Summary
Definition
History and exam
Key diagnostic factors
- painful and tender joints
- osteoarthritis-like involvement of joints (wrists, shoulders)
- sudden worsening of osteoarthritis
Other diagnostic factors
- red and swollen joints
- joint effusion and fluctuance
- fever and malaise
Risk factors
- advanced age
- injury
- hyperparathyroidism
- hemochromatosis
- family history of CPPD
- hypomagnesemia
- hypophosphatasia
- gout
- other metabolic conditions
Diagnostic tests
1st tests to order
- arthrocentesis with synovial fluid analysis
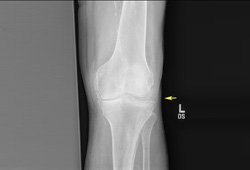
- radiographs of affected joints
- serum calcium
- serum parathyroid hormone
- iron studies
- serum magnesium
- serum alkaline phosphatase
Tests to consider
- ultrasonography
- CT scan
Treatment algorithm
mono- or oligoarticular disease
polyarticular disease
chronic recurrent involvement of knee, hip, or shoulder joint with severe degeneration
with osteoarthritis-like disease or rheumatoid-like disease
Contributors
Authors
Ann K. Rosenthal, MD

Professor of Medicine
Medical College of Wisconsin
Milwaukee
WI
Disclosures
AKR is the author of several articles cited in this topic.
Peer reviewers
Priyanka Iyer, MD
Clinical Assistant Professor
University of California, Irvine
Irvine
CA
Disclosures
PI declares that she has no competing interests.
Ade Adebajo, MBBS, MSc, FRCP (Glasgow), FACP
Consultant Rheumatologist
Rheumatology
University of Sheffield Medical School
Sheffield
UK
Disclosures
AA declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
McCarty DJ. Diagnostic mimicry in arthritis: patterns of joint involvement associated with calcium pyrophosphate dihydrate crystal deposits. Bull Rheum Dis. 1975;25:804-809.
Zhang W, Doherty M, Bardin T, et al. European League Against Rheumatism recommendations for calcium pyrophosphate deposition. Part I: terminology and diagnosis. Ann Rheum Dis. 2011 Apr;70(4):563-70.Full text Abstract
Rosenthal AK, Ryan LM. Calcium Pyrophosphate Deposition Disease. N Engl J Med. 2016 Jun 30;374(26):2575-84.Full text Abstract
Martinez Sanchis A, Pascual E. Intracellular and extracellular CPPD crystals are a regular feature in synovial fluid from uninflamed joints of patients with CPPD related arthropathy. Ann Rheum Dis. 2005 Dec;64(12):1769-72. Abstract
Zhang W, Doherty M, Pascual E, et al. EULAR recommendations for calcium pyrophosphate deposition. Part II: management. Ann Rheum Dis. 2011 Apr;70(4):571-5.Full text Abstract
Creamer P. Intra-articular corticosteroid treatment in osteoarthritis. Curr Opin Rheumatol. 1999 Sep;11(5):417-21. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Acute gouty arthritis
- Acute septic arthritis
- Milwaukee shoulder syndrome
More DifferentialsGuidelines
- European League Against Rheumatism recommendations for calcium pyrophosphate deposition. Part I: terminology and diagnosis
- EULAR recommendations for calcium pyrophosphate deposition. Part II: management
More GuidelinesVideos
Aspiration and injection of the knee: animated demonstration
More videosLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer