Resumo
Definição
História e exame físico
Principais fatores diagnósticos
- hypercyanotic episodes
- harsh systolic ejection murmur
- cyanosis
- tachypnea
Outros fatores diagnósticos
- shock
Fatores de risco
- trisomy 21, 18, or 13
- chromosome 22q11 deletions (DiGeorge syndrome)
- Jagged1 gene mutations (Alagille syndrome)
- mutation in NKX2.5 gene
- environmental factors
- family history of congenital heart disease
Investigações diagnósticas
Primeiras investigações a serem solicitadas
- pulse oximetry
- echocardiogram
- ECG
- CXR
- hyperoxygenation test
Investigações a serem consideradas
- cardiac CT angiography or MRI
- cardiac catheterization
Algoritmo de tratamento
hypercyanotic spells
neonate with profound cyanosis and severely limited pulmonary blood flow
neonate or infant with nonremitting severe cyanosis
all patients
Colaboradores
Autores
Jeffrey Gossett, MD

Vice President and System Chief of Pediatric Cardiology
Professor of Pediatrics
Division of Pediatric Cardiology
Cohen Children’s Medical Center, Northwell Health
New Hyde Park
NY
Declarações
JG declares that he has no competing interests.
Agradecimentos
Dr Jeffrey Gossett would like to gratefully acknowledge Dr Anna Kamp, a previous contributor to this topic.
Declarações
AK declares that she has no competing interests.
Revisores
Adam B. Christopher, MD
Assistant Professor of Pediatrics
Director of Cardiac MRI
UPMC Children's Hospital of Pittsburgh
Pittsburgh
PA
Declarações
ABC declares that he has no competing interests.
Ranjit Aiyagari, MD
Clinical Assistant Professor of Pediatrics
University of Michigan
Ann Arbor
MI
Declarações
RA declares that he has no competing interests.
Michael Cheung, BSc, MBChB, MD
Deputy Director
Department of Cardiology
Royal Children's Hospital
Melbourne
Australia
Declarações
MC declares that he has no competing interests.
Créditos aos pareceristas
Os tópicos do BMJ Best Practice são constantemente atualizados, seguindo os desenvolvimentos das evidências e das diretrizes. Os pareceristas aqui listados revisaram o conteúdo pelo menos uma vez durante a história do tópico.
Declarações
As afiliações e declarações dos pareceristas referem--se ao momento da revisão.
Referências
Principais artigos
Valente AM, Cook S, Festa P, et al. Multimodality imaging guidelines for patients with repaired tetralogy of Fallot: a report from the American Society of Echocardiography: developed in collaboration with the Society for Cardiovascular Magnetic Resonance and the Society for Pediatric Radiology. J Am Soc Echocardiogr. 2014 Feb;27(2):111-41. Resumo
Hirsch JC, Mosca RS, Bove EL. Complete repair of tetralogy of Fallot in the neonate: results in the modern era. Ann Surg. 2000 Oct;232(4):508-14.Texto completo Resumo
Habib G, Lancellotti P, Antunes MJ, et al. 2015 ESC guidelines for the management of infective endocarditis. Eur Heart J. 2015 Nov 21;36(44):3075-128.Texto completo Resumo
Stout KK, Daniels CJ, Aboulhosn JA, et al. 2018 AHA/ACC guideline for the management of adults with congenital heart disease: a report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines. Circulation. 2019 Apr 2;139(14):e698-800.Texto completo Resumo
Lui GK, Saidi A, Bhatt AB, et al. Diagnosis and management of noncardiac complications in adults with congenital heart disease: a scientific statement from the American Heart Association. Circulation. 2017 Nov 14;136(20):e348-92.Texto completo Resumo
Baumgartner H, De Backer J, Babu-Narayan SV, et al. 2020 ESC guidelines for the management of adult congenital heart disease. Eur Heart J. 2021 Feb 11;42(6):563-645.Texto completo Resumo
Artigos de referência
Uma lista completa das fontes referenciadas neste tópico está disponível para os usuários com acesso total ao BMJ Best Practice.
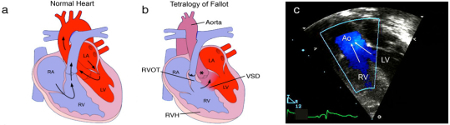
Diagnósticos diferenciais
- Other cyanotic congenital cardiac abnormalities
- Pulmonary stenosis
- Ventricular septal defect (VSD)
Mais Diagnósticos diferenciaisDiretrizes
- ACR Appropriateness Criteria: congenital or acquired heart disease
- Recommendations for the adult cardiac sonographer performing echocardiography to screen for critical congenital heart disease in the newborn
Mais DiretrizesConectar-se ou assinar para acessar todo o BMJ Best Practice
O uso deste conteúdo está sujeito ao nosso aviso legal