Resumo
Definição
História e exame físico
Principais fatores diagnósticos
- nausea and vomiting
- abdominal distention
- no features of mechanical obstruction or peritoneal inflammation (e.g., abdominal hernia, peritoneal signs)
Outros fatores diagnósticos
- obstipation (severe constipation with no passage of stool or flatus)
- discomfort and abdominal cramping
- decreased or hypoactive bowel sounds
- hypovolemia
Fatores de risco
- abdominal surgery
- acute/systemic illness (e.g., myocardial infarction, pneumonia, acute cholecystitis, pancreatitis, sepsis, multi-organ trauma)
- nonabdominal surgery
- electrolyte imbalance
- opioid analgesics, anticholinergics, or anesthetic gases
- comorbidities (e.g., diabetes mellitus, cardiovascular insufficiency, Chagas disease, scleroderma)
Investigações diagnósticas
Primeiras investigações a serem solicitadas
- serum electrolytes
- serum magnesium
- CBC
- abdomen and pelvis CT scan (with intravenous contrast and oral water soluble contrast)
Investigações a serem consideradas
- serum LFTs
- serum amylase
- serum lipase
- small bowel series
- gastric emptying study
Algoritmo de tratamento
postoperative ileus
nonsurgical cause
ileus lasting longer than 3 days or prolonging the postoperative recovery
Colaboradores
Consultores especialistas
Steven D. Wexner, MD, PhD (Hon), FACS, FRCS (Eng), FRCS (Ed), FRCSI (Hon)
Director
Digestive Disease Center
Professor and Chair
Department of Colorectal Surgery
Cleveland Clinic
Weston, FL
Declarações
SDW has received consulting fees, stock options, and royalties from the following companies. These relationships are ongoing. Consulting: ICON Language Services, Intuitive Surgical, Stryker, Medtronic, Takeda, ARC/Corvus, Astellas, Baxter, Olympus, AIS Channel, Livsmed. Royalties: Medtronic, Intuitive Surgical, Karl Storz Endoscopy-America, Unique Surgical Innovations. Stock Options: Regentys, LifeBond, Pragma/GibLib, and Renew Medical.
Sameh Hany Emile Rizkalla, MBBCh, MSc, MD, FACS
Research associate, Colorectal Surgery Department
Digestive Disease Center
Professor and Chair
Department of Colorectal Surgery
Cleveland Clinic
Weston, FL
Declarações
SHER declares that he has no competing interests.
Agradecimentos
Dr Steven D. Wexner would like to gratefully acknowledge the contribution of Dr Stephen P. Sharp to the update for this topic. Dr Wexner would also like to acknowledge Dr Ahmed Sami Chadi, and Dr Paula I. Denoya, previous contributors to this topic.
Declarações
SPS, ASC, and PID declare that they have no competing interests.
Revisores
David J. Hackam, MD, PhD
Associate Professor of Pediatric Surgery
University of Pittsburgh School of Medicine
Pittsburgh, PA
Declarações
DJH declares that he has no competing interests.
John Jenkins, MB CHB, FRCP
Consultant Colorectal Surgeon
St. Mark's Hospital
Harrow
UK
Declarações
JJ declares that he has no competing interests.
Créditos aos pareceristas
Os tópicos do BMJ Best Practice são constantemente atualizados, seguindo os desenvolvimentos das evidências e das diretrizes. Os pareceristas aqui listados revisaram o conteúdo pelo menos uma vez durante a história do tópico.
Declarações
As afiliações e declarações dos pareceristas referem--se ao momento da revisão.
Referências
Principais artigos
Wattchow D, Heitmann P, Smolilo D, et al. Postoperative ileus- an ongoing conundrum. Neurogastroenterol Motil. 2021 May;33(5):e14046. Resumo
Gustafsson UO, Scott MJ, Hubner M, et al. Guidelines for perioperative care in elective colorectal surgery: Enhanced Recovery After Surgery (ERAS(®)) Society recommendations: 2018. World J Surg. 2019 Mar;43(3):659-95.Texto completo Resumo
American College of Radiology. ACR appropriateness criteria: suspected small-bowel obstruction. 2019 [internet publication].Texto completo
Artigos de referência
Uma lista completa das fontes referenciadas neste tópico está disponível para os usuários com acesso total ao BMJ Best Practice.
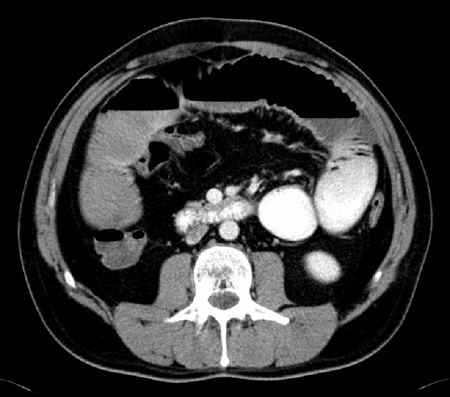
Diagnósticos diferenciais
- Mechanical bowel obstruction
- Pseudo-obstruction (Ogilvie syndrome)
- Gastroenteritis
Mais Diagnósticos diferenciaisDiretrizes
- ACR appropriateness criteria: suspected small-bowel obstruction
- Guidelines for perioperative care in elective colorectal surgery
Mais DiretrizesVideos
Nasogastric tube insertion animated demonstration
Mais vídeosConectar-se ou assinar para acessar todo o BMJ Best Practice
O uso deste conteúdo está sujeito ao nosso aviso legal