FDA approves new oral antibiotics effective against resistant strains of gonorrhea
Two new oral antibiotics, zoliflodacin and gepotidacin, have been approved by the Food and Drug Administration (FDA) for treating patients with uncomplicated urogenital gonorrhea in patients age 12 years and older. The gepotidacin approval is restricted to patients with few or no other treatment choices because of limited safety data.
Zoliflodacin and gepotidacin have novel mechanisms of action, which means they are effective against strains of Neisseria gonorrhoeae that are resistant to currently recommended antibiotics. Gepotidacin and zoliflodacin act by inhibiting bacterial DNA replication.
The new antibiotics provide oral treatment options and alternative treatments for resistant strains of N gonorrhoeae.
Summary
Definition
History and exam
Key diagnostic factors
- urethral discharge
- urethral irritation or itching
- dysuria
Other diagnostic factors
- orchialgia
- absence of epididymal tenderness and/or swelling
- absence of pelvic pain (women)
- absence of pustular or petechial rash
- absence of arthritis
- absence of eye inflammation
Risk factors
- ages 15 to 24 years
- female sex
- men who have sex with men
- new or multiple sex partners
- prior or current STI
- inconsistent condom use
- circumcision
Diagnostic tests
1st tests to order
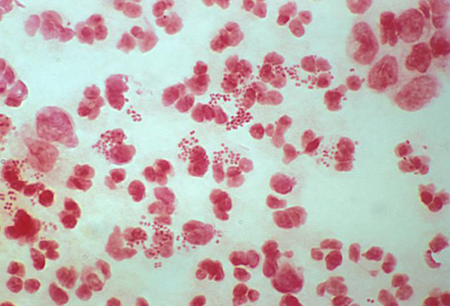
- Gram stain of urethral discharge and/or urine sediment
- nucleic acid amplification tests (NAAT)
- culture of urethral discharge
- potassium hydroxide prep of urethral discharge
- HIV test
- syphilis test
Tests to consider
- urinalysis and culture
- wet mount of urethral discharge (women)
- NAAT and culture of urine or urethral/vaginal swab for Trichomonas vaginalis
- NAAT for other organisms
Treatment algorithm
initial Gram stain suggestive of gonorrhea: nonpregnant
initial Gram stain suggestive of gonorrhea: pregnant
initial Gram stain not suggestive of gonorrhea: nonpregnant
initial Gram stain not suggestive of gonorrhea: pregnant
recurrent or resistant urethritis
Contributors
Authors
Sheldon Morris, MD, MPH
Assistant Professor
Division of Infectious Diseases
Department of Medicine
UCSD Antiviral Research Center
Division of Family Medicine
Department of Family and Preventive Medicine
UCSD La Jolla Family and Sports Medicine
San Diego, CA
Disclosures
SM has received funding from NIH, CHRP, CIRM, NASA, and Visby Medical. SM owns stock in Bristol Myers Squib and is the founder of Aspera Biomedicines. SM is an author of a number of references cited in this topic.
Acknowledgements
Dr Sheldon Morris would like to gratefully acknowledge Dr Christina Bailey, a previous contributor to this topic.
Disclosures
CB declares that she has no competing interests.
Peer reviewers
Vani Dandolu, MD, MPH
Associate Professor
Ob/Gyn and Urology
Director
Division of Urogynecology
Associate Residency Program Director
Temple University Hospital
Philadelphia, PA
Disclosures
VD declares that he has no competing interests.
Khalil Ghanem, MD, PhD
Assistant Professor of Medicine
Associate Fellowship Program Director
Division of Infectious Diseases
Johns Hopkins University School of Medicine
Baltimore, MD
Disclosures
KG declares that he has no competing interests.
Christopher Fairley, PhD
Professor of Sexual Health
University of Melbourne
Director
Melbourne Sexual Health Centre
Carlton
Victoria
Australia
Disclosures
CF is an author of a number of references cited in this topic. CF has received program grants of 6 figures US$.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Centers for Disease Control and Prevention. Sexually transmitted infections treatment guidelines, 2021. Jul 2021 [internet publication].Full text
Centers for Disease Control and Prevention. National overview of STIs in 2023. Nov 2024 [internet publication].Full text
European Association of Urology. Guidelines on urological infections. 2023 [internet publication].Full text
Horner PJ, Blee K, Falk L, et al; International Union against Sexually Transmitted Infections. 2016 European guideline on the management of non-gonococcal urethritis. Int J STD AIDS. 2016 Oct;27(11):928-37.Full text
British Association for Sexual Health and HIV. Urethritis and cervicitis. May 2023 [internet publication].Full text
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Urinary tract infection
- Candida balanitis or vaginitis
- Noninfectious urethritis
More DifferentialsGuidelines
- Guidelines on urological infections
- 2021 European guideline on Mycoplasma genitalium infections
More GuidelinesPatient information
Chlamydia
Gonorrhea
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer
