Summary
Definition
History and exam
Key diagnostic factors
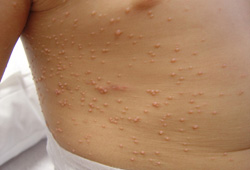
- pearly papule with a central dell
Other diagnostic factors
- surrounding erythema
- facial or groin distribution of lesions
- pruritus
- atopic dermatitis
- sleep disturbance
Risk factors
- close contact with an infected individual
- sexual contact with an infected individual
- atopic dermatitis
- immunocompromise
- tropical climate
- swimming
Diagnostic tests
Tests to consider
- dermoscopy
- curettage biopsy
- hematoxylin and eosin staining
- full sexual health screen including HIV test
Treatment algorithm
immunocompetent
immunocompromised
Contributors
Authors
Nicholas Francis, PhD, MD, BA, MRCGP
Professor of Primary Care Research
Primary Care Research Centre
School of Primary Care, Population Sciences and Medical Education
University of Southampton
Southampton
UK
Disclosures
NF declares that he has no competing interests.
Acknowledgements
Dr Nicholas Francis would like to gratefully acknowledge Dr Nanette B. Silverberg, a previous contributor to this topic.
Disclosures
NBS declares that she has no competing interests.
Peer reviewers
David M. Ozog, MD
Director of Cosmetic Dermatology
Department of Dermatology
Cosmetic and Procedural Dermatology
Henry Ford Health System
Detroit
MI
Disclosures
DMO declares that he has no competing interests.
Anthony Ormerod, MB, ChB, MRCP, FRCP(Edin), MD, FRCP(Lond)
Consultant Dermatologist
Aberdeen Royal Infirmary
Aberdeen
UK
Disclosures
None disclosed.
Andrea Bershow, MD
Staff Dermatologist
VA Medical Center
Minneapolis
MN
Disclosures
AB declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Fernando I, K Edwards S, Grover D. British Association for Sexual Health and HIV national guideline for the management of genital molluscum in adults (2021). Int J STD AIDS. 2022 Apr;33(5):422-32. Abstract
Edwards S, Boffa MJ, Janier M, et al. 2020 European guideline on the management of genital molluscum contagiosum. J Eur Acad Dermatol Venereol. 2021 Jan;35(1):17-26.Full text Abstract
van der Wouden JC, van der Sande R, Kruithof EJ, et al. Interventions for cutaneous molluscum contagiosum. Cochrane Database Syst Rev. 2017 May 17;(5):CD004767.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Warts
- Deep fungal infection (Cryptococcosis and Penicillium marneffei)
- Herpes simplex virus
More DifferentialsGuidelines
- UK national guideline for the management of genital molluscum in adults
- 2020 European guideline on the management of genital molluscum contagiosum
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer