Resumo
Definição
História e exame físico
Principais fatores diagnósticos
- pain on swallowing
- fever (>100.5°F [>38°C])
- tonsillar exudate
Outros fatores diagnósticos
- sudden onset of sore throat
- headache
- abdominal pain
- nausea and vomiting
- presence of cough or runny nose
- tonsillar erythema
- tonsillar enlargement
- enlarged anterior cervical lymph nodes
Fatores de risco
- age between 5 and 15 years
- contact with infected people in enclosed spaces (e.g., child care centers, schools, prison)
Investigações diagnósticas
Primeiras investigações a serem solicitadas
- throat culture
- rapid streptococcal antigen test
Investigações a serem consideradas
- serologic testing for streptococci
- WBC count and differential
- heterophile antibodies
- vaginal and cervical, or penile, and rectal cultures
- HIV viral load assay
- lateral cervical view x-ray, exposed for soft tissue
Algoritmo de tratamento
acute tonsillitis not due to group A beta-hemolytic streptococcal infection
acute tonsillitis due to group A beta-hemolytic streptococcal infection
recurrent episodes of tonsillitis
Colaboradores
Autores
Christos Georgalas, PhD, DLO, FRCS (ORL-HNS)

Professor of Surgery - Head and Neck
University of Nicosia
Cyprus
Declarações
CG declares that he has no competing interests.
Eleftherios Margaritis, PhD, MSc, MD

Otolaryngologist - Head and Neck Surgeon
Collaborator in Otolaryngology
ENT Department
Hippokration University Hospital
Athens
Greece
Declarações
EM declares that he has no competing interests.
Revisores
Itzhak Brook, MD, MSc
Professor of Pediatrics and Medicine
Georgetown University
Washington
DC
Declarações
IB declares that he has no competing interests.
Chris Del Mar, MB BChir, FRACGP MD, MA, FAFPHM
Dean
Faculty of Health Sciences and Medicine
Bond University
Gold Coast
Queensland
Australia
Declarações
CDM is an author of a number of references cited in this topic.
Créditos aos pareceristas
Os tópicos do BMJ Best Practice são constantemente atualizados, seguindo os desenvolvimentos das evidências e das diretrizes. Os pareceristas aqui listados revisaram o conteúdo pelo menos uma vez durante a história do tópico.
Declarações
As afiliações e declarações dos pareceristas referem--se ao momento da revisão.
Referências
Principais artigos
Shaikh N, Swaminathan N, Hooper EG, et al. Accuracy and precision of the signs and symptoms of streptococcal pharyngitis in children: a systematic review. J Pediatr. 2012 Mar;160(3):487-93. Resumo
Aalbers J, O'Brien KK, Chan WS, et al. Predicting streptococcal pharyngitis in adults in primary care: a systematic review of the diagnostic accuracy of symptoms and signs and validation of the Centor score. BMC Med. 2011 Jun 1;9:67.Texto completo Resumo
Spinks A, Glasziou PP, Del Mar CB. Antibiotics for sore throat. Cochrane Database Syst Rev. 2013;(11):CD000023.Texto completo Resumo
Shulman ST, Bisno AL, Clegg HW, et al. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clin Infect Dis. 2012 Nov 15;55(10):e86-102.Texto completo Resumo
de Cassan S, Thompson MJ, Perera R, et al. Corticosteroids as standalone or add-on treatment for sore throat. Cochrane Database Syst Rev. 2020 May 1;5(5):CD008268.Texto completo Resumo
Burton MJ, Glasziou PP, Chong LY, et al. Tonsillectomy or adenotonsillectomy versus non-surgical treatment for chronic/recurrent acute tonsillitis. Cochrane Database Syst Rev. 2014 Nov 19;(11):CD001802.Texto completo Resumo
Windfuhr JP, Toepfner N, Steffen G, et al. Clinical practice guideline: tonsillitis II. Surgical management. Eur Arch Otorhinolaryngol. 2016 Apr;273(4):989-1009. Resumo
Artigos de referência
Uma lista completa das fontes referenciadas neste tópico está disponível para os usuários com acesso total ao BMJ Best Practice.
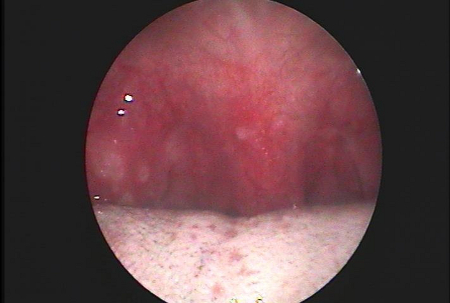
Diagnósticos diferenciais
- Infectious mononucleosis
- Epiglottitis
- Peritonsillar abscess (quinsy)
Mais Diagnósticos diferenciaisDiretrizes
- Clinical practice guideline: tonsillectomy in children (update)
- A guide to utilization of the microbiology laboratory for diagnosis of infectious diseases: 2018 update
Mais DiretrizesFolhetos informativos para os pacientes
Sore throat
Tonsillitis
Mais Folhetos informativos para os pacientesCalculadoras
Sore Throat (Pharyngitis) Evaluation and Treatment Criteria (McIsaac)
Mais CalculadorasConectar-se ou assinar para acessar todo o BMJ Best Practice
O uso deste conteúdo está sujeito ao nosso aviso legal