Summary
Definition
History and exam
Key diagnostic factors
- right upper quadrant (RUQ) or epigastric pain (lasting >30 minutes)
Other diagnostic factors
- postprandial pain
- RUQ or epigastric tenderness
- nausea
- jaundice
Risk factors
- increasing age
- female sex
- Hispanic and American Indian ethnicity
- family history of gallstones
- gene mutations
- elevated estrogen and progesterone levels
- obesity, diabetes, and metabolic syndrome
- nonalcoholic fatty liver disease
- prolonged fasting/rapid weight loss
- total parenteral nutrition (TPN)
- use of octreotide
- use of glucagon-like peptide-1 (GLP-1) receptor agonists
- use of ceftriaxone
- terminal ileum disease or resection
- hemoglobinopathy
- cirrhosis
- cystic fibrosis
- diet and lifestyle
- helicobacter pylori gallbladder infection
Diagnostic tests
1st tests to order
- abdominal ultrasound
- serum liver function tests
- CBC
- serum lipase or amylase
Tests to consider
- magnetic resonance cholangiopancreatography (MRCP)
- endoscopic ultrasound scan (EUS)
- endoscopic retrograde cholangiopancreatography (ERCP)
- abdominal CT scan
Treatment algorithm
symptomatic cholelithiasis
choledocholithiasis with or without symptoms
asymptomatic cholelithiasis
Contributors
Expert advisers
Eldon Shaffer, MD, FRCPC
Emeritus Professor of Medicine
Division of Gastroenterology
University of Calgary
Calgary
Canada
Disclosures
ES is an author of several references cited in this topic.
Acknowledgements
Professor Eldon Shaffer would like to gratefully acknowledge Dr Vikesh K. Singh and Dr Anthony N. Kalloo, previous contributors to this topic.
Disclosures
VKS and ANK declare that they have no competing interests.
Peer reviewers
Timothy B. Gardner, MD
Assistant Professor
Director of Pancreatic Disorders
Section of Gastroenterology
Dartmouth-Hitchcock Medical Center
Lebanon, NH
Disclosures
TBG declares that he has no competing interests.
Ajith Siriwardena, MD, FRCS
Professor of Hepatobiliary Surgery
Manchester Royal Infirmary
Manchester
UK
Disclosures
AS declares that he has no competing interests.
Kurinchi Gurusamy, MBBS, MS, MRCS, MSc
Clinical Research Fellow
Hepatopancreatobiliary and Liver Transplant Surgery
University Department of Surgery
Royal Free Campus
UCL Medical School
London
UK
Disclosures
KG declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
European Association for the Study of the Liver (EASL). EASL clinical practice guidelines on the prevention, diagnosis and treatment of gallstones. J Hepatol. 2016 Jul;65(1):146-81.Full text Abstract
ASGE Standards of Practice Committee; Buxbaum JL, Abbas Fehmi SM, Sultan S, et al. ASGE guideline on the role of endoscopy in the evaluation and management of choledocholithiasis. Gastrointest Endosc. 2019 Jun;89(6):1075-105;e15.Full text Abstract
Tazuma S, Unno M, Igarashi Y, et al. Evidence-based clinical practice guidelines for cholelithiasis 2016. J Gastroenterol. 2017 Mar;52(3):276-300.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
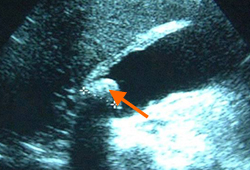
Differentials
- Acalculous cholecystitis
- Nonbiliary acute pancreatitis
- Peptic ulcer disease (PUD)
More DifferentialsGuidelines
- ACR appropriateness criteria: right upper quadrant pain
- 2020 World Society of Emergency Surgery updated guidelines for the diagnosis and treatment of acute calculus cholecystitis
More GuidelinesPatient information
Gallstones
Gallstones: questions to ask your doctor
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer