practice parameter update 2015. Ann Allergy Asthma Immunol. 2015 Nov;115(5):341-84. Abstract
Golden DBK, Wang J, Waserman S, et al. Anaphylaxis: a 2023 practice parameter update. Ann Allergy Asthma Immunol. 2024 Feb;132(2):124-76.Full text Abstract
Rubio-Tapia A, Hill ID, Semrad C, et al. American College of Gastroenterology guidelines update: diagnosis and management of celiac disease. Am J Gastroenterol. 2023 Jan 1;118(1):59-76.Full text Abstract
Sampson HA, Aceves S, Bock SA, et al. Food allergy: a practice parameter update-2014. J Allergy Clin Immunol. 2014 Nov;134(5):1016-25.e43.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Use of this content is subject to our disclaimer