Summary
Differentials
Common
- Bacterial vaginosis
- Trichomoniasis
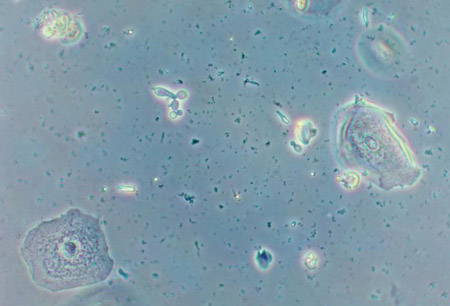
- Vulvovaginal candidiasis
- Chlamydia trachomatis infection
- Neisseria gonorrhoeae infection
- Mycoplasma genitalium
- Irritant and allergic vaginitis
- Physiologic discharge in adults
- Foreign body in children
- Nonspecific vaginitis
- Physiologic discharge in children
Uncommon
- Herpes simplex virus (HSV) infection
- Streptococcal vaginitis in adults
- Genital schistosomiasis
- Entamoeba gingivalis plus intrauterine device (IUD)
- Inadequate hygiene
- Foreign body in adults
- Combined contraceptive or hormonal vaginal ring-related
- Genitourinary syndrome of menopause
- Postpuerperal atrophic vaginitis; lochia
- Behcet syndrome
- Desquamative inflammatory vaginitis
- Erosive lichen planus
- Postoperative sling/mesh procedure
- Postradiation
- Cervical cancer
- Carcinoma of the fallopian tube
- Pinworm infection
- Streptococcal vaginitis in children
- Sexual abuse
- Transmitted maternal birth canal infection
- Prolapsing fibroid
- Vaginal fistula
- Lymphoma of genital tract
Contributors
Authors
Jenell S. Coleman, MD, MPH, FACOG
Associate Professor
Division Director, Gynecologic Specialties
Medical Director, JHOC Women’s Health Center
Director, JHOC Resident Continuity Clinic
Co-Director, JHOC Colposcopy Clinic
Department of Gynecology & Obstetrics
Johns Hopkins University School of Medicine
Baltimore
MD
Disclosures
JC is an author of a reference cited in this topic and received research grants from Hologic, Gilead, and Merck.
Acknowledgements
Dr Jenell Coleman would like to gratefully acknowledge Dr Veronica Gomez-Lobo and Dr Isabelle Guichard, previous contributors to this topic.
Disclosures
VGL and IG declare that they have no competing interests.
Peer reviewers
Susie Logan, MB ChB, MD, FRCOG, FFSRH
Senior Consultant, Department of Obstetrics and Gynaecology, National University Hospital, NUHS
Director of Residency Obstetrics and Gynaecology, National University Hospital, NUHS
Co-Lead for Women's Health, Alexandra Hospital
Assistant Professor, National University of Singapore
Singapore
Disclosures
SL is a member of the Examination Committee of the Membership of the Faculty of Sexual and Reproductive Healthcare of the Royal College of Obstetricians and Gynaecologists.
David Chelmow, MD
Chair
Department of Obstetrics and Gynecology
Virginia Commonwealth University
Richmond
VA
Disclosures
DC declares that he has no competing interests.
Lesley Bacon, FFSRH, MRCGP
Consultant in Sexual and Reproductive Health
Lewisham Primary Care Trust
Waldron Health Centre
London
UK
Disclosures
LB was a member of the group that produced the 2006 Faculty of Sexual and Reproductive Health guidance on the management of women with vaginal discharge presenting in a non-genitourinary setting.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Centers for Disease Control and Prevention. Sexually transmitted infections treatment guidelines, 2021. Jul 2021 [internet publication].Full text
Sherrard J, Wilson J, Donders G, et al. 2018 European (IUSTI/WHO) International Union against sexually transmitted infections (IUSTI) World Health Organisation (WHO) guideline on the management of vaginal discharge. Int J STD AIDS. 2018 Nov;29(13):1258-72. Abstract
Miller JM, Binnicker MJ, Campbell S, et al. Guide to utilization of the microbiology laboratory for diagnosis of infectious diseases: 2024 update by the Infectious Diseases Society of America (IDSA) and the American Society for Microbiology (ASM). Clin Infect Dis. 2024 Mar 5:ciae104.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Patient information
Chlamydia
Genital herpes
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer