Резюме
Определение
Анамнез и осмотр
Ключевые диагностические факторы
- insidious onset
- well-localized tenderness
Другие диагностические факторы
- pain during activity
- tendon thickening
- tendon nodularity
- crepitus
Факторы риска
- athletic training
- unsuitable equipment
- hard and high-friction playing surface
- increasing age
- fluoroquinolone treatment
Диагностические исследования
Исследования, которые показаны в первую очередь
- clinical diagnosis
Исследования, проведение которых нужно рассмотреть
- ultrasound
- MRI
- x-ray
Алгоритм лечения
shoulder with rotator cuff tendinopathy
shoulder with biceps tendinopathy
elbow with lateral epicondylitis
elbow with medial epicondylitis
knee with patellar tendinopathy
knee with quadriceps, iliotibial band, or popliteus tendinopathy
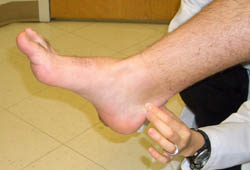
ankle with Achilles tendinopathy
Составители
Авторы
James H-C. Wang, PhD

Professor and Director
MechanoBiology Laboratory
Department of Orthopaedic Surgery
University of Pittsburgh School of Medicine
Pittsburgh
PA
Раскрытие информации
JHW declares that he has no competing interests.
Benjamin B. Rothrauff, MD, PhD
Research Fellow
UPMC Center for Sports Medicine
University of Pittsburgh
Pittsburgh
PA
Раскрытие информации
BBR declares that he has no competing interests.
Kevin J. Byrne, MD
Research Fellow
UPMC Center for Sports Medicine
University of Pittsburgh
Pittsburgh
PA
Раскрытие информации
KJB declares that he has no competing interests.
Выражение благодарностей
Dr James H-C. Wang, Dr Benjamin B. Rothrauff, and Dr. Kevin J. Byrne would like to gratefully acknowledge Dr Kivanc Atesok, Dr Chad Griffith, Dr Garth N. Walker, Dr Chealon Miller, Dr Paulo H. Araujo, Dr Margaret S. Lo, Dr Márcio Albers, and Dr Freddie H. Fu, previous contributors to this topic. Unfortunately, we have since been made aware that Dr Freddie H. Fu is deceased.
Раскрытие информации
KA, CG, GNW, CM, PHA, MSL, and MA declare that they have no competing interests. FHF declared that he had no competing interests.
Рецензенты
Per Renström, MD
Professor Emeritus
Karolinska Institute
Stockholm
Sweden
Раскрытие информации
PR declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
Список литературы
Основные статьи
Almekinders LC, Temple JD. Etiology, diagnosis, and treatment of tendonitis: an analysis of the literature. Med Sci Sports Exerc. 1998 Aug;30(8):1183-90. Аннотация
Beaudreuil J, Dhénain M, Coudane H, et al. Clinical practice guidelines for the surgical management of rotator cuff tears in adults. Orthop Traumatol Surg Res. 2010 Apr;96(2):175-9.Полный текст Аннотация
Schepsis AA, Jones H, Haas AL. Achilles tendon disorders in athletes. Am J Sports Med. 2002 Mar-Apr;30(2):287-305. Аннотация
Kukkonen J, Joukainen A, Lehtinen J, et al. Treatment of nontraumatic rotator cuff tears: a randomized controlled trial with two years of clinical and imaging follow-up. J Bone Joint Surg Am. 2015 Nov 4;97(21):1729-37. Аннотация
Статьи, указанные как источники
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Отличия
- Rotator cuff tear
- Osgood-Schlatter disease
- Sinding-Larsen-Johansson disease
Больше ОтличияРекомендации
- ACR appropriateness criteria: chronic shoulder pain
- ACR appropriateness criteria: chronic elbow pain
Больше РекомендацииЛифлеты для пациента
Rotator cuff injury
Больше Лифлеты для пациентаВойдите в учетную запись или оформите подписку, чтобы получить полноценный доступ к BMJ Best Practice
Использование этого контента попадает под действие нашего заявления об отказе от ответственности