შეჯამება
განსაზღვრება
ანამნეზი და გასინჯვა
ძირითადი დიაგნოსტიკური ფაქტორები
- diplopia
- eye misalignment
- amblyopia
სხვა დიაგნოსტიკური ფაქტორები
- abnormal eye movements
- visual confusion
- asthenopia
- intermittent closure of one eye
- cranial nerve palsy
რისკფაქტორები
- family history of strabismus
- prematurity
- low birth weight
- maternal smoking during pregnancy
- refractive error
დიაგნოსტიკური კვლევები
1-ად შესაკვეთი გამოკვლევები
- cover test
- simultaneous prism and cover test (SPCT)
- uncover test (UCT)
- alternate prism cover test (APCT)
- Hirschberg test
- Krimsky test
გასათვალისწინებელი კვლევები
- version testing
- duction testing
- forced duction testing
- CT or MRI of orbit
- MRI of brain
- CT chest
მკურნალობის ალგორითმი
primary strabismus
secondary strabismus
კონტრიბუტორები
ავტორები
Daniel J. Salchow, MD

Director
Pediatric Ophthalmology; Strabismus; Neuro-ophthalmology
Charité-Universitätsmedizin Berlin
Berlin
Germany
გაფრთხილება:
DJS declares that he has no competing interests.
რეცენზენტები
Donny W. Suh, MD, FAAP, MBA, FACS
Chief and Professor of Pediatric Ophthalmology and Strabismus
Department of Ophthalmology
University of California, Irvine
Irvine
CA
გაფრთხილება:
DWS declares that he has no competing interests.
Peter Tiffin, BMedSci(Hons), MBBS, FRCOphth
Ophthalmology Consultant
City Hospitals Sunderland
Sunderland
UK
გაფრთხილება:
PT declares that he has no competing interests.
Jonathan Smith, MBBS, MRCP, MRCOphth
Specialist Registrar in Ophthalmology
Ophthalmics
Royal Victoria Infirmary
Newcastle
UK
გაფრთხილება:
JS declares that he has no competing interests.
რეცენზენტების განცხადებები
BMJ Best Practice-ის თემების განახლება სხვადასხვა პერიოდულობით ხდება მტკიცებულებებისა და რეკომენდაციების განვითარების შესაბამისად. ქვემოთ ჩამოთვლილმა რეცენზენტებმა თემის არსებობის მანძილზე კონტენტს ერთხელ მაინც გადახედეს.
გაფრთხილება
რეცენზენტების აფილიაციები და გაფრთხილებები მოცემულია გადახედვის მომენტისთვის.
წყაროები
ძირითადი სტატიები
US Preventive Services Task Force. Vision in children ages 6 months to 5 years: screening. Sep 2017 [internet publication].სრული ტექსტი
Sprunger DT, Lambert SR, Hercinovic A, et al. Esotropia and exotropia preferred practice pattern®. Ophthalmology. 2023 Mar;130(3):P179-221.სრული ტექსტი აბსტრაქტი
Dagi LR, Velez FG, Holmes JM, et al. Adult strabismus preferred practice pattern®. Ophthalmology. 2024 Apr;131(4):P306-403.სრული ტექსტი
Hutchinson AK, Morse CL, Hercinovic A, et al. Pediatric eye evaluations preferred practice pattern. Ophthalmology. 2023 Mar;130(3):P222-70.სრული ტექსტი აბსტრაქტი
Cruz OA, Repka MX, Hercinovic A, et al. Amblyopia preferred practice pattern. Ophthalmology. 2023 Mar;130(3):P136-78.სრული ტექსტი აბსტრაქტი
გამოყენებული სტატიები
ამ თემაში მოხსენიებული წყაროების სრული სია ხელმისაწვდომია მომხმარებლებისთვის, რომლებსაც აქვთ წვდომა BMJ Best Practice-ის ყველა ნაწილზე.
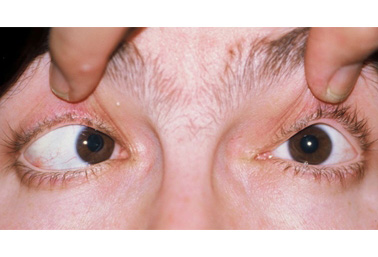
დიფერენციული დიაგნოზები
- Pseudostrabismus
- Blurred vision
- Monocular diplopia
მეტი დიფერენციული დიაგნოზებიგაიდლაინები
- Pediatric ophthalmology/strabismus summary benchmarks
- Adult strabismus summary benchmarks
მეტი გაიდლაინებიშედით სისტემაში ან გამოიწერეთ BMJ Best Practice
ამ მასალის გამოყენება ექვემდებარება ჩვენს განცხადებას