Summary
Definition
History and exam
Key diagnostic factors
- cirrhosis
- severe liver disease
- alcohol misuse
- hepatitis B or C infection
- ascites
- spider angioma
- caput medusa
- jaundice
- encephalopathy
- hematemesis
- melena
- hematochezia
- HIV coinfection
Other diagnostic factors
- splenomegaly
Risk factors
- portal hypertension
- size of varices
- red wale marks
- decompensated cirrhosis
- ascites
Diagnostic investigations
1st investigations to order
- hepatic venous pressure gradient (HPVG)
- complete blood count
- coagulation profile (INR/prothrombin time)
- serum LFTs
- BUN and creatinine
- blood typing/cross-matching
- hepatitis B surface antigen (HBsAg)
- anti-hepatitis C virus IgG (anti-HCV IgG)
- esophago-gastro-duodenoscopy (EGD)
- liver stiffness measurement (LSM)
Emerging tests
- capsule endoscopy
Treatment algorithm
decompensated cirrhosis with acute variceal hemorrhage (hepatic venous pressure gradient ≥10 mmHg)
decompensated cirrhosis with acute variceal hemorrhage and failed endoscopic/pharmacologic therapy
compensated cirrhosis with mild portal hypertension (hepatic venous pressure gradient >5 and <10 mmHg)
compensated cirrhosis with clinically significant portal hypertension (hepatic venous pressure gradient ≥10 mmHg): without gastroesophageal varices
compensated cirrhosis with clinically significant portal hypertension (hepatic venous pressure gradient ≥10 mmHg): with gastroesophageal varices (no bleeding)
previous variceal bleed
Contributors
Expert advisers
Savio John, MD, AGAF, FACG
Chief (Division of Gastroenterology), Director (Hepatology), Associate Professor
Department of Medicine
State University of New York Upstate Medical University
Syracuse, NY
Disclosures
SJ serves as editor of the hepatology section for Stat Pearls.
Kelita Singh, MD
Associate Professor of Medicine
Department of Gastroenterology
State University of New York Upstate Medical University
Syracuse, NY
Disclosures
KS declares that she has no competing interests.
Acknowledgements
Dr Savio John and Dr Keilita Singh would like to gratefully acknowledge Dr Grace E. Dolman, Dr Gennaro D'Amico, Dr Giuseppe Malizia, Dr Vikram Boolchand, and Dr Thomas Boyer, previous contributors to this topic.
Disclosures
GED, GDA, GM, VB, and TB declare that they have no competing interests.
Peer reviewers
Shreyas Saligram, MD, MRCP, FACG, FASGE
Assistant Professor
Department of Gastroenterology
University of California
San Francisco, CA
Disclosures
SS declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Kaplan DE, Ripoll C, Thiele M, et al. AASLD practice guidance on risk stratification and management of portal hypertension and varices in cirrhosis. Hepatology. 2024 May 1;79(5):1180-211.Full text Abstract
de Franchis R, Bosch J, Garcia-Tsao G, et al. Baveno VII - renewing consensus in portal hypertension. J Hepatol. 2022 Apr;76(4):959-74.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
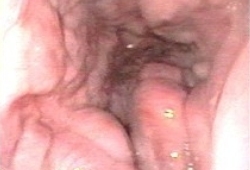
Differentials
- Hiatal hernia
- Gastric varices
- Mallory-Weiss tear
More DifferentialsGuidelines
- AASLD practice guidance on risk stratification and management of portal hypertension and varices in cirrhosis
- American College of Gastroenterology–Canadian Association of Gastroenterology clinical practice guideline: management of anticoagulants and antiplatelets during acute gastrointestinal bleeding and the periendoscopic period
More GuidelinesCalculators
Child Pugh classification for severity of liver disease
More CalculatorsPatient information
Hepatitis B: should I have the vaccine?
Hepatitis C: what is it?
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer