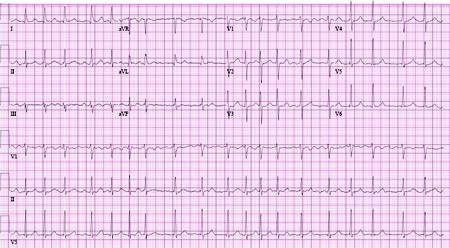
Resumo
Definição
História e exame físico
Principais fatores diagnósticos
- worsening heart failure or pulmonary symptoms
- jugular venous pulsations with rapid flutter waves
Outros fatores diagnósticos
- palpitations
- fatigue or lightheadedness
- chest pain
- dyspnea
- syncope
- hypotension
- embolic events
Fatores de risco
- increasing age
- valvular dysfunction
- atrial septal defects
- atrial dilation
- recent cardiac or thoracic procedures
- surgical or postablation scarring of atria
- heart failure
- hyperthyroidism
- COPD
- asthma
- pneumonia
- antiarrhythmics for atrial fibrillation
- diabetes
- digitalis use
- male sex
- congenital or lone atrial flutter
Investigações diagnósticas
Primeiras investigações a serem solicitadas
- ECG
- thyroid function tests
- serum electrolytes
Tests to avoid
- imaging stress tests
- coronary CT angiography
Investigações a serem consideradas
- pulmonary function tests
- CXR
- digitalis level
- cardiac enzymes
- spiral CT with pulmonary embolism protocol
- transthoracic echocardiogram
- atrial electrogram recording
- electrophysiologic studies
Algoritmo de tratamento
hemodynamically unstable
hemodynamically stable
recurrent atrial flutter or failure of elective cardioversion
Colaboradores
Consultores especialistas
Komandoor Srivathsan, MD
Cardiac Electrophysiologist, Cardiologist
Mayo Clinic
Phoenix, AZ
Declarações
KS declares that he has no competing interests.
Sai Anil Kumar Sriramoju, MD
Cardiovascular Disease Fellow
Garden City Hospital
Garden City, MI
Declarações
SAKS declares that he has no competing interests.
Acknowledgement
BMJ Best Practice would like to gratefully acknowledge the previous expert contributor, whose work has been retained in parts of the content:
Katherine C. Wu MD, FACC
Associate Professor of Medicine
Johns Hopkins University
School of Medicine
Baltimore, MD
Declarações
KCW declares that she has no competing interests.
Revisores
Richard C. Wu, MD
Associate Professor of Medicine
Director
Cardiac Electrophysiology Laboratory
UT Southwestern Medical Center
University Hospital
St. Paul
Dallas, TX
Declarações
RCW declares that he has no competing interests.
Reginald Ho, MD
Clinical Assistant Professor
Department of Medicine
Thomas Jefferson University Hospital
Philadelphia, PA
Declarações
RH declares that he has no competing interests.
George Juang, MD, FACC
Director of Electrophysiology
Long Island Arrhythmia Center
Mineola, NY
Declarações
GJ declares that he has no competing interests.
Créditos aos pareceristas
Os tópicos do BMJ Best Practice são constantemente atualizados, seguindo os desenvolvimentos das evidências e das diretrizes. Os pareceristas aqui listados revisaram o conteúdo pelo menos uma vez durante a história do tópico.
Declarações
As afiliações e declarações dos pareceristas referem--se ao momento da revisão.
Referências
Principais artigos
Page RL, Joglar JA, Caldwell MA, et al. 2015 ACC/AHA/HRS guideline for the management of adult patients with supraventricular tachycardia. J Am Coll Cardiol. 2016 Apr 5;67(13):e27-115.Texto completo Resumo
Joglar JA, Chung MK, Armbruster AL, et al. 2023 ACC/AHA/ACCP/HRS guideline for the diagnosis and management of atrial fibrillation: a report of the American College of Cardiology/American Heart Association Joint Committee on clinical practice guidelines. Circulation. 2024 Jan 2;149(1):e1-156.Texto completo Resumo
Van Gelder IC, Rienstra M, Bunting KV, et al. 2024 ESC guidelines for the management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J. 2024 Sep 29;45(36):3314-414.Texto completo Resumo
Artigos de referência
Uma lista completa das fontes referenciadas neste tópico está disponível para os usuários com acesso total ao BMJ Best Practice.
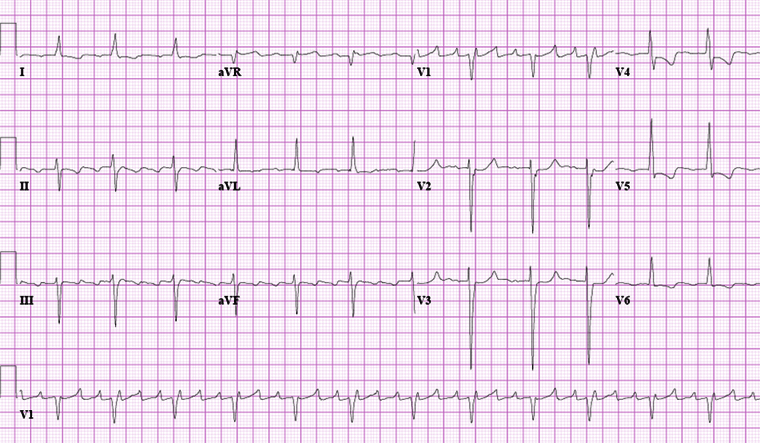
Diagnósticos diferenciais
- Atrial fibrillation
- Atrial tachycardia
Mais Diagnósticos diferenciaisDiretrizes
- 2024 ESC guidelines for the management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS)
- 2023 ACC/AHA/ACCP/HRS guideline for the diagnosis and management of atrial fibrillation
Mais DiretrizesCalculadoras
Atrial Fibrillation CHA(2)DS(2)-VASc Score for Stroke Risk
HAS-BLED Bleeding Risk Score
Mais CalculadorasVideos
Electrical (direct current) cardioversion animated demonstration
Mais vídeosFolhetos informativos para os pacientes
Atrial fibrillation: what is it?
Atrial fibrillation: what are the treatment options?
Mais Folhetos informativos para os pacientesConectar-se ou assinar para acessar todo o BMJ Best Practice
O uso deste conteúdo está sujeito ao nosso aviso legal